## Clinical Context: Mitochondrial Cytopathy and TCA Cycle Impairment Mutations in mitochondrial DNA-encoded Complex I (NADH dehydrogenase) impair the entry of reducing equivalents into the electron transport chain. This causes: - Reduced NAD^+^ regeneration → impaired TCA cycle flux (TCA dehydrogenases require NAD^+^) - Accumulation of pyruvate and lactate (Pasteur effect reversal) - Ragged-red fibers and mitochondrial proliferation on muscle biopsy - Multi-system involvement (CNS, cardiac, renal, endocrine) ## Pathophysiology of Lactate Accumulation **Key Point:** The elevated lactate-to-pyruvate ratio (20:1) indicates severe impairment of oxidative metabolism. Complex I dysfunction → reduced NAD^+^ → pyruvate cannot be efficiently oxidized in the TCA cycle → shunted to lactate via lactate dehydrogenase. **High-Yield:** Ragged-red fibers are pathognomonic for mitochondrial myopathy; they reflect abnormal mitochondrial proliferation and accumulation of defective mitochondria. ## Management Algorithm for Mitochondrial Cytopathy ```mermaid flowchart TD A[Suspected mitochondrial disease]:::outcome --> B{Genetic confirmation + phenotype assessment?}:::decision B -->|Yes: heteroplasmic mtDNA mutation| C[Specialist metabolic genetics review]:::action C --> D[Assess organ involvement: cardiac, renal, CNS, endocrine]:::action D --> E[Individualized management plan]:::action E --> F[Avoid mitochondrial toxins: valproate, statins, certain antibiotics]:::action E --> G[Supportive: CoQ10, arginine, carnitine as indicated]:::action F --> H[Regular monitoring: lactate, organ function]:::outcome ``` ## Why This Answer is Correct **Key Point:** Mitochondrial cytopathies are multi-system disorders requiring comprehensive assessment and individualized management. The next step is NOT empirical supplementation but rather: 1. **Specialist review:** Metabolic geneticist assesses disease burden, organ involvement (cardiac arrhythmias, cardiomyopathy, renal tubular dysfunction, diabetes, stroke-like episodes), and heteroplasmy load 2. **Avoidance of mitochondrial toxins:** Valproate, statins, certain aminoglycosides, and other drugs worsen mitochondrial function 3. **Tailored supplementation:** CoQ10, L-arginine, L-carnitine, and other agents are considered based on specific defects and organ involvement, not empirically **Clinical Pearl:** Heteroplasmic mutations show variable tissue distribution and clinical severity. Specialist assessment guides prognosis, genetic counseling (maternal inheritance), and prevention of acute decompensation. ## Why Other Options Are Incorrect | Option | Why Wrong | |--------|----------| | High-dose CoQ10 + L-arginine without specialist input | CoQ10 and arginine may be beneficial in some mitochondrial diseases, but empirical use without comprehensive assessment is not standard of care. Dosing, duration, and patient selection require specialist input. Rechecking lactate in 4 weeks delays necessary investigation of organ involvement. | | L-alanine infusion | L-alanine does not directly enhance pyruvate carboxylase or gluconeogenesis in the setting of Complex I dysfunction. This approach ignores the underlying mitochondrial defect and may worsen metabolic acidosis. | | Cardiac catheterization | While mitochondrial cardiomyopathy is common, catheterization is not the first-line investigation. Echocardiography and ECG are non-invasive screening tools. Catheterization is indicated only if structural coronary disease is suspected after imaging. | 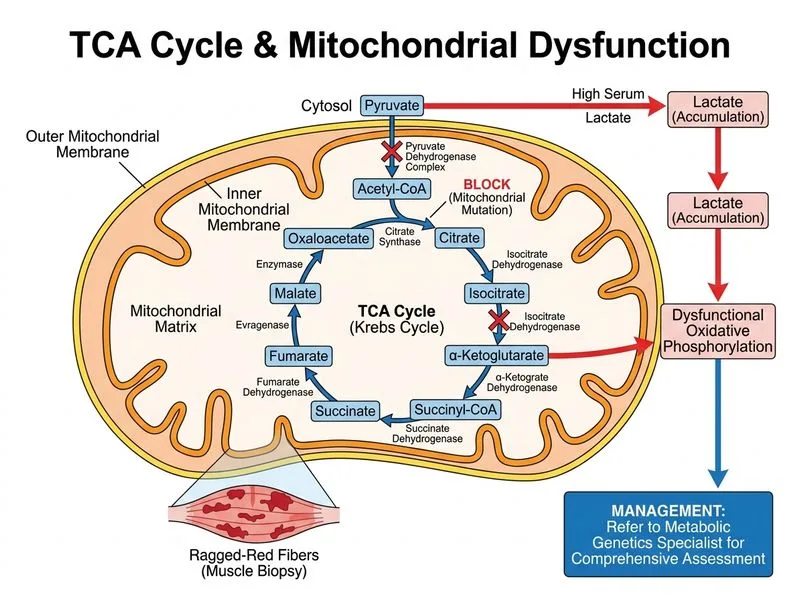
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.