## Management of Displaced Supracondylar Fracture (Gartland Type III) ### Clinical Context This is a **displaced supracondylar fracture with intact neurovascular status**—the gold standard is **urgent closed reduction and percutaneous pinning (CRPP)** within 6–8 hours of injury. ### Why Closed Reduction and Percutaneous Pinning? **Key Point:** Type III supracondylar fractures (displaced, angulated, or rotated) require anatomic reduction to restore alignment and prevent malunion complications (cubitus varus, loss of extension, cosmetic deformity). **High-Yield:** Percutaneous pinning (usually two lateral pins or one medial + one lateral) provides stable fixation after reduction, allows early mobilization, and avoids the morbidity of open surgery in pediatric fractures. **Clinical Pearl:** The window for reduction is **6–8 hours post-injury**. Delays increase risk of vascular compromise, compartment syndrome, and Volkmann's contracture. This patient is well within the safe window at 2 hours. ### Timing and Technique | Aspect | Details | |--------|----------| | **Timing** | Within 6–8 hours of injury (preferably <6 hrs) | | **Anesthesia** | General anesthesia (GA) with muscle relaxation | | **Reduction** | Closed reduction under fluoroscopy | | **Fixation** | Percutaneous K-wires (lateral approach preferred to avoid ulnar nerve) | | **Pins** | Usually 2–3 wires; lateral entry safer than medial | | **Post-op** | Posterior slab, elevation, neurovascular monitoring | ### Why Not the Other Options? **Immobilization alone (Option C):** While appropriate for Type I (non-displaced) fractures, Type III requires reduction to prevent malunion and loss of function. Reassessing after 4–6 hours delays definitive treatment and risks neurovascular deterioration. **Skeletal traction (Option B):** Historically used for Type III fractures, but now largely replaced by CRPP because traction is cumbersome, requires prolonged hospitalization, and carries risk of pin-site complications. Reserved only if CRPP is unavailable or contraindicated. **Open reduction and internal fixation (Option D):** ORIF with plates/screws is reserved for: - Open fractures (Gustilo Grade II–III) - Fractures with vascular injury requiring exploration - Neurovascular compromise not relieved by reduction - Soft tissue interposition preventing closed reduction - Revision cases after failed closed reduction In this uncomplicated displaced fracture with intact neurovascular status, ORIF is unnecessarily invasive. ### Neurovascular Monitoring **Key Point:** Intact neurovascular status does NOT eliminate the need for urgent reduction. Compartment syndrome and vascular compromise can develop within hours. Continuous monitoring is essential post-reduction. **Mnemonic: 5 P's of Compartment Syndrome** — Pain (out of proportion), Pressure (tense compartments), Paresthesia, Pallor, Pulselessness (late sign). 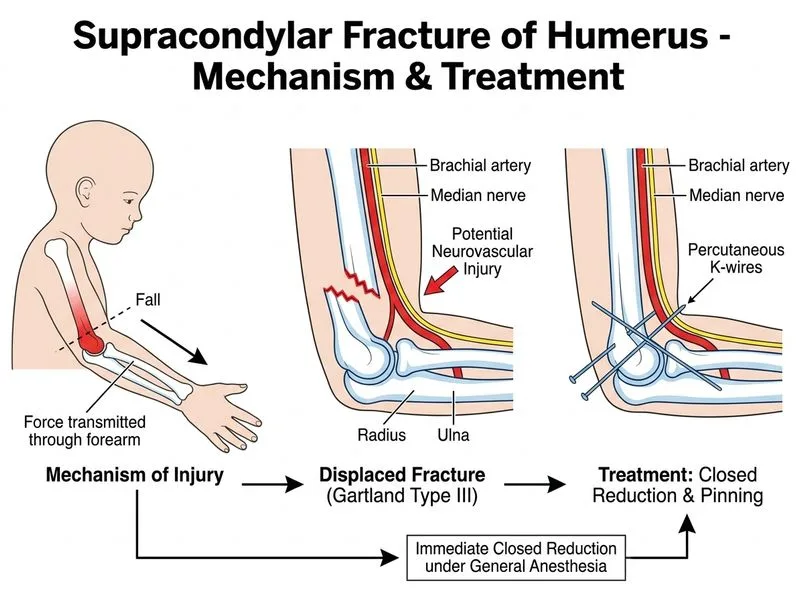
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.