## Mechanism of Hypoparathyroidism in Thyroid Surgery **Key Point:** Permanent hypoparathyroidism occurs in 0.3–1% of thyroid surgeries and is most commonly caused by devascularization of parathyroid glands, particularly the inferior parathyroids, due to excessive mobilization and stripping of their blood supply from the thyroid capsule. ### Why Devascularization is the Leading Cause 1. **Vascular anatomy**: Parathyroid glands receive their blood supply from small vessels running along the thyroid capsule 2. **Excessive mobilization**: Stripping the thyroid gland away from its capsule can disrupt these delicate vessels 3. **Inferior parathyroids at higher risk**: The inferior parathyroids have a more tenuous blood supply compared to superior parathyroids 4. **Delayed manifestation**: Devascularization may not cause immediate necrosis but gradual ischemic injury ### Clinical Presentation **High-Yield:** Hypoparathyroidism typically presents 24–72 hours post-operatively with: - Paresthesias (circumoral, fingertips) - Positive Chvostek's and Trousseau's signs - Hypocalcemia (serum Ca < 8.5 mg/dL) - Low or inappropriately normal PTH levels ### Prevention Strategies | Strategy | Mechanism | |----------|----------| | Careful capsular dissection | Preserves parathyroid blood supply | | Identification of all 4 glands | Allows selective preservation | | Minimal gland manipulation | Reduces vascular injury | | Cryopreservation (if needed) | Allows autotransplantation if glands damaged | **Clinical Pearl:** If all parathyroids appear devascularized intraoperatively, cryopreservation and autotransplantation to the sternocleidomastoid muscle or brachioradialis is a salvage option. **Tip:** In exam questions, when asked about permanent hypoparathyroidism, think "devascularization" rather than direct injury — it is the most common mechanism. 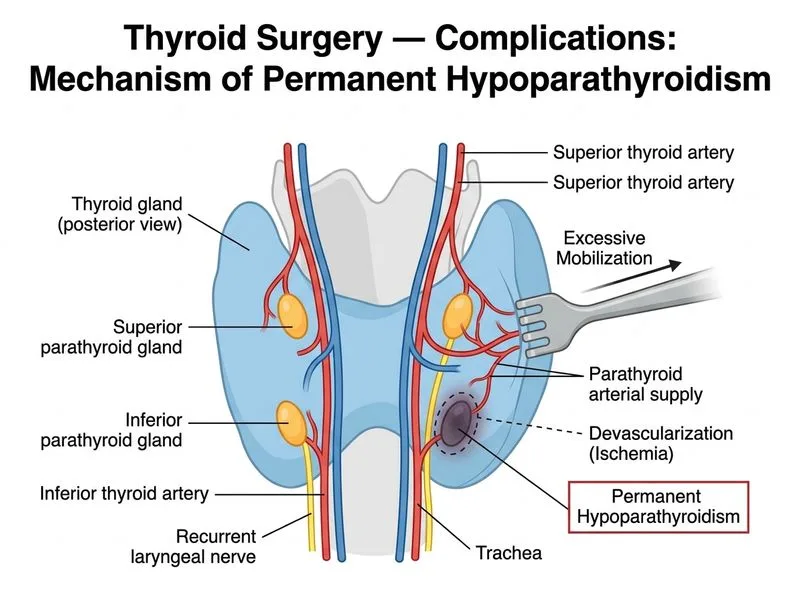
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.