## Clinical Presentation & Biochemical Basis This patient presents with a constellation of findings consistent with **pyruvate dehydrogenase (PDH) complex deficiency** — the most important enzyme defect at the TCA cycle entry point causing lactic acidosis. > **Note on age of presentation:** Classic PDH deficiency (X-linked PDHA1 mutation) typically presents in infancy. However, **late-onset and acquired forms** exist — including partial enzyme deficiencies, thiamine (vitamin B₁) deficiency (which impairs PDH's TPP cofactor), and mitochondrial dysfunction from chronic malnutrition. This patient's rural background, refined-carbohydrate diet, and minimal protein intake strongly suggest **acquired/nutritional PDH dysfunction** (thiamine deficiency), which can manifest in adulthood. --- ### Why PDH Deficiency Best Explains the Findings **Key Point:** Pyruvate dehydrogenase catalyzes the **irreversible, rate-limiting conversion of pyruvate → acetyl-CoA**, the critical gateway into the TCA cycle. Deficiency (or impairment) causes pyruvate accumulation, which is shunted toward lactate via lactate dehydrogenase (LDH). 1. **Elevated lactate & metabolic acidosis** (pH 7.32, HCO₃⁻ 16, lactate 4.2 mmol/L): Accumulated pyruvate → lactate via LDH → lactic acidosis. This is the hallmark of PDH deficiency/impairment. 2. **Hypokalemia**: Secondary to metabolic acidosis-driven renal potassium wasting and impaired muscle energy metabolism. 3. **Muscle weakness & fatigue**: Skeletal muscle depends heavily on oxidative phosphorylation; PDH impairment severely reduces mitochondrial ATP production. 4. **Ketonuria & lipid accumulation**: Impaired acetyl-CoA entry into TCA → compensatory ketogenesis and fatty acid accumulation in muscle (seen on biopsy). 5. **Mitochondrial abnormalities on biopsy**: Chronic PDH dysfunction causes structural mitochondrial changes, consistent with the biopsy findings. --- ### Pathophysiology Summary ``` Glucose → Glycolysis → Pyruvate ↓ [PDH impaired] Pyruvate accumulates ↓ (LDH) Lactate → Lactic Acidosis ↓ (alternative) Ketone bodies → Ketonuria ``` --- ### High-Yield Comparison: Why Not the Other Options? | Enzyme | Substrate → Product | Why NOT the answer here | |--------|---------------------|------------------------| | **Pyruvate dehydrogenase** ✓ | Pyruvate → Acetyl-CoA | **Directly causes pyruvate/lactate accumulation** | | Succinate dehydrogenase (Complex II) | Succinate → Fumarate | Causes fumaric aciduria; does NOT cause lactic acidosis | | Isocitrate dehydrogenase | Isocitrate → α-Ketoglutarate | Citrate accumulation; not associated with lactic acidosis | | α-Ketoglutarate dehydrogenase | α-Ketoglutarate → Succinyl-CoA | Causes organic aciduria (2-oxoglutaric aciduria); pyruvate/lactate NOT elevated | **Clinical Pearl:** PDH is the **only** TCA-related enzyme defect that consistently produces **lactic acidosis** because it is the sole entry point for pyruvate into the TCA cycle. Defects in downstream TCA enzymes (succinate dehydrogenase, α-ketoglutarate dehydrogenase) do not cause pyruvate/lactate accumulation. --- ### Management Implications **High-Yield:** - **Thiamine (Vitamin B₁) supplementation** — PDH requires thiamine pyrophosphate (TPP) as a cofactor; thiamine deficiency is a reversible, acquired cause of PDH dysfunction. - **Ketogenic diet** — bypasses PDH by providing ketones as alternative fuel (used in genetic PDH deficiency). - Avoid high carbohydrate loads (worsen lactate production). - Correct hypokalemia cautiously. [cite: Lehninger Principles of Biochemistry, 7th ed., Ch. 16 & 20; Harper's Illustrated Biochemistry, 31st ed., Ch. 17] 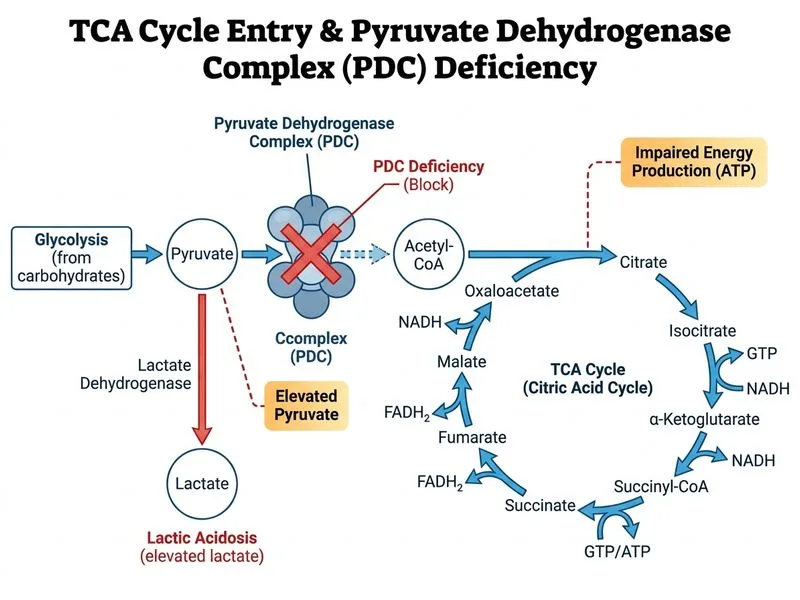
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.