## Imaging in Subarachnoid Hemorrhage (SAH) ### Clinical Context This patient has clinical and CSF evidence of SAH (xanthochromia on LP) but a normal CT head. While CT is highly sensitive for acute SAH (>95% within 6 hours), sensitivity decreases over time as blood is metabolized. The question asks for the **most sensitive modality to detect the source** (aneurysm, AVM, or other vascular lesion). ### Comparison of Modalities | Modality | Sensitivity for Aneurysm | Timing | Invasiveness | Role in SAH | |----------|--------------------------|--------|--------------|-------------| | **CT angiography (CTA)** | 95–98% | Acute phase | Non-invasive | First-line when CT+ | | **MRA** | 85–90% | Any time | Non-invasive | Alternative when CTA contraindicated | | **Digital subtraction angiography (DSA)** | 98–100% | Any time | Invasive (catheter) | Gold standard; therapeutic capability | | **Transcranial Doppler** | 60–70% | Any time | Non-invasive | Detects vasospasm, not source | | **Repeat CT** | Same as initial | Delayed | Non-invasive | Not for source detection | ### Why DSA is the Answer **Key Point:** Digital subtraction angiography (DSA) is the **gold standard** and **most sensitive** imaging modality for detecting the source of SAH, with sensitivity approaching 100% for aneurysms ≥3 mm. - **Superior resolution**: Real-time vascular imaging with spatial resolution superior to CTA and MRA. - **Therapeutic capability**: If an aneurysm is identified, coil embolization can be performed in the same session. - **Detects small lesions**: Can identify aneurysms <3 mm that might be missed on CTA/MRA. - **Definitive diagnosis**: When CTA/MRA are inconclusive (as stated in the stem), DSA is the next step. ### Clinical Approach ```mermaid flowchart TD A[Suspected SAH: headache + neck stiffness]:::outcome --> B[Non-contrast CT head]:::action B --> C{CT positive for blood?}:::decision C -->|Yes| D[CTA brain]:::action C -->|No| E[Lumbar puncture]:::action E --> F{Xanthochromia present?}:::decision F -->|Yes| G[Confirmed SAH]:::outcome G --> H{CTA conclusive?}:::decision H -->|Yes| I[Coil embolization if aneurysm]:::action H -->|No| J[DSA - gold standard]:::action J --> K[Identify source + treat]:::action ``` **High-Yield:** In patients with SAH and **inconclusive CTA**, DSA is mandatory before discharge. It is both diagnostic and therapeutic. **Clinical Pearl:** DSA carries a small risk of stroke (~0.5–1%), but this is justified when the source must be identified and treated. MRA is a reasonable non-invasive alternative if DSA is contraindicated (e.g., renal failure, contrast allergy), but it is less sensitive. ### Why Each Distractor is Wrong **Option 0 (MRA):** While MRA is non-invasive and can detect most aneurysms (85–90% sensitivity), it is **less sensitive than DSA** and lacks therapeutic capability. It is a reasonable alternative when DSA is contraindicated, but DSA is more sensitive. **Option 2 (Transcranial Doppler):** TCD detects **vasospasm** (increased flow velocity in narrowed vessels), not the source of bleeding. It is used for surveillance after SAH, not for aneurysm detection. **Option 3 (Repeat CT after 24 hours):** Repeating non-contrast CT does not improve sensitivity for detecting the **source** of bleeding; it merely confirms the presence of blood. It does not identify the aneurysm or vascular lesion responsible. ## Summary **Key Point:** DSA is the **gold standard** for detecting the source of SAH when CTA is inconclusive, with 98–100% sensitivity and the added advantage of allowing immediate therapeutic intervention (coil embolization). 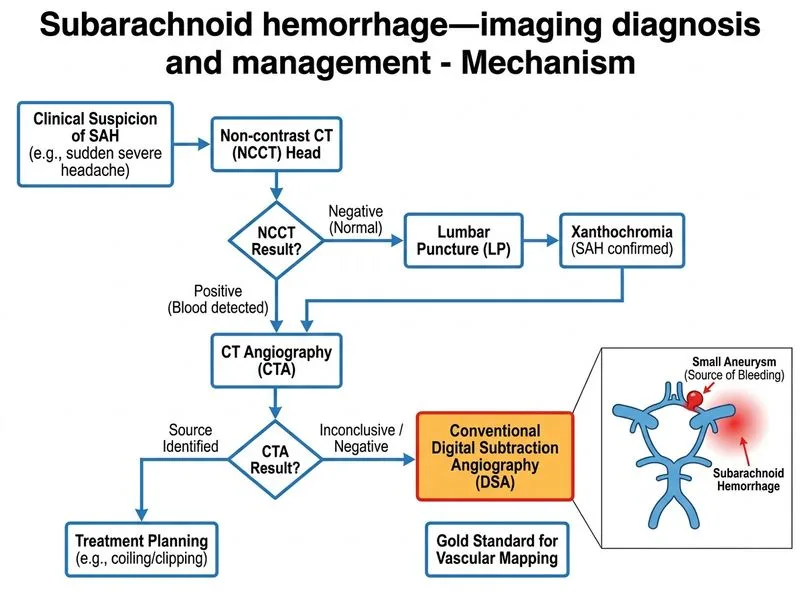
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.