## Postoperative Hypoparathyroidism After Thyroidectomy **Key Point:** Hypoparathyroidism is the most common endocrine complication of thyroidectomy, caused by inadvertent injury, devascularization, or removal of parathyroid glands. Diagnosis is confirmed by **low calcium + low PTH + high phosphate**. ### Clinical Presentation of Acute Hypocalcemia **High-Yield:** Neuromuscular manifestations of hypocalcemia appear within hours to days: - **Perioral paresthesias** (circumoral tingling) — earliest sign - **Acral paresthesias** (fingers, toes) - **Muscle cramps, tetany, seizures** (severe) - **Positive Chvostek sign** (tap facial nerve → lip twitch) - **Positive Trousseau sign** (inflate BP cuff → carpopedal spasm) ### Diagnostic Criteria for Hypoparathyroidism | Parameter | Finding | Interpretation | |---|---|---| | **Serum calcium** | 7.2 mg/dL (↓) | Hypocalcemia | | **Serum phosphate** | 4.8 mg/dL (↑) | Hyperphosphatemia (inverse relationship) | | **PTH** | 12 pg/mL (↓) | Inadequate parathyroid response | | **Magnesium** | 1.6 mg/dL (↓) | Mild hypomagnesemia (may impair PTH secretion) | **Clinical Pearl:** The triad of **low calcium + high phosphate + low PTH** is pathognomonic for hypoparathyroidism. Magnesium is also low, which can worsen PTH resistance; correction of both is essential. ### Incidence and Risk Factors ```mermaid flowchart TD A[Thyroidectomy]:::action --> B{Parathyroid<br/>Injury?}:::decision B -->|Devascularization| C[Temporary Hypoparathyroidism<br/>24-72 hrs]:::outcome B -->|Inadvertent Removal| D[Permanent Hypoparathyroidism]:::outcome C --> E[Recovery of PTH secretion]:::action D --> F[Lifelong calcium +<br/>calcitriol replacement]:::action B -->|No injury| G[Euthyroid]:::outcome ``` **Mnemonic: CHVOSTEK** — **C**ircumoral paresthesias, **H**yperreflexia, **V**asospasm (Trousseau), **O**scillations (tetany), **S**eizures, **T**etany, **E**xcitability, **K**ramps. ### Immediate Management 1. **Intravenous calcium gluconate** (10 mL of 10% solution in 50 mL 5% dextrose over 10–20 min) - Raises serum calcium acutely - Monitor cardiac rhythm (hypercalcemia risk) - Repeat every 4–6 hours until symptoms resolve 2. **Calcitriol (active vitamin D)** 0.5–1 µg PO/IV twice daily - Enhances intestinal calcium absorption - Increases renal calcium reabsorption - Onset: 4–6 hours 3. **Magnesium supplementation** (IV magnesium sulfate 1–2 g, or PO magnesium oxide) - Correct hypomagnesemia to restore PTH secretion - Magnesium <1.5 mg/dL impairs PTH response 4. **Oral calcium supplements** (calcium carbonate 1–2 g elemental calcium TID) - Maintenance therapy once acute crisis resolves **High-Yield:** Do NOT give phosphate binders in hypoparathyroidism; the elevated phosphate is a consequence of low PTH and will normalize with calcium/calcitriol replacement. ### Differential: Why Not the Other Options? **Hypomagnesemia alone** would not explain the low PTH and high phosphate. While magnesium correction is important, it is not the primary driver here. **Thyroid storm** presents with fever, tachycardia, agitation, and hyperreflexia — not perioral paresthesias or hypocalcemia. TSH and free T4 would be abnormal. **Acute kidney injury** would cause hyperphosphatemia but would also raise PTH (secondary hyperparathyroidism), not lower it. [cite:Sabiston Textbook of Surgery 21e Ch 37; Harrison 21e Ch 397] 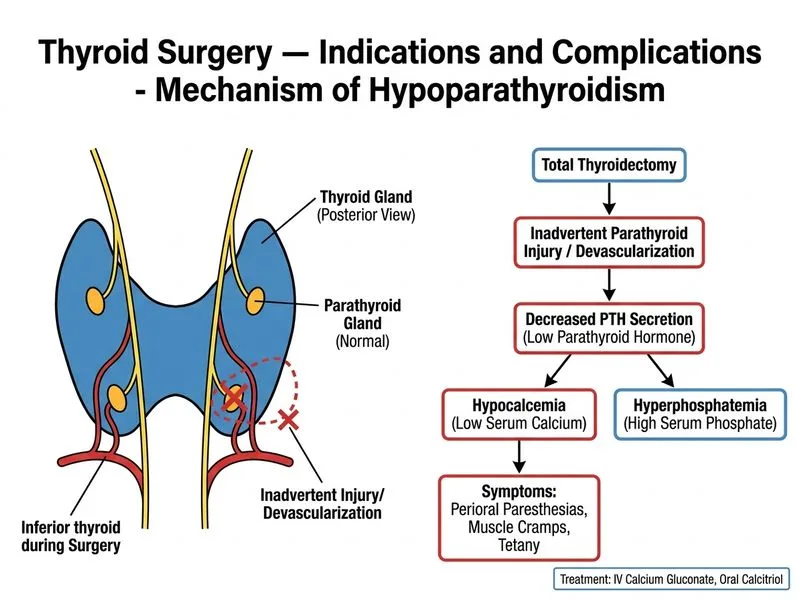
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.