## Distinguishing Supracondylar Fracture Types ### Gartland Classification Overview | Feature | Type I | Type II | Type III | |---------|--------|---------|----------| | **Displacement** | No displacement | Anterior angulation, posterior cortex intact | Complete displacement, no cortical contact | | **Neurovascular Risk** | Minimal | Low to moderate | High (40–50% have vascular injury) | | **Anterior Swelling** | Mild | Moderate | Severe, tense | | **Pulse Status** | Normal | Usually present (may be weak) | Often absent or diminished | | **Reduction Difficulty** | Closed reduction easy | Closed reduction usually successful | Often requires open reduction | **Key Point:** Type III fractures have complete loss of cortical contact between proximal and distal fragments, resulting in severe displacement and a much higher incidence of neurovascular injury (particularly brachial artery compression). This is the critical discriminator. ### Clinical Correlation **High-Yield:** The **degree of displacement and associated neurovascular compromise** is the single best distinguishing feature: - Type II: Posterior cortex intact, anterior angulation only → neurovascular injury ~5–10% - Type III: Complete displacement → neurovascular injury ~40–50% **Clinical Pearl:** A tense, severely swollen anterior elbow with absent radial pulse in a child with supracondylar fracture is a Type III until proven otherwise. This mandates urgent reduction (often open) and vascular assessment. **Warning:** Do not confuse the *mechanism* of injury (which is similar across types — falls from height) with the *fracture pattern* (which defines the type). 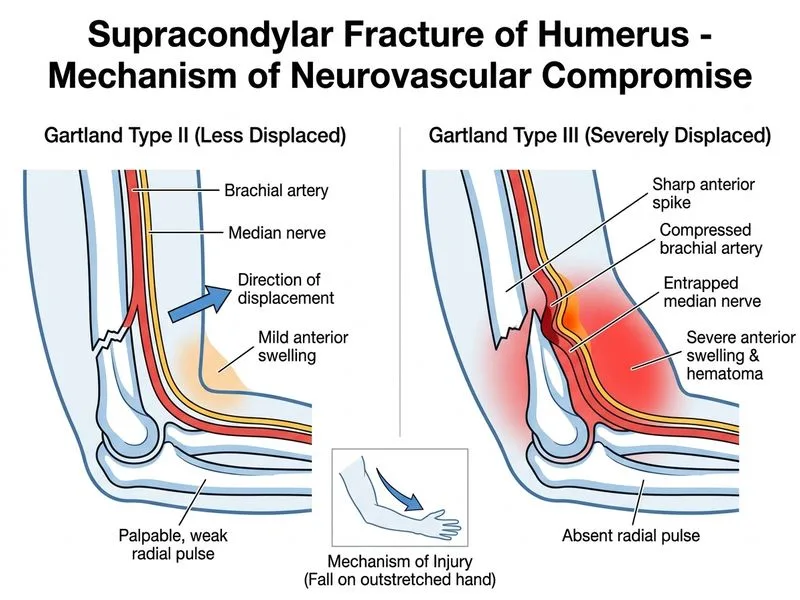
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.