## Diagnosis: Toxic Epidermal Necrolysis (TEN) ### Clinical Recognition **Key Point:** This patient meets diagnostic criteria for TEN: - >30% BSA involvement with full-thickness epidermal necrosis - Positive Nikolsky sign (indicates keratinocyte apoptosis) - Mucosal involvement (oral, conjunctival, genital) - Temporal relationship to drug initiation (TMP-SMX is a high-risk culprit) - Systemic symptoms (fever, malaise) ### Management Algorithm ```mermaid flowchart TD A[Suspected SJS/TEN]:::outcome --> B{Confirm diagnosis<br/>and assess BSA}:::decision B -->|SJS: 1-10% BSA| C[Discontinue offending drug<br/>Supportive care<br/>Consider IVIG/systemic corticosteroids]:::action B -->|SJS-TEN overlap: 10-30% BSA| D[Discontinue offending drug<br/>ICU admission<br/>Multidisciplinary care]:::action B -->|TEN: >30% BSA| E[IMMEDIATE discontinuation<br/>of offending drug]:::urgent E --> F[ICU admission]:::action F --> G[Fluid/electrolyte management<br/>Nutritional support<br/>Pain control<br/>Infection prevention]:::action G --> H[Consider IVIG or<br/>systemic corticosteroids<br/>per institution protocol]:::action ``` ### Immediate Priorities (First 24 Hours) 1. **Discontinue the offending drug immediately** — TMP-SMX is a well-established culprit 2. **ICU/high-dependency unit admission** — TEN is a dermatological emergency with mortality 20–50% 3. **Fluid resuscitation** — like severe burns; use Parkland formula or modified approach 4. **Infection prevention** — sterile technique, avoid unnecessary antibiotics (risk of cross-sensitization) 5. **Ophthalmology consultation** — conjunctival involvement requires urgent assessment to prevent blindness 6. **Nutritional support** — enteral feeding preferred; parenteral if GI involvement severe ### Why NOT Corticosteroids Alone? **High-Yield:** The role of systemic corticosteroids in TEN remains controversial. Early high-dose corticosteroids (e.g., methylprednisolone 1–2 g/day IV) may reduce progression if given within 48 hours of onset, but evidence is mixed. **IVIG (2 g/kg over 3–5 days) is increasingly preferred** as first-line adjunctive therapy due to lower infection risk. However, **discontinuation of the offending drug is non-negotiable and must happen first**. ### Why NOT Continue the Drug? **Warning:** Continuing TMP-SMX while adding corticosteroids is a critical error. The drug is the source of the problem; corticosteroids alone cannot stop the cascade of keratinocyte apoptosis triggered by the offending agent. Continuing the drug will only worsen outcome. ### Scoring: SCORTEN Scale (Prognostic) Use to predict mortality: - Age >40 years: 1 point - Heart rate >120/min: 1 point - Serum urea >10 mmol/L: 1 point - Serum glucose >14 mmol/L: 1 point - Active malignancy: 1 point - BSA detached on day 1 >10%: 1 point **Score ≥4** = mortality ~90%; **Score 0–1** = mortality ~3%. ### Key Drugs Associated with SJS/TEN **Mnemonic: SCAR** — Sulfonamides, Carbamazepine, Allopurinol, Retinoids - **Sulfonamides** (TMP-SMX, sulfasalazine) — highest risk - **Anticonvulsants** (phenytoin, carbamazepine, phenobarbital) - **NSAIDs** (especially long-acting: meloxicam, piroxicam) - **Antibiotics** (fluoroquinolones, macrolides, beta-lactams) - **Allopurinol** — dose-dependent risk **Clinical Pearl:** TEN is a medical emergency equivalent to severe thermal burns. Mortality correlates with BSA involvement and delay in drug discontinuation. Every hour counts. 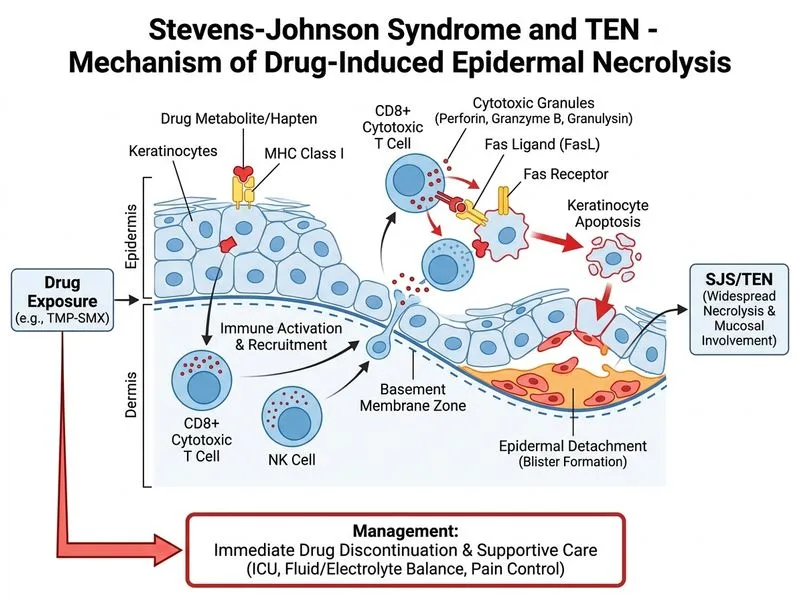
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.