## Diagnosis: Stevens-Johnson Syndrome (SJS) **Key Point:** SJS is a severe cutaneous adverse reaction (SCAR) characterized by mucosal involvement, target lesions, and systemic toxicity. The patient's presentation — fever, oral erosions with crusting, target lesions, and temporal relationship to trimethoprim-sulfamethoxazole — is pathognomonic. **High-Yield:** The **RegiSCAR scoring system** confirms SJS when: - Mucosal involvement (mandatory for SJS/TEN) - Target lesions or atypical lesions with central blistering - Facial edema - Involvement of ≥2 mucosal sites - Fever ≥38.5°C - Lymphadenopathy - Leukocytosis or leukopenia ## Management Algorithm ```mermaid flowchart TD A[Suspected SJS/TEN]:::outcome --> B[Discontinue offending drug IMMEDIATELY]:::action B --> C[Supportive care]:::action C --> D[Fluid resuscitation & electrolyte correction]:::action D --> E[Analgesia, temperature control]:::action E --> F[Ophthalmology & ENT review]:::action F --> G{Systemic corticosteroids?}:::decision G -->|Controversial; consider early in SJS| H[Methylprednisolone 0.5-1 mg/kg/day]:::action G -->|Not recommended in TEN| I[Supportive care alone]:::action H --> J[Gradual taper over 6-8 weeks]:::action I --> J J --> K[Monitor for infection, fluid/electrolyte balance]:::action ``` ### Why Immediate Drug Withdrawal is Critical **Clinical Pearl:** The **single most important intervention** in SJS is **immediate discontinuation of the causative agent**. Continuing the drug dramatically worsens prognosis and increases mortality. In this case, trimethoprim-sulfamethoxazole is the likely culprit — sulfonamides are among the top 3 causes of SJS/TEN globally. ### Supportive Care Pillars | Intervention | Rationale | |---|---| | **IV fluids** | Prevent hypovolemic shock; target urine output 0.5–1 mL/kg/hr | | **Electrolyte correction** | Correct Na^+^, K^+^, Ca^2+^ losses from widespread erosions | | **Analgesia** | Severe mucosal pain impairs oral intake; use opioids if needed | | **Temperature management** | Fever increases metabolic demand and infection risk | | **Ophthalmology review** | Prevent cicatricial pemphigoid and blindness | | **Barrier nursing** | Minimize infection risk in denuded skin | **Warning:** Skin biopsy is NOT required for diagnosis in a classic presentation — it delays critical care. Histology (subepidermal blistering with full-thickness epidermal necrosis) confirms SJS but does not change acute management. **Mnemonic — SJS vs TEN (% BSA involvement):** **"SJS ≤10, TEN ≥30, Overlap 10–30"** ### Role of Systemic Corticosteroids **High-Yield:** The use of systemic corticosteroids in SJS remains **controversial** but is increasingly supported by retrospective data and expert consensus: - **Early use** (within 48–72 hours of onset) may reduce progression and mortality - **Dosing:** Methylprednisolone 0.5–1 mg/kg/day IV, then oral taper over 6–8 weeks - **Contraindication:** Avoid in TEN (>30% BSA) due to increased infection risk - **This patient has SJS** (mucosal involvement, <10% BSA likely), so corticosteroids are reasonable but NOT the **first** priority — drug withdrawal is **Tip:** In exam questions, the **correct answer hierarchy** for SJS management is: 1. **Discontinue the offending drug** (non-negotiable, immediate) 2. **Supportive care** (fluids, electrolytes, analgesia, barrier nursing) 3. **Consider early systemic corticosteroids** (if within 48–72 hours and SJS, not TEN) 4. **Specialist input** (ophthalmology, ENT, ICU) ### Why This Patient Needs Immediate Resuscitation - **BP 98/62 mmHg** = early shock; fluid resuscitation is urgent - **Creatinine 1.8 mg/dL** = acute kidney injury (likely prerenal from hypovolemia + direct tubular toxicity) - **Fever + tachycardia** = systemic inflammatory response [cite:Robbins 10e Ch 25] 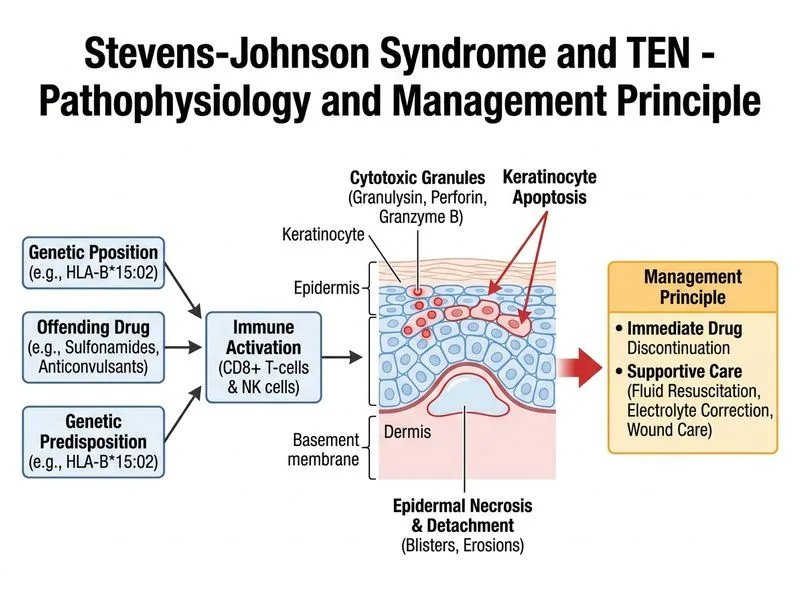
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.