## Clinical Scenario Analysis **Key Point:** Bilateral vocal cord paralysis in the immediate postoperative period after thyroidectomy, despite intraoperative RLN visualization and preservation, indicates **neuropraxia** (functional nerve injury) rather than transection. ## Mechanism of RLN Injury in Thyroidectomy ```mermaid flowchart TD A[RLN Injury During Thyroidectomy]:::outcome --> B{Mechanism?}:::decision B -->|Transection| C[Complete nerve division]:::urgent B -->|Traction| D[Stretching/compression]:::action B -->|Thermal injury| E[Heat from electrocautery]:::action D --> F[Neuropraxia: conduction block]:::outcome E --> F C --> G[Immediate permanent paralysis]:::urgent F --> H[Temporary paralysis, recovery possible]:::outcome ``` ## Differential Diagnosis: Transection vs. Neuropraxia | Feature | RLN Transection | RLN Neuropraxia | |---------|-----------------|------------------| | **Mechanism** | Complete nerve division | Traction, compression, thermal injury | | **Intraoperative finding** | Nerve visibly cut | Nerve appears intact | | **Onset** | Immediate (postop day 0–1) | Immediate (postop day 0–1) | | **Vocal cord position** | Paramedian (abducted) | Paramedian (abducted) | | **Recovery** | None (permanent) | Yes, weeks to months | | **EMG** | Denervation (fibrillations after 3 weeks) | Conduction block (normal motor units) | **High-Yield:** In this case, the surgeon **directly visualized and preserved both RLNs**, making transection unlikely. The bilateral paramedian vocal cord paralysis occurring immediately postoperatively is classic for **bilateral neuropraxia from traction or thermal injury** during dissection or electrocautery use near the nerve. ## Why Neuropraxia, Not Transection? 1. **Intraoperative visualization:** The surgeon saw and preserved both nerves—transection would require cutting despite visualization, which is unlikely. 2. **Bilateral involvement:** While bilateral RLN injury is rare (0.5–1% of thyroidectomies), it typically occurs from traction or thermal injury during aggressive dissection, not simultaneous transection of both nerves. 3. **Paramedian position:** Both cords are in the paramedian (abducted) position, consistent with RLN injury (not SLN injury, which causes high-pitched voice). 4. **Prognosis:** Neuropraxia carries a favorable prognosis for recovery over weeks to months; transection is permanent. ## Clinical Management of Bilateral RLN Neuropraxia **Clinical Pearl:** Bilateral RLN paralysis in the immediate postoperative period is a **medical emergency** if airway compromise occurs. Management includes: - Observation for airway patency; most patients tolerate paramedian cords if breathing is adequate. - If dyspnea is severe: consider tracheostomy or endoscopic procedures (laser-assisted posterior cordotomy, arytenoid abduction). - Expectant management: neuropraxia often recovers over 3–12 months as nerve conduction returns. - Voice therapy for dysphonia. ## Why Not the Other Options? **Transection (Option A):** Ruled out by intraoperative visualization and preservation of both nerves. Transection would require the surgeon to cut the nerve despite seeing it, which is inconsistent with the clinical history. **Tracheal stenosis (Option B):** Presents with dyspnea but NOT with vocal cord paralysis on laryngoscopy. Stenosis is a late complication (weeks to months), not immediate postoperative. **Thyroid storm (Option C):** Presents with fever, tachycardia, altered mental status, and hemodynamic instability—not focal vocal cord paralysis. Also, modern preoperative antithyroid preparation (PTU/methimazole + iodine) makes thyroid storm rare. 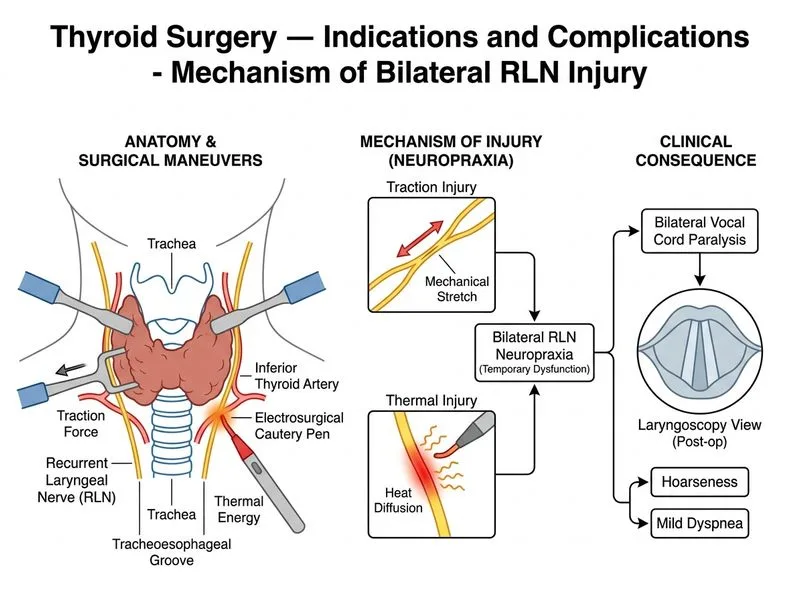
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.