## Management of Displaced Supracondylar Fracture with Neurovascular Compromise ### Clinical Context This is a Gartland Type III (completely displaced) supracondylar fracture with absent radial pulse — a neurovascular emergency. The warm, pink hand indicates collateral circulation is maintaining perfusion, but the absent radial pulse indicates anterior interosseous nerve (AIN) or radial artery involvement. ### Immediate Management Principles **Key Point:** Displaced supracondylar fractures (Gartland Type II–III) require urgent closed reduction under general anesthesia to restore neurovascular integrity and prevent ischemic complications (Volkmann's contracture, compartment syndrome). **High-Yield:** The presence of neurovascular deficit (absent pulse, pale hand, cold fingers) mandates reduction within 6–8 hours. Reduction often restores the pulse spontaneously by relieving traction on the artery. ### Why Closed Reduction + Percutaneous Pinning? 1. **Restores neurovascular status:** Reduction relieves kinking of the brachial artery and reduces nerve compression. 2. **Maintains reduction:** Percutaneous pinning (usually 2–3 lateral or crossed pins) prevents redisplacement after reduction, which is common in Type III fractures. 3. **Avoids open surgery:** Open reduction increases soft-tissue trauma, infection risk, and stiffness — reserved only for: - Failed closed reduction - Open fractures - Vascular injury requiring exploration 4. **Preserves elbow function:** Minimally invasive approach reduces scarring and contracture risk. ### Contraindications to Closed Reduction - Open fracture with vascular injury requiring exploration → open reduction - Irreducible fracture (soft-tissue interposition) → open reduction - Compartment syndrome → fasciotomy + reduction ### Timeline | Scenario | Action | |---|---| | **Neurovascular intact, Type I–II** | Closed reduction + casting (may not need pins if stable) | | **Neurovascular intact, Type III** | Closed reduction + percutaneous pinning | | **Neurovascular deficit, Type III** | **Urgent closed reduction + pinning within 6–8 hrs** | | **Failed closed reduction** | Open reduction + internal fixation | | **Open fracture + vascular injury** | Vascular exploration + reduction + fixation | **Clinical Pearl:** A warm, pink hand with absent radial pulse is a "pink pulseless hand" — this is not an absolute indication for immediate vascular surgery. Reduction alone restores the pulse in ~80% of cases. Vascular exploration is reserved for: - Persistent absent pulse after reduction - Signs of distal ischemia (pale, cold, mottled hand) - Brachial artery transection on imaging ### Why NOT the Other Options? - **Option 2 (Open ORIF):** Increases soft-tissue trauma, infection, and stiffness. Reserved for failed closed reduction or open fractures with vascular injury. - **Option 3 (Cast alone):** Type III fractures are unstable and will redisplace in a cast, leading to malunion, cubitus varus, and loss of elbow extension. Percutaneous pinning is mandatory. - **Option 4 (Skeletal traction):** Outdated. Traction does not reliably maintain reduction and delays definitive fixation, increasing ischemia risk and prolonging hospitalization. [cite:Rockwood & Green's Fractures in Adults 9e Ch 11] 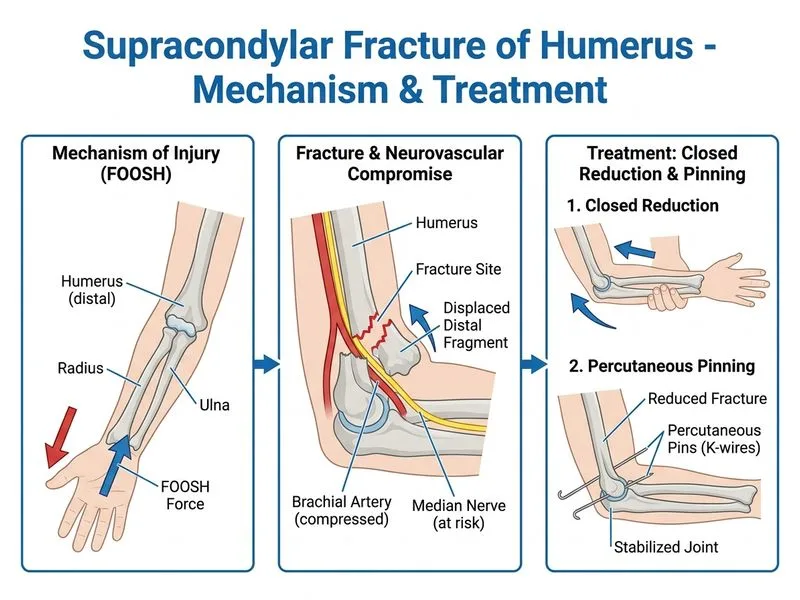
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.