## Diagnosis and Immediate Management **Key Point:** Stevens-Johnson Syndrome (SJS) is a severe cutaneous adverse drug reaction characterized by involvement of <10% body surface area (BSA), with mucosal involvement in >90% of cases. The clinical triad of fever, mucosal ulceration, and targetoid lesions with epidermal necrosis on histology confirms SJS. ### Immediate Management Priorities 1. **Drug Withdrawal** — The offending agent (cotrimoxazole in this case) must be stopped immediately. Continuation delays healing and increases mortality risk. 2. **Supportive Care** — This is the cornerstone of management: - Fluid and electrolyte replacement (large fluid losses from denuded skin) - Nutritional support (oral intake often impaired due to mucosal involvement) - Pain control - Infection prevention (barrier nursing, sterile dressings) 3. **Monitoring** — Assess for systemic complications (hepatic, renal, pulmonary involvement) ### Role of Systemic Corticosteroids **High-Yield:** The use of systemic corticosteroids in SJS/TEN remains controversial. Current evidence suggests: - Early high-dose corticosteroids (within 48 hours of onset) may reduce progression and mortality in severe cases - However, they do NOT accelerate healing and carry infection risk in an already immunocompromised state - Most guidelines recommend AGAINST routine corticosteroid use in established SJS unless there is evidence of systemic organ involvement - Supportive care alone is often sufficient for SJS (BSA <10%) ### Histopathology Correlation Full-thickness epidermal necrosis with subepidermal blister formation is pathognomonic for SJS/TEN and confirms the diagnosis. This distinguishes it from: - Erythema multiforme (superficial dermal inflammation, keratinocyte necrosis limited to basal layer) - Drug reaction with eosinophilia and systemic symptoms (DRESS) — perivascular infiltrate, no epidermal necrosis **Clinical Pearl:** The presence of mucosal involvement (oral, ocular, genital) in >90% of SJS cases makes this a systemic disease requiring intensive supportive care and monitoring for ocular sequelae (symblepharon, corneal scarring). ### Why Supportive Care is the Cornerstone SJS is fundamentally a disorder of keratinocyte apoptosis triggered by drug-immune interaction. Management focuses on: - Halting the trigger (drug withdrawal) - Supporting the patient through the acute phase (fluid, nutrition, infection prevention) - Preventing complications (ophthalmologic involvement, secondary infection, organ dysfunction) [cite:Harrison 21e Ch 56] 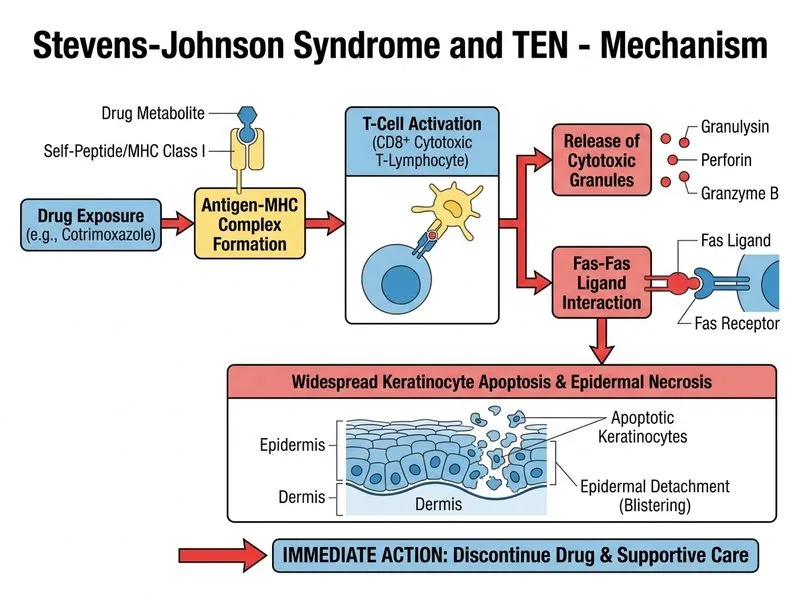
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.