## Diagnosis: Stevens-Johnson Syndrome (SJS) ### Clinical Presentation Analysis **Key Point:** SJS is characterized by the acute onset of fever, mucosal involvement, and a targetoid rash with <10% body surface area (BSA) involvement of blistering and detachment. This patient presents with: - **Mucosal involvement:** Extensive erosions of lips, buccal mucosa, and pharynx (hallmark of SJS/TEN) - **Systemic symptoms:** Fever, severe oral pain, dysphagia - **Skin findings:** Targetoid lesions with central blistering on trunk, face, neck, and proximal limbs - **Drug exposure:** Amoxicillin-clavulanate initiated 5 days prior (common culprit) - **Histopathology:** Full-thickness epidermal necrosis with minimal dermal inflammation (pathognomonic) ### SJS vs TEN Classification | Feature | SJS | TEN | SJS/TEN Overlap | |---------|-----|-----|------------------| | **BSA involvement** | <10% | >30% | 10–30% | | **Mucosal involvement** | Often present | Usually present | Present | | **Epidermal necrosis** | Full-thickness | Full-thickness | Full-thickness | | **Mortality** | 1–5% | 25–50% | 10–15% | | **Histology** | Minimal dermal inflammation | Minimal dermal inflammation | Minimal dermal inflammation | **High-Yield:** The extent of BSA involvement is the PRIMARY criterion for distinguishing SJS from TEN. This patient has rash involvement limited to trunk, face, neck, and proximal limbs—estimated <10% BSA—consistent with SJS. ### Pathophysiology **Clinical Pearl:** SJS/TEN is a cytotoxic T-lymphocyte (CTL)-mediated reaction. The drug (or its metabolite) acts as a hapten, binding to HLA molecules and presenting to CTLs. This triggers massive keratinocyte apoptosis, leading to full-thickness epidermal necrosis with relatively spared dermis. **Mnemonic: DRESS vs SJS** — **DRESS = Delayed Reaction with Eosinophilia and Systemic Symptoms** - DRESS: atypical lymphocytes, eosinophilia, lymphadenopathy, hepatosplenomegaly, skin involvement develops slowly (2–8 weeks) - SJS: acute onset (days), minimal dermal inflammation, no eosinophilia ### Management Principles 1. **Immediate:** Discontinue amoxicillin-clavulanate 2. **Supportive care:** IV fluids, electrolyte monitoring, pain control, eye care (risk of corneal ulceration) 3. **Systemic corticosteroids:** Controversial but often used in early SJS (within 48 hours of onset) 4. **ICU monitoring:** For fluid/electrolyte balance and infection surveillance 5. **Ophthalmology consultation:** Mandatory (risk of symblepharon, corneal scarring) **Warning:** Do NOT use NSAIDs or antibiotics (except for documented infection) in SJS/TEN—they may worsen disease. [cite:Robbins 10e Ch 25] 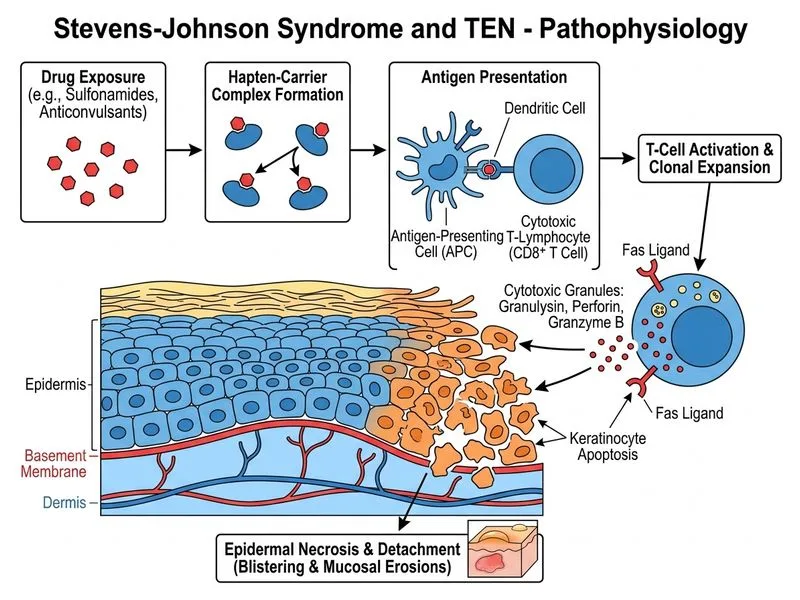
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.