## Diagnosis: Papillary Thyroid Carcinoma (PTC) ### Key Cytological Features **Key Point:** Nuclear grooves and intranuclear pseudoinclusions ("Orphan Annie eye" nuclei) are pathognomonic for papillary thyroid carcinoma on FNAC. The FNAC findings described — nuclear grooves and intranuclear pseudoinclusions — are classic hallmarks of PTC. These nuclear features are so characteristic that their presence on cytology is virtually diagnostic. ### Clinical Presentation | Feature | PTC | FTC | MTC | ATC | |---------|-----|-----|-----|-----| | **Age at presentation** | 30–50 years | 30–50 years | 40–60 years | 50–70 years | | **Nodule character** | Firm, may be fixed | Firm, mobile | Firm, often hard | Hard, fixed, rapidly enlarging | | **Lymph node involvement** | Common (30–50%) | Rare | Common | Common | | **Prognosis** | Excellent (>90% 10-yr survival) | Good (>80% 10-yr survival) | Variable (depends on stage) | Poor (<5% 1-yr survival) | ### Pathological Features of PTC **High-Yield:** PTC is the most common thyroid malignancy (80% of all thyroid cancers) and has the best prognosis among thyroid carcinomas. 1. **Nuclear features (diagnostic):** - Nuclear grooves (longitudinal creases) - Intranuclear pseudoinclusions (cytoplasm invaginated into nucleus) - Overlapping nuclei - Irregular nuclear membranes 2. **Architectural patterns:** - Papillary (classic) - Follicular variant - Solid/trabecular variant - Tall cell variant (more aggressive) 3. **Spread:** - Lymph node metastases (30–50% at presentation) - Distant metastases rare at presentation (lung, bone) ### Clinical Pearl **Clinical Pearl:** Even with lymph node involvement, PTC has an excellent prognosis because lymph node metastases do not significantly worsen survival outcomes. This is unique among thyroid carcinomas. ### Management Implications - **FNAC diagnosis:** Bethesda Category V (suspicious for malignancy) or VI (malignant) - **Definitive diagnosis:** Histopathology on thyroidectomy specimen - **Treatment:** Total thyroidectomy ± central neck dissection; radioactive iodine therapy for high-risk disease - **Follow-up:** TSH suppression therapy; thyroglobulin monitoring [cite:Robbins 10e Ch 24] 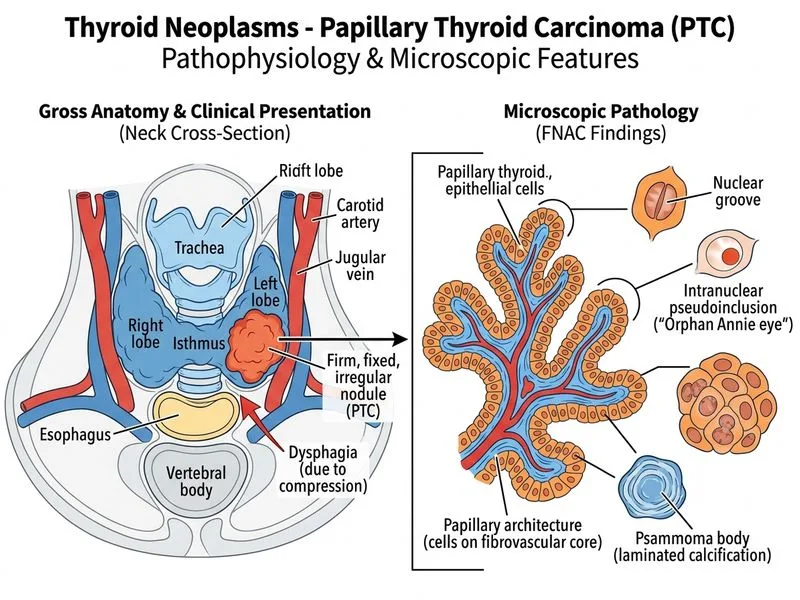
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.