## Investigation for Suspected Nerve Injury Post-Supracondylar Fracture ### Clinical Context: AIN Injury in Supracondylar Fractures **Key Point:** Nerve injuries occur in 10–20% of supracondylar fractures. The anterior interosseous nerve (AIN, a branch of the median nerve) is the most commonly injured nerve, presenting with loss of thumb IP flexion (flexor pollicis longus) and index finger DIP flexion (flexor digitorum profundus to index). **High-Yield:** AIN injury may be: - **Iatrogenic** (from pin placement during reduction) - **Traction-related** (from initial displacement) - **Stretch-related** (from angulation) Most nerve injuries in supracondylar fractures are neurapraxias and recover spontaneously within 3–6 months. ### Why EMG/NCS Is the Gold Standard **Clinical Pearl:** Electromyography (EMG) and nerve conduction studies (NCS) are the definitive investigations for: 1. **Confirming nerve injury** — demonstrates denervation potentials (fibrillations, positive sharp waves) in affected muscles 2. **Assessing severity** — distinguishes neurapraxia (normal NCS, abnormal EMG) from axonotmesis/neurotmesis (abnormal NCS) 3. **Timing of injury** — EMG changes appear 3–5 days after injury; early testing may be falsely negative 4. **Prognostic information** — extent of denervation predicts recovery potential ### Diagnostic Approach Table | Investigation | Role | Timing | Sensitivity | |---|---|---|---| | **Clinical exam** | Initial screening | Immediate | Detects gross deficits; may miss partial injuries | | **EMG/NCS** | Definitive confirmation | 3–5 days post-injury | High; quantifies severity | | **MRI** | Assesses nerve compression/transection | Delayed (if no recovery) | Useful only if surgical exploration planned | | **Plain radiographs** | Assesses fracture/pin position | Immediate | Does not assess nerve status | **Tip:** Do not perform EMG/NCS immediately after injury—wait 3–5 days for denervation changes to appear. Early testing may be falsely reassuring. ### Why Other Investigations Are Inadequate - **Plain radiographs:** Assess fracture reduction and pin position but provide no information about nerve integrity - **MRI of brachial plexus:** Useful for detecting nerve transection or compression in chronic cases; not standard for acute postoperative assessment - **Clinical examination alone:** Establishes the deficit but does not quantify severity or predict recovery; EMG/NCS provides objective, prognostic data **Warning:** Do not delay EMG/NCS if nerve injury is suspected—early testing (after 3–5 days) guides prognosis and treatment decisions. 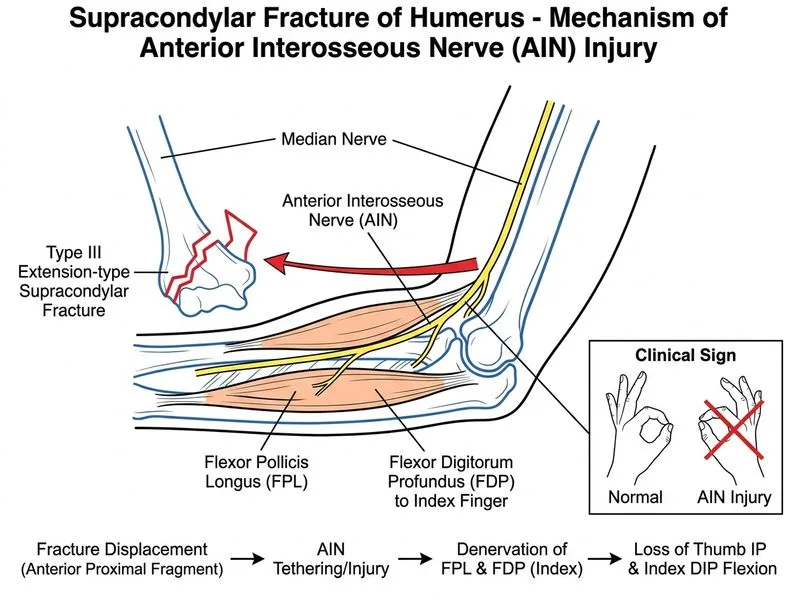
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.