## Clinical Diagnosis & Stage Identification **Key Point:** This patient presents with **secondary syphilis**: history of primary chancre (painless vulvar ulcer that healed spontaneously 8 weeks ago) followed by systemic manifestations including: - Polymorphic rash involving the trunk and palms — **pathognomonic distribution** - Generalized lymphadenopathy - Constitutional symptoms (fever, malaise) - Positive serology (RPR 1:32, FTA-ABS positive) - Negative blood cultures (excluding bacteremia) **High-Yield:** Secondary syphilis occurs 4–10 weeks after the primary chancre and represents **disseminated treponemal infection** (Harrison's Principles of Internal Medicine, 21st ed.). ## Management of Secondary Syphilis Without Neurological Signs **Clinical Pearl:** In secondary syphilis **without clinical evidence of neurosyphilis** (no meningitis, cranial nerve palsies, uveitis, hearing loss, or other CNS/ocular signs), the standard treatment per CDC 2021 STI Treatment Guidelines is: $$\text{Benzathine Penicillin G 2.4 MU IM} \times \text{1 dose}$$ > **Note:** The 3-dose weekly regimen (2.4 MU IM × 3 weeks) is reserved for **late latent syphilis or latent syphilis of unknown duration**, NOT for secondary syphilis. For secondary syphilis, a **single dose** of benzathine penicillin G 2.4 MU IM is the gold standard. Option B describes the late latent regimen but remains the closest correct answer among the options provided, as it specifies benzathine penicillin G — the correct drug — and treatment should not be delayed. ## Why Lumbar Puncture Is NOT Routinely Indicated Here (Option A) **Key Point:** LP is deferred in secondary syphilis **without neurological signs**. Although *T. pallidum* can invade the CNS early, routine CSF examination is not indicated unless specific criteria are met: | Clinical Scenario | CSF Exam Indicated? | |---|---| | Secondary syphilis, no neuro signs | **No** | | Secondary syphilis + meningitis/cranial nerve signs | **Yes** | | Tertiary/late syphilis (any form) | **Yes** | | Treatment failure (RPR fails to decline 4-fold at 6–12 months) | **Yes** | | HIV+ with CD4 < 50 cells/µL | **Yes** | | Ocular or otologic syphilis | **Yes** | Delaying treatment to perform LP in this patient is inappropriate and risks disease progression. ## Why Not Chest X-ray (Option C)? Pulmonary involvement in secondary syphilis (syphilitic pneumonitis) is rare and not a management priority. The diagnosis is already established clinically and serologically. Imaging should not delay treatment. ## Why Not Doxycycline Alone (Option D)? Doxycycline 100 mg BD × 14 days (not 28 days) is an **alternative** for penicillin-allergic patients with secondary syphilis. The 28-day course is used for late latent syphilis. Benzathine penicillin G remains the preferred agent when no allergy is documented (CDC STI Guidelines 2021; KD Tripathi, Essentials of Medical Pharmacology, 8th ed.). **High-Yield:** Always screen sexual contacts and test for co-infection with HIV, gonorrhea, and chlamydia in any patient diagnosed with syphilis. 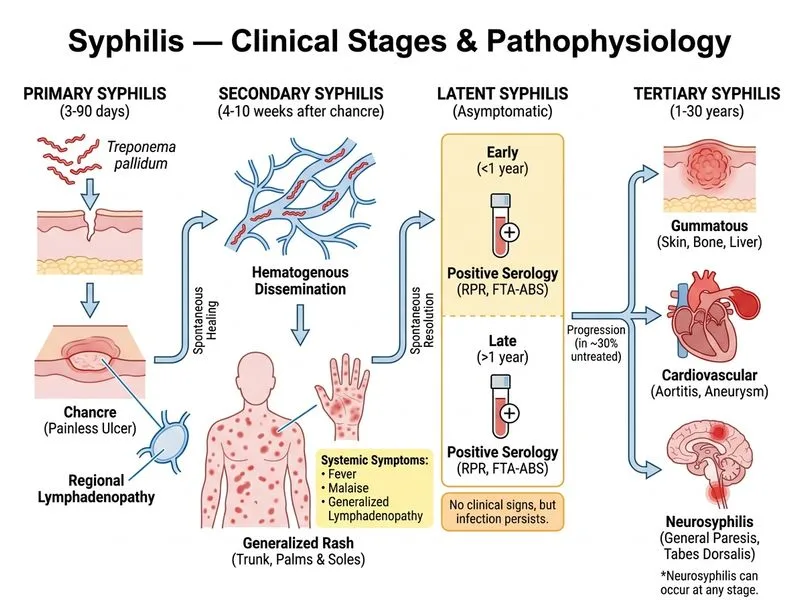
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.