## Clinical Context This patient develops **symptomatic hypocalcemia** (perioral paresthesias, Chvostek's sign, ionized calcium <7 mg/dL) on postoperative day 2 following total thyroidectomy for Graves' disease. Despite careful intraoperative identification of parathyroid glands and RLN, hypocalcemia has occurred—indicating **parathyroid dysfunction**. ## Pathophysiology of Postoperative Hypocalcemia **Key Point:** Hypocalcemia after thyroidectomy is most commonly due to **hypoparathyroidism** from parathyroid gland injury, devascularization, or inadvertent removal—not from RLN injury or vitamin D deficiency. **High-Yield:** The four parathyroid glands are at risk during thyroidectomy because: - **Superior parathyroids** lie at the level of the inferior thyroid artery and the recurrent laryngeal nerve - **Inferior parathyroids** are more variable in location but often lie within the thymic tongue - **Devascularization** (stripping of blood supply) is the most common mechanism of injury, even if the glands are not removed - **Transient hypoparathyroidism** occurs in 5–10% of thyroidectomies; **permanent hypoparathyroidism** in 0.5–2% ## Why Hypoparathyroidism Is the Answer 1. **Timing:** Symptomatic hypocalcemia on POD 2 is typical for **parathyroid injury** (not RLN injury, which causes voice changes, not hypocalcemia). 2. **Clinical Signs:** Chvostek's sign and perioral paresthesias indicate **ionized hypocalcemia** from PTH deficiency, not from other causes. 3. **Mechanism:** Even with careful dissection, parathyroid glands can be devascularized by stripping of the thyroid capsule or thermal injury from electrocautery. 4. **Serum Calcium:** A calcium of 7.2 mg/dL is consistent with acute hypoparathyroidism; vitamin D deficiency causes more gradual, milder hypocalcemia. ## Differential Diagnosis Table | Cause | Timing | Chvostek's Sign | Serum PTH | Serum PO₄ | Notes | |-------|--------|-----------------|-----------|-----------|-------| | **Hypoparathyroidism** | POD 1–2 | Positive | **Low** | **High** | Most common; may be transient | | RLN injury | POD 1+ | Negative | Normal | Normal | Causes hoarseness, not hypocalcemia | | Hungry bone syndrome | POD 1–7 | Possible | Normal/high | Low | Occurs with correction of hyperthyroidism; PTH is appropriately elevated | | Vitamin D deficiency | Gradual (weeks–months) | Negative | High (secondary) | Low | Rare acute cause; PTH elevated | **Clinical Pearl:** **Hungry bone syndrome** (rapid uptake of calcium into bone after correction of hyperthyroidism) can cause hypocalcemia, but PTH levels are **normal or elevated** as the parathyroids respond appropriately. In this case, the clinical presentation (Chvostek's sign, acute symptoms) and the surgical context (parathyroid at risk) point to **parathyroid hypofunction**, not hungry bone syndrome. ## Management Implications **Key Point:** Postoperative hypocalcemia requires: 1. **Serum PTH measurement** (low in hypoparathyroidism; normal/high in hungry bone syndrome) 2. **Serum phosphate** (high in hypoparathyroidism; low in hungry bone syndrome) 3. **Calcium supplementation** (oral or IV depending on severity) 4. **Active vitamin D** (calcitriol) if PTH is low 5. **Serial monitoring** to determine if hypoparathyroidism is transient or permanent **Mnemonic:** **CHVOSTEK** = Calcium Hypo, Vital signs (paresthesias), Osteomalacia risk, Serum PTH low, Tetany, Excitability, Kidney function (check for secondary hyperparathyroidism) [cite:Sabiston Textbook of Surgery 21e Ch 37; Harrison 21e Ch 397] 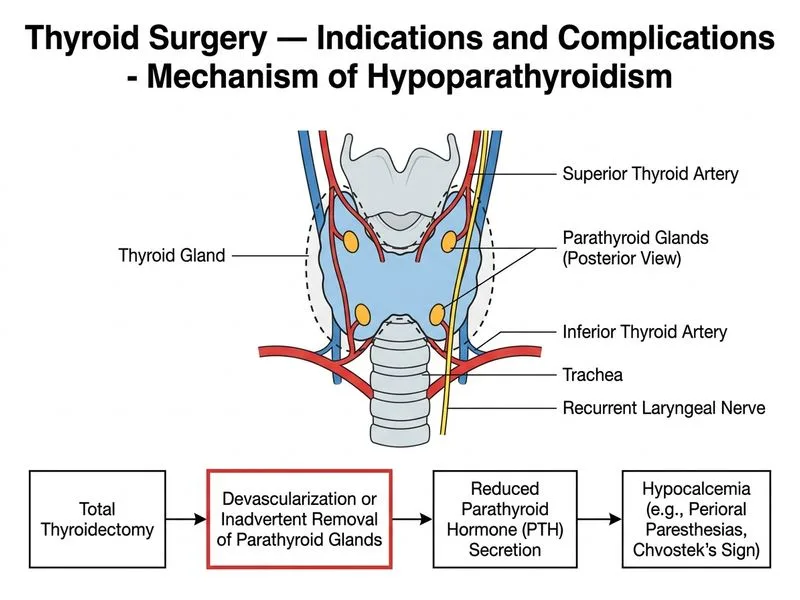
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.