## Diagnostic Approach to Stevens-Johnson Syndrome ### Histopathological Confirmation **Key Point:** Skin biopsy with histopathology is the gold standard for confirming SJS and differentiating it from other blistering disorders. ### Histological Features of SJS | Feature | Finding | |---------|----------| | **Epidermal necrosis** | Full-thickness or near-complete keratinocyte apoptosis | | **Dermal infiltrate** | Sparse to moderate lymphocytic infiltration | | **Blister formation** | Subepidermal or intraepidermal cleavage | | **Inflammatory pattern** | Interface dermatitis with minimal dermal inflammation | | **Immunoglobulin deposition** | Absent (unlike erythema multiforme) | ### Why Biopsy is Essential 1. **Distinguishes SJS from mimics:** - Erythema multiforme (EM): Has dermal inflammation with "full-house" pattern; SJS shows epidermal necrosis with sparse dermal infiltrate - Toxic epidermal necrolysis (TEN): Histology is identical to SJS; distinction is clinical (>30% BSA involvement = TEN) - Drug reaction with eosinophilia and systemic symptoms (DRESS): Shows eosinophilic infiltrate 2. **Timing:** Biopsy should be taken from an active lesion (target or atypical target), preferably from the edge of a blister. 3. **Specimen handling:** Tissue for both routine H&E staining and direct immunofluorescence should be obtained. **High-Yield:** The histopathological finding of **widespread epidermal necrosis with minimal dermal inflammation** is pathognomonic for SJS/TEN and separates it from erythema multiforme, which shows dermal-predominant inflammation. **Clinical Pearl:** Biopsy confirmation is particularly important in early SJS when clinical diagnosis may be uncertain, and it helps guide prognosis and management intensity. ### Why Other Investigations Are Not First-Line - **Viral serology:** While HSV-1 and other viruses may trigger SJS, serology is not diagnostic of the syndrome itself - **Immunofluorescence:** Direct IF is typically negative in SJS (unlike EM, which may show IgM/C3 at the dermal-epidermal junction) - **Bacterial culture:** Not indicated; SJS is not an infectious disease but a drug/pathogen-triggered immune reaction 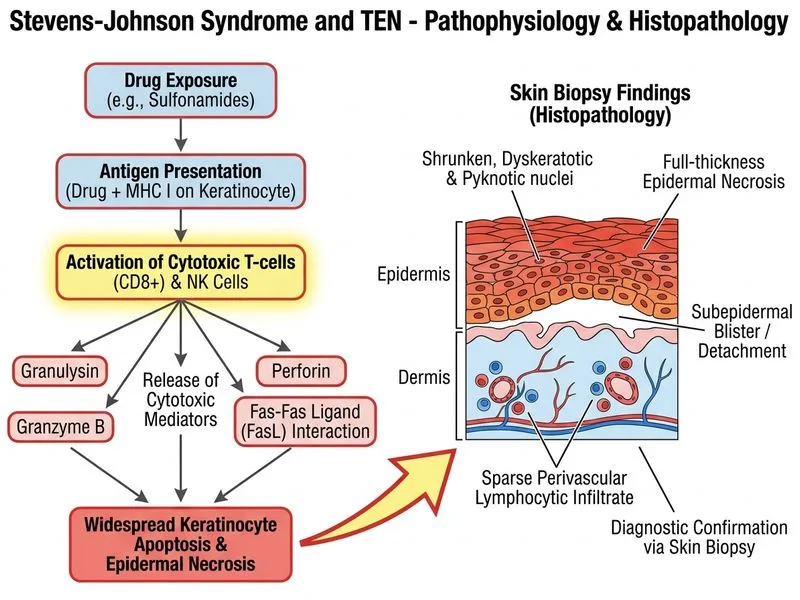
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.