## Investigation of Choice for Supracondylar Fracture ### Clinical Context Supracondylar fractures of the humerus are the most common elbow fractures in children, typically occurring after a FOOSH injury. The clinical presentation of severe swelling, loss of extension, and absent radial pulse suggests a displaced fracture with potential vascular compromise. ### Why Plain Radiography is the Investigation of Choice **Key Point:** Plain radiographs (AP and lateral views) are the gold standard for diagnosis and classification of supracondylar fractures. They are: - Immediately available in the emergency setting - Sufficient to confirm fracture presence and displacement - Essential for Gartland classification (Types I, II, III) - Non-invasive and rapid - Allow assessment of fracture pattern and comminution ### Role of Vascular Assessment **Clinical Pearl:** While the absent radial pulse is concerning for vascular injury, the initial management priority is: 1. Confirm fracture diagnosis with plain radiographs 2. Assess fracture displacement and type 3. Reduce the fracture urgently (often restores perfusion) 4. Re-assess pulse after reduction If pulse remains absent post-reduction, then advanced imaging (Doppler ultrasound or CT angiography) is warranted. ### Why Other Investigations Are Not First-Line | Investigation | Limitation | |---|---| | **Doppler ultrasound** | Useful for vascular assessment but does NOT diagnose the fracture; requires plain films first | | **CT angiography** | Delays urgent fracture reduction; reserved for post-reduction vascular complications | | **MRI** | Time-consuming, not suitable for acute trauma; poor for bone detail in acute setting | **High-Yield:** The vascular status (pulse presence/absence) is a clinical finding, not an investigation finding. Plain radiographs guide fracture reduction, which is the definitive treatment for most vascular compromise in supracondylar fractures. 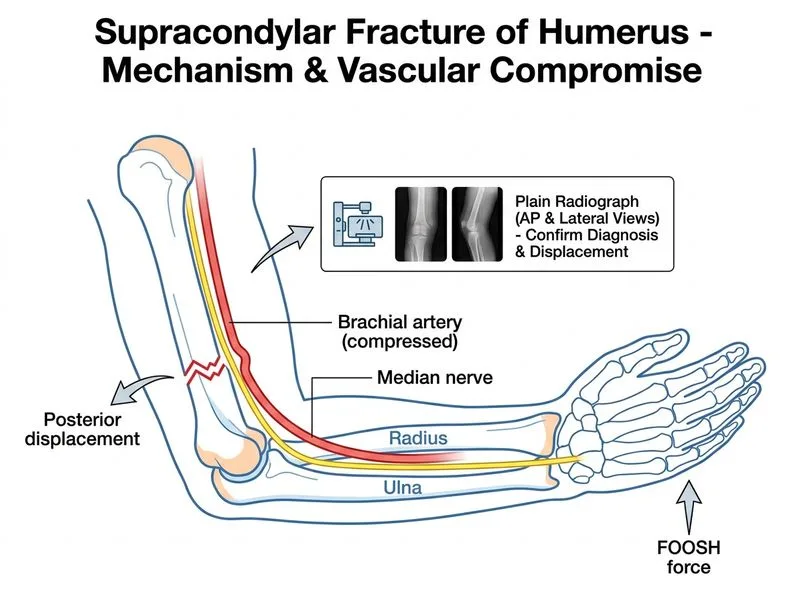
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.