## Intraoperative RLN Neuromonitoring Loss: Management Algorithm **Key Point:** Loss of neuromonitoring signal (LOS) during thyroid surgery with an anatomically intact nerve does NOT mandate immediate cessation of surgery. Per the International Neural Monitoring Study Group (INMSG) guidelines, the recommended approach is to complete the ipsilateral dissection carefully, then perform **postoperative laryngoscopy** to assess true vocal cord function before deciding on contralateral dissection. ### Why Continue Surgery (Option C) is Correct When LOS occurs and the nerve appears visually intact, the surgeon should: 1. **Systematically troubleshoot** the monitoring system (electrode position, impedance, stimulator settings) to rule out technical failure 2. **Identify and address** any reversible cause (release traction, irrigate with warm saline) 3. **Complete the ipsilateral dissection** with meticulous technique — abandoning mid-dissection may leave bleeding or incomplete resection 4. **Perform postoperative laryngoscopy** (after extubation or in recovery) — this is the **gold standard** for assessing RLN function Postoperative laryngoscopy will reveal: - **Normal vocal cord mobility** → transient conduction block (neurapraxia); reassuring prognosis - **Ipsilateral cord paralysis** → functional injury; counsel on 3–6 month recovery timeline for neurapraxia vs. permanent injury if transection occurred **Clinical Pearl (INMSG Protocol):** If LOS persists and postoperative laryngoscopy confirms ipsilateral cord paralysis, the contralateral side should NOT be operated on in the same sitting — this prevents bilateral cord paralysis. This staged approach is the cornerstone of safe bilateral thyroid surgery. *(Randolph GW et al., Laryngoscope 2011)* ### Why NOT the Other Options? - **Option A (Abort and refer):** Unnecessarily exposes the patient to a second anesthesia and operative risk when the nerve is anatomically intact and the ipsilateral dissection can be safely completed - **Option B (Immediate intraoperative laryngoscopy):** Under general anesthesia, vocal cords are relaxed and immobile regardless of nerve function — intraoperative laryngoscopy cannot reliably assess cord mobility and is NOT the standard of care. Postoperative assessment after extubation is required for meaningful evaluation - **Option D (Steroid injection around nerve):** No evidence-based role in acute intraoperative LOS; may obscure tissue planes and complicate dissection; not recommended in any guideline ### Summary Table | Scenario | Action | |---|---| | LOS + nerve anatomically intact | Complete ipsilateral side; postop laryngoscopy | | Postop laryngoscopy: normal | Proceed with contralateral side if needed | | Postop laryngoscopy: cord paralysis | Stage contralateral surgery; do NOT proceed same sitting | **High-Yield:** The key distinction is that intraoperative neuromonitoring LOS guides *surgical decision-making* (especially regarding the contralateral side), while *postoperative laryngoscopy* is the definitive assessment of actual nerve function. *(Randolph GW, Dralle H; INMSG Guidelines, Laryngoscope 2011)* 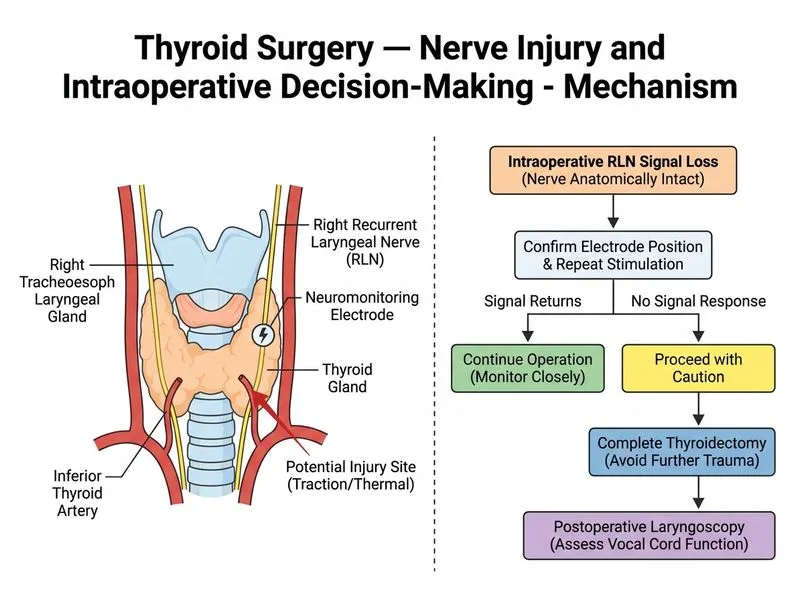
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.