## Differential Diagnosis of Intraoperative Vocal Cord Immobility ### Clinical Presentation Interpretation The key finding is **adduction of the right vocal cord with immobility**. This is the classic presentation of **recurrent laryngeal nerve (RLN) injury**, not superior laryngeal nerve (SLN) injury. **High-Yield:** Distinguishing RLN from SLN injury by vocal cord position: | Nerve | Vocal Cord Position | Function Lost | Voice Quality | |-------|-------------------|---------------|---------------| | **RLN** | Adducted (paramedian) | Abduction, all intrinsic muscles except cricothyroid | Hoarse, weak, breathy | | **SLN** (external branch) | Paramedian, slight abduction | Cricothyroid (tension) | High-pitched voice loss, fatigue | **Key Point:** The RLN innervates all intrinsic laryngeal muscles except the cricothyroid (which is SLN external branch). RLN injury → vocal cord assumes a paramedian adducted position due to unopposed cricothyroid action and loss of posterior cricoarytenoid (the only abductor). ### Why This Is RLN Injury 1. **Anatomical course:** The RLN has a longer course than the SLN and is at greater risk during thyroid lobe mobilization, particularly near the inferior thyroid artery. 2. **Mechanism:** During lobe mobilization, traction on the lobe can stretch the RLN, which loops under the aorta on the left and under the subclavian artery on the right. 3. **Timing:** The injury occurred during lobe mobilization, before deliberate SLN dissection, making RLN the likely culprit. ### Management Algorithm ```mermaid flowchart TD A[Intraoperative vocal cord adduction/immobility]:::outcome --> B{RLN or SLN injury?}:::decision B -->|RLN: adducted cord| C[Release traction immediately]:::action B -->|SLN: minimal abduction| D[Assess cricothyroid function]:::action C --> E{Function recovered?}:::decision E -->|Yes| F[Continue dissection with careful technique]:::action E -->|No| G[Assess for transection]:::decision G -->|Transection confirmed| H[Primary repair or graft if feasible]:::action G -->|Stretch/contusion| I[Complete surgery, document injury]:::action D --> J[Complete surgery carefully]:::action F --> K[Complete lobectomy]:::action H --> K I --> K J --> K K --> L[Postoperative voice assessment]:::outcome ``` ### Best Next Step: Release Traction and Reassess **Clinical Pearl:** Intraoperative RLN injury from traction is often **reversible** if the traction is released promptly. The nerve may recover function within minutes to hours if it is stretched but not transected. 1. **Immediate action:** Release all traction on the right lobe. 2. **Reassess:** Repeat laryngoscopy to determine if vocal cord function returns. 3. **If function returns:** Proceed with careful dissection, avoiding further traction. 4. **If function does not return:** Explore the nerve for transection or severe contusion; consider primary repair if transection is confirmed. ### Why Other Options Are Incorrect **Option 0 (SLN injury):** The adducted vocal cord position is diagnostic of RLN injury, not SLN injury. SLN injury would present with a cord in a more abducted position and loss of voice pitch/tension, not adduction. **Option 1 (Abort procedure):** Aborting the procedure is premature. Intraoperative exploration and release of traction may restore function. Aborting wastes the opportunity for immediate intervention and requires a second anesthesia exposure. **Option 3 (Complete lobectomy with SLN injury):** This misidentifies the nerve and suggests completing surgery without investigating the injury. Even if it were SLN injury (which it is not), completing surgery without exploration would be suboptimal. **Warning:** Continuing dissection without releasing traction risks converting a reversible stretch injury into a permanent transection or severe contusion. 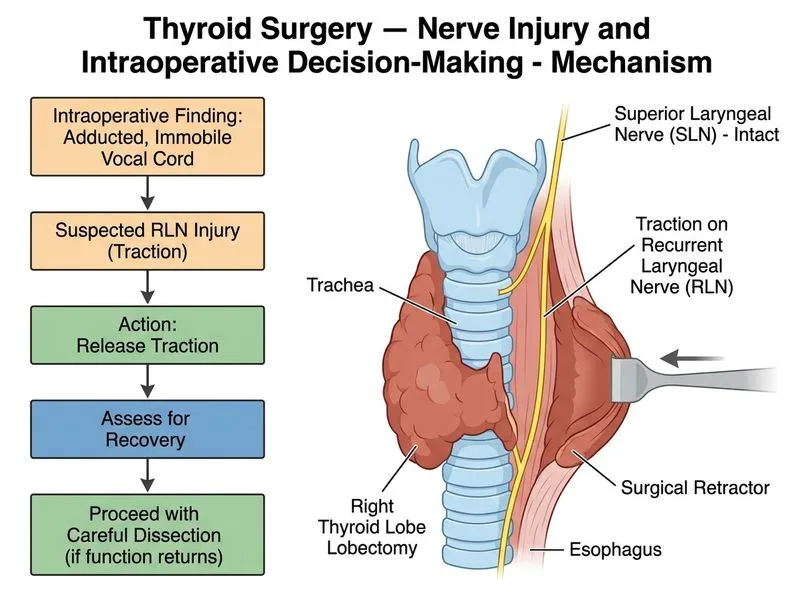
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.