## Immediate Management of Stevens-Johnson Syndrome **Key Point:** The cornerstone of SJS management is immediate discontinuation of the offending drug and transfer to a specialized unit (burns ICU or dermatology ICU) for supportive care, even when involvement is <10% BSA. ### Why Immediate Drug Withdrawal is Critical 1. **Pathophysiology**: SJS is a drug-induced, T-cell-mediated cytotoxic reaction. The offending drug (here, TMP-SMX) must be stopped immediately to halt progression. 2. **Progression Risk**: Without drug withdrawal, SJS can rapidly progress to TEN (>30% BSA) within 24–72 hours, with mortality increasing from 5% to 30%. 3. **Specialized Unit Transfer**: These patients require: - Fluid and electrolyte management (similar to severe burns) - Nutritional support (often via feeding tube) - Infection prevention in a controlled environment - Ophthalmologic and mucosal care to prevent long-term sequelae ### Why Other Options Are Incorrect **High-dose corticosteroids (Option A):** - Controversial and not first-line. Early systemic corticosteroids may increase infection risk without clear mortality benefit. - Some experts advocate for short courses in severe cases, but drug withdrawal takes absolute priority. - Not the "most appropriate immediate" step. **Observation with topical care alone (Option C):** - Dangerous delay. SJS requires ICU-level monitoring for fluid shifts, electrolyte imbalance, and early infection. - Topical care is supportive, not curative. - <10% BSA today can become >30% BSA (TEN) within 48 hours without drug withdrawal and intensive support. **Urgent skin grafting (Option D):** - Premature and contraindicated in acute phase. Grafting is considered only after: - Stabilization (typically day 7–10) - Cessation of new blister formation - Infection control - Early grafting increases infection risk and is not the immediate next step. ### Clinical Pearl **High-Yield:** The **RegiSCAR scoring system** (Reaction to Anticonvulsants Score) helps identify high-risk drugs (anticonvulsants, sulfonamides, NSAIDs, allopurinol, antibiotics). TMP-SMX is a well-known culprit. Once SJS is suspected, the drug must go immediately. ### Management Timeline ```mermaid flowchart TD A[SJS suspected: fever + rash + mucosal erosions + biopsy confirmation]:::outcome --> B[STOP offending drug immediately]:::urgent B --> C[Transfer to burns/ICU unit]:::action C --> D[Supportive care: fluids, electrolytes, nutrition]:::action D --> E[Ophthalmology & mucosal care]:::action E --> F{Stabilization by day 7-10?}:::decision F -->|Yes| G[Consider skin grafting if needed]:::action F -->|No| H[Escalate care; rule out infection/sepsis]:::urgent ``` **Mnemonic:** **STOP-SJS** = **S**top drug, **T**ransfer to ICU, **O**phtho review, **P**revent infection. 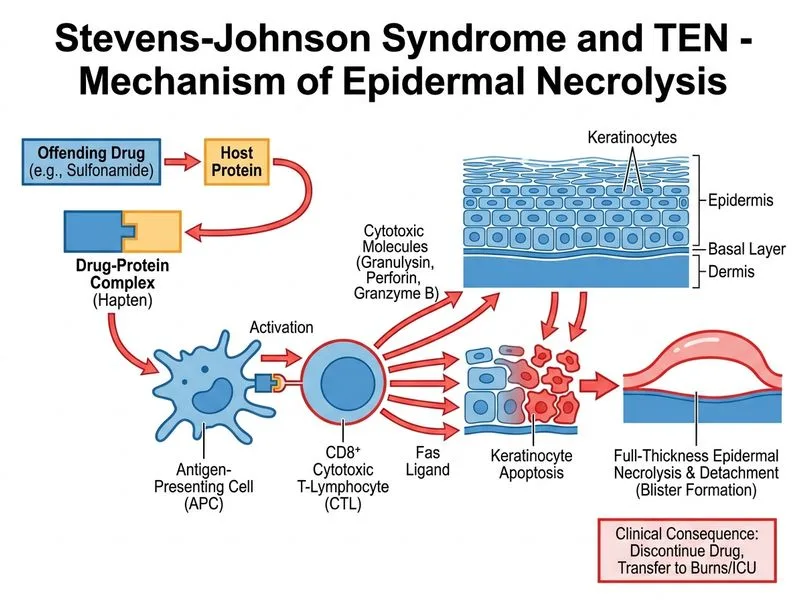
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.