## Diagnosis: Toxic Epidermal Necrolysis (TEN) **Key Point:** This patient has Toxic Epidermal Necrolysis (TEN), not SJS. The defining feature is epidermal necrosis involving >30% of body surface area (this patient has 35% BSA involvement). Near-total epidermal necrosis with minimal inflammation on histology is pathognomonic for TEN. ### Distinguishing SJS from TEN | Feature | SJS | TEN | |---------|-----|-----| | **BSA involvement** | <10% | >30% | | **Mucosal involvement** | >90% | >90% | | **Histology** | Full-thickness epidermal necrosis, subepidermal blister | Near-total epidermal necrosis, minimal inflammation | | **Mortality** | 5–10% | 25–50% | | **Management urgency** | High | **CRITICAL** | **High-Yield:** TEN is a dermatologic emergency with mortality rates of 25–50% depending on age and organ involvement. This patient requires ICU-level care. ### Immediate Management of TEN 1. **Drug Withdrawal** — All potentially offending drugs must be stopped immediately. Isoniazid, rifampicin, and pyrazinamide are all known culprits in anti-TB regimens. 2. **Specialist Transfer** — Transfer to a burn unit or specialized dermatology ICU is mandatory. TEN patients require: - Intensive fluid and electrolyte management (losses equivalent to 30–50% BSA burn) - Nutritional support (often via nasogastric or parenteral nutrition) - Infection prevention (sterile technique, barrier nursing) - Temperature regulation - Ophthalmologic monitoring (prevent symblepharon, corneal scarring) 3. **Systemic Corticosteroids** — In TEN (unlike SJS), early high-dose systemic corticosteroids are indicated: - Start within 48 hours of onset (this patient is at day 7, but still within treatment window) - Typical regimen: methylprednisolone 1–2 g/day IV or equivalent - Evidence suggests corticosteroids reduce mortality and progression in TEN - Taper gradually as lesions stabilize 4. **Supportive Care** - IV fluid resuscitation (calculate using Parkland formula or similar) - Electrolyte monitoring and replacement - Pain control (opioids often required) - Prophylactic antibiotics (not therapeutic; infection is a major cause of death) - Nutritional support **Clinical Pearl:** TEN is a medical emergency with mortality comparable to severe thermal burns. The patient should be managed in an ICU with multidisciplinary input (dermatology, intensive care, ophthalmology, infectious disease). ### Why This Patient Requires Corticosteroids Unlike SJS, where corticosteroids are controversial, TEN with >30% BSA involvement has stronger evidence for benefit from early high-dose corticosteroids. The rationale: - Corticosteroids suppress the cytotoxic T-cell response driving keratinocyte apoptosis - Early administration (within 48–72 hours) may halt progression - In TEN, the risk-benefit favors treatment, as mortality without intervention is very high **Mnemonic: TEN-ALERT** — **T**emperature control, **E**lectrolytes, **N**utrition, **A**ntibiotics (prophylactic), **L**ung monitoring, **E**yes (ophthalmology), **R**enal function, **T**ransfer to ICU/burn unit. [cite:Harrison 21e Ch 56; Robbins 10e Ch 25] 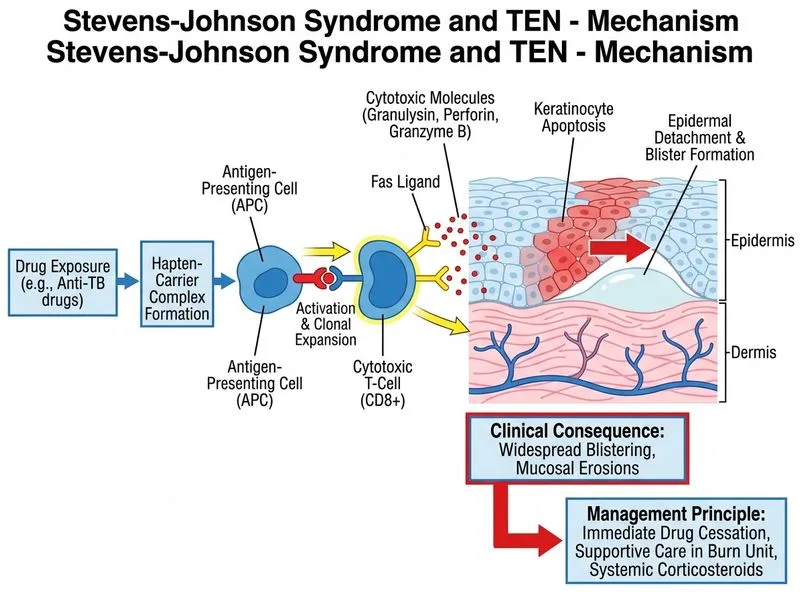
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.