## Clinical Diagnosis: Stevens-Johnson Syndrome (SJS) **Key Point:** This patient meets diagnostic criteria for SJS based on: - Prodromal fever and systemic symptoms - Characteristic target lesions with central blistering - Mucosal involvement (oral ulceration, conjunctival injection, lip crusting) - Temporal relationship to trimethoprim-sulfamethoxazole (TMP-SMX is a classic culprit) - Skin biopsy showing full-thickness epidermal necrosis ## Management Algorithm ```mermaid flowchart TD A[SJS/TEN Diagnosis Confirmed]:::outcome --> B[Immediate Actions]:::action B --> B1[Stop offending drug immediately] B --> B2[Transfer to ICU/Burn unit] B --> B3[Fluid & electrolyte resuscitation] B1 --> C{Extent of Involvement?}:::decision C -->|< 10% BSA| D[Supportive care + monitoring]:::action C -->|10-30% BSA| E[Consider IVIG or Cyclosporine]:::action C -->|> 30% BSA| F[IVIG 2g/kg or Cyclosporine]:::action D --> G[Avoid systemic corticosteroids]:::urgent E --> G F --> G ``` **High-Yield:** The cornerstone of SJS/TEN management is **immediate discontinuation of the offending drug**. Unlike many dermatologic emergencies, systemic corticosteroids are NOT first-line and may increase infection risk and mortality in severe cases [cite:Harrison 21e Ch 56]. **Clinical Pearl:** The patient's skin biopsy showing full-thickness epidermal necrosis with minimal dermal inflammation is pathognomonic for SJS/TEN and distinguishes it from other severe drug reactions (e.g., DRESS, which shows prominent dermal inflammation). **Warning:** Do NOT delay drug withdrawal while awaiting further investigations. Every hour counts in preventing disease progression. ## Supportive Care Essentials | Intervention | Rationale | |---|---| | IV fluid resuscitation (Parkland formula) | Prevent hypovolemic shock; estimate 1–1.5 L/% BSA affected | | Electrolyte monitoring & correction | Massive fluid loss mimics burn injury | | Nutritional support (NG feeding) | Oral ulceration prevents oral intake | | Ophthalmology consultation | Prevent corneal scarring and blindness | | Avoid NSAIDs, antibiotics (except proven safe) | Risk of triggering or worsening reaction | **Mnemonic:** **STOP SJS** = **S**top drug, **T**ransfer to ICU, **O**phthalmic care, **P**erfusion support, **S**upportive measures, **J**oin multidisciplinary team, **S**econd opinion on corticosteroids. ## Role of Immunosuppression - **Systemic corticosteroids:** Controversial; meta-analyses show no mortality benefit and possible increased infection risk. Avoid unless severe mucosal involvement threatens airway. - **IVIG:** May be considered in severe cases (>30% BSA) or rapidly progressive disease, but evidence is mixed. - **Cyclosporine:** Emerging evidence suggests benefit in severe TEN; not standard in SJS. **Key Point:** The absence of systemic corticosteroids in the immediate management is the critical differentiator in this question. 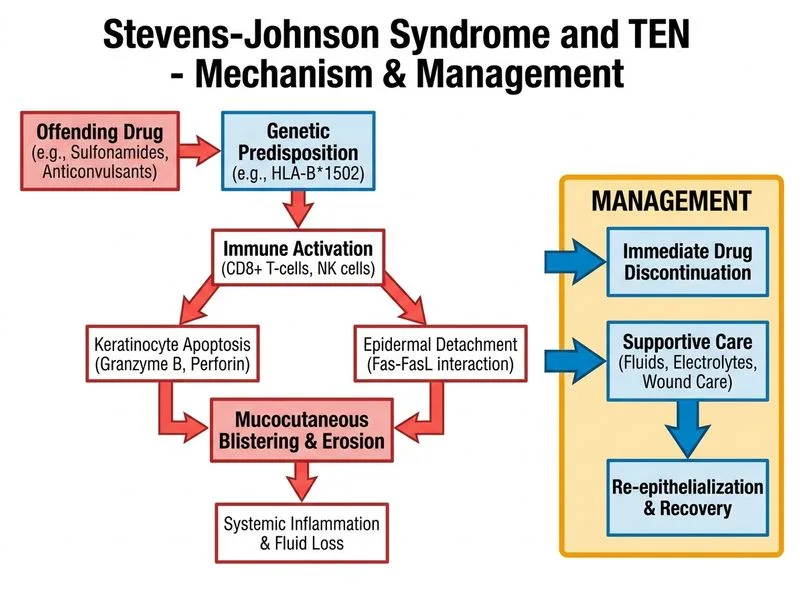
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.