## Investigation of Choice for Postoperative Hypocalcemia After Thyroidectomy ### Clinical Context The patient presents with classic signs of acute hypocalcemia (perioral paresthesia, positive Chvostek sign) on postoperative day 1 after total thyroidectomy. This clinical picture is highly suggestive of **hypoparathyroidism** due to inadvertent parathyroid gland injury or devascularization during surgery. ### Why Serum PTH and Ionized Calcium? **Key Point:** Serum PTH level is the single most important investigation to confirm hypoparathyroidism. In true hypoparathyroidism, PTH is inappropriately LOW (or low-normal) despite hypocalcemia—this is the pathognomonic finding. **High-Yield:** The PTH-calcium relationship differentiates causes of hypocalcemia: - **Hypoparathyroidism:** Low PTH + Low Ca²⁺ (parathyroid failure) - **Vitamin D deficiency:** High PTH + Low Ca²⁺ (secondary hyperparathyroidism) - **Renal disease:** High PTH + Low Ca²⁺ (tertiary hyperparathyroidism) **Clinical Pearl:** Ionized calcium (free Ca²⁺) is more accurate than total calcium in acute settings because it is not affected by albumin levels, which may fluctuate postoperatively. ### Diagnostic Algorithm for Postoperative Hypocalcemia ```mermaid flowchart TD A[Postoperative hypocalcemia<br/>after thyroidectomy]:::outcome --> B[Measure serum PTH<br/>and ionized calcium]:::action B --> C{PTH level?}:::decision C -->|Low or low-normal| D[Hypoparathyroidism<br/>Parathyroid injury/devascularization]:::outcome C -->|High| E{Vitamin D status?}:::decision E -->|Low| F[Vitamin D deficiency<br/>Secondary hyperparathyroidism]:::outcome E -->|Normal| G[Renal disease or<br/>other cause]:::outcome D --> H[Treat with IV calcium<br/>and calcitriol]:::action ``` ### Role of Other Investigations | Investigation | Role in Hypocalcemia Workup | Utility in This Case | |---|---|---| | **Serum PTH** | **Gold standard** — confirms hypoparathyroidism | **Essential — must-do** | | **Ionized calcium** | More accurate than total Ca in acute settings | **Essential — confirms hypocalcemia** | | **Serum phosphate** | Elevated in hypoparathyroidism (PTH ↓ → PO₄ ↑) | Supportive, not diagnostic | | **Alkaline phosphatase** | Nonspecific; not helpful in acute hypocalcemia | Not useful for diagnosis | | **24-hour urinary calcium** | Assesses renal handling of calcium | Not useful in acute postoperative setting | | **Vitamin D level** | Rules out vitamin D deficiency | Secondary test if PTH is high | **Warning:** Do NOT rely on serum phosphate or alkaline phosphatase alone to diagnose hypoparathyroidism. PTH is the definitive test because it directly reflects parathyroid function. **Mnemonic:** **"PTH-Ca Pair"** — Always measure PTH and calcium together. Low PTH + Low Ca = Hypoparathyroidism (parathyroid failure). High PTH + Low Ca = Secondary hyperparathyroidism (kidney or vitamin D problem). ### Management Implication Once hypoparathyroidism is confirmed (low PTH + low ionized Ca), immediate treatment with intravenous calcium gluconate (10–20 mL of 10% solution) and calcitriol (1,25-dihydroxyvitamin D₃) is initiated to prevent tetany and seizures. 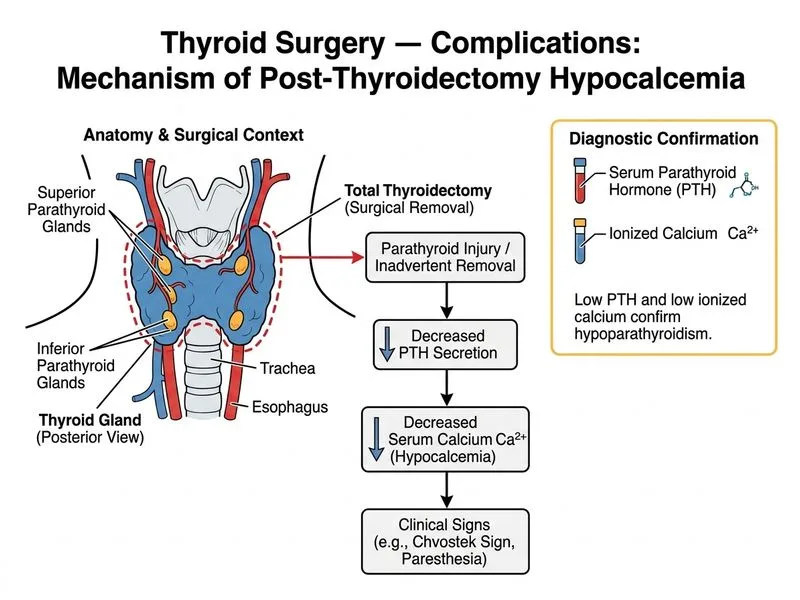
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.