## Gartland Classification of Supracondylar Fractures The Gartland classification system is the gold standard for grading supracondylar fractures based on radiographic displacement and cortical continuity. ### Type II vs Type III: Key Discriminator | Feature | Type II | Type III | |---------|---------|----------| | **Posterior cortex** | Intact (in contact) | Completely displaced (no contact) | | **Distal fragment position** | Angulated posteriorly | Completely displaced posteriorly | | **Radiographic appearance** | Posterior angulation only | Loss of all cortical contact | | **Stability** | Relatively more stable | Highly unstable | | **Reduction difficulty** | Easier (closed reduction often successful) | More difficult (often requires ORIF) | **Key Point:** The defining feature of Type III is **complete loss of cortical contact** between proximal and distal fragments on both AP and lateral views. Type II retains at least some posterior cortical contact, even if angulated. **High-Yield:** Type III fractures have significantly higher rates of: - Neurovascular injury (15–20%) - Loss of reduction after closed reduction - Need for operative fixation (percutaneous pinning or ORIF) **Clinical Pearl:** On lateral X-ray, Type II shows the distal fragment angulated backward but still touching the proximal fragment; Type III shows complete separation with no cortical overlap. **Mnemonic:** **"Contact = Type II; No Contact = Type III"** — if you can see cortical contact on any view, it's Type II; if completely displaced on both views, it's Type III. 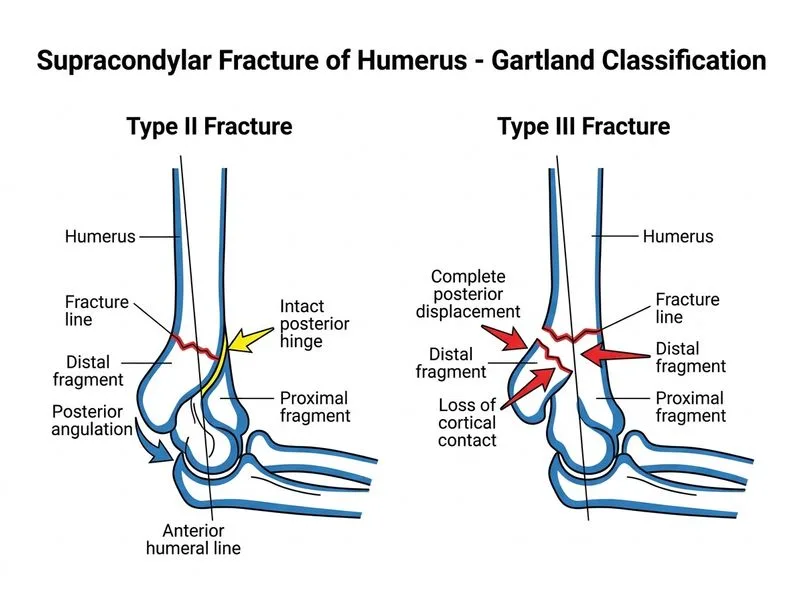
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.