## Management of Stevens-Johnson Syndrome (SJS) ### Immediate Actions in Acute SJS **Key Point:** The single most critical intervention in SJS is immediate discontinuation of the causative drug. This is the only intervention proven to halt disease progression and reduce mortality. **High-Yield:** In this case, trimethoprim-sulfamethoxazole is the likely culprit (one of the top 3 causative drugs in SJS). Stopping it is non-negotiable and must occur within hours of diagnosis. ### Rationale for Correct Answer 1. **Drug withdrawal** — stops the pathogenic cascade; delays of even 24–48 hours worsen outcomes and increase mortality risk. 2. **Systemic corticosteroids** — methylprednisolone 1–2 mg/kg/day IV or high-dose oral prednisolone (0.5–1 mg/kg/day) is initiated concurrently to suppress the immune-mediated epidermal necrosis and mucosal inflammation. 3. **Timing** — both steps must occur simultaneously and urgently; this patient has 25% BSA involvement and mucosal involvement, consistent with SJS (not EM minor). ### Supportive Management (Concurrent) | Intervention | Rationale | |---|---| | Fluid and electrolyte replacement | Large surface area loss; risk of hypovolemia | | Topical care (non-adherent dressings, gentle cleansing) | Minimize secondary infection and pain | | Ophthalmology consultation | Prevent corneal scarring and blindness | | Nutritional support | High metabolic demand from extensive skin loss | | Monitoring for infection | Impaired skin barrier; highest cause of death | **Clinical Pearl:** SJS is a medical emergency with mortality 1–5% if managed early; delayed recognition and continued drug exposure increase mortality to 10–15%. ### Why Biopsy Is NOT the First Step **Warning:** While histopathology (full-thickness epidermal necrosis with subepidermal blister) is diagnostic, waiting for biopsy results delays life-saving drug withdrawal and corticosteroid initiation. Clinical diagnosis in this context is sufficient; biopsy can be deferred or performed after stabilization if diagnosis is uncertain. ### Plasmapheresis and Antibiotics **Tip:** Plasmapheresis is not first-line and is reserved for severe TEN (>30% BSA) unresponsive to corticosteroids or when corticosteroids are contraindicated. Empirical antibiotics are given only if infection is suspected; prophylactic antibiotics are not routine and may increase resistance risk. [cite:Robbins 10e Ch 25] 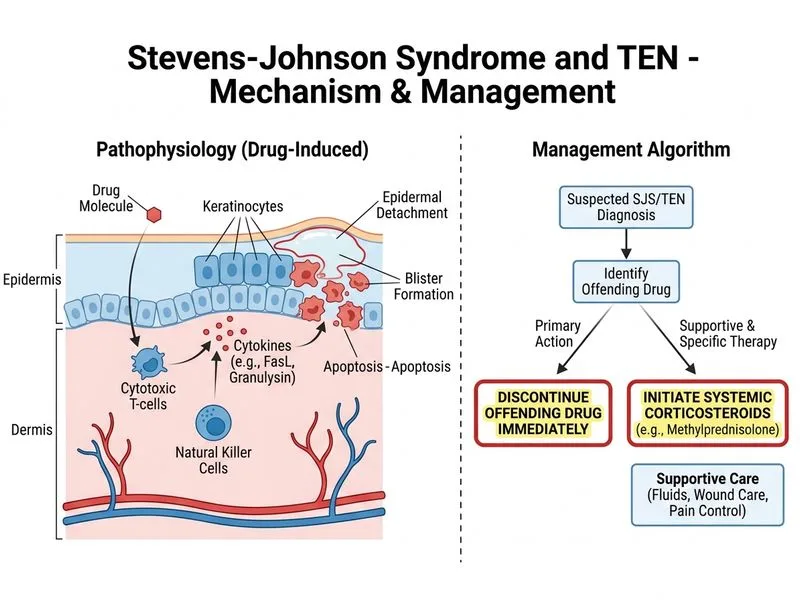
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.