## Diagnosis: Tinea Capitis (Non-Inflammatory Type) ### Overview of Tinea Capitis **Key Point:** Tinea capitis is a dermatophyte infection of the scalp and hair shaft, most common in children but can occur at any age. It accounts for ~10% of all dermatophyte infections. ### Classification of Tinea Capitis by Inflammatory Pattern | Type | Appearance | Symptoms | Organisms | Prognosis | |------|-----------|----------|-----------|----------| | **Non-inflammatory (Ectothrix)** | Scaling, broken hairs, minimal erythema | Asymptomatic or mild pruritus | *T. mentagrophytes*, *M. canis*, *M. audouinii* | Good; responds to topical ± systemic | | **Inflammatory (Endothrix)** | Pustules, nodules, severe erythema, kerion | Pruritus, pain, drainage | *T. violaceum*, *T. tonsurans*, *T. schoenleinii* | Requires systemic therapy; risk of scarring alopecia | | **Black dot** | Broken hairs at scalp level, black dots | Minimal inflammation | *T. tonsurans*, *T. violaceum* | Chronic; easy to miss clinically | **High-Yield:** **Trichophyton mentagrophytes** is the classic organism for **non-inflammatory tinea capitis** with broken hairs and scaling but minimal inflammation or pruritus. ### Why This Case Fits Tinea Capitis (Non-Inflammatory) 1. **Positive fungal culture for *T. mentagrophytes*** — definitive diagnosis 2. **Well-demarcated patches of alopecia** — characteristic of tinea capitis 3. **Broken hairs at the surface** — hyphae invade the hair shaft (ectothrix pattern) 4. **Erythema and fine scaling** — dermatophyte inflammation 5. **Absence of pruritus** — typical of non-inflammatory variant 6. **3-month duration** — subacute presentation consistent with dermatophyte infection ### Pathophysiology ```mermaid flowchart TD A[Dermatophyte spore exposure]:::outcome --> B[Colonization of hair follicle]:::action B --> C{Inflammatory response?}:::decision C -->|Minimal| D[Non-inflammatory tinea capitis]:::outcome C -->|Marked| E[Inflammatory tinea capitis/Kerion]:::urgent D --> F[Broken hairs, scaling, alopecia]:::outcome E --> F2[Pustules, nodules, drainage, scarring risk]:::urgent ``` ### Diagnostic Methods - **KOH mount:** Branching septate hyphae within/around hair shaft - **Fungal culture:** Gold standard; identifies organism and guides therapy - **Wood's lamp:** Non-fluorescent (except *M. audouinii* and *M. canis*, which fluoresce blue-green) - **Dermoscopy:** Comma-shaped hairs, zigzag hairs, black dots ### Management **Non-inflammatory tinea capitis:** - **Topical antifungals** (selenium sulfide shampoo, ketoconazole shampoo) — adjunctive only - **Systemic antifungals** (terbinafine 125–250 mg daily × 4–6 weeks, or griseofulvin 20 mg/kg/day × 6–12 weeks) — required for cure **Inflammatory tinea capitis/Kerion:** - **Systemic antifungals** (mandatory) - **Oral corticosteroids** (to reduce inflammation and risk of permanent scarring alopecia) **Clinical Pearl:** Tinea capitis is contagious; close contacts (especially children) should be screened and treated prophylactically if infected. [cite:Fitzpatrick's Dermatology 9e Ch 130] 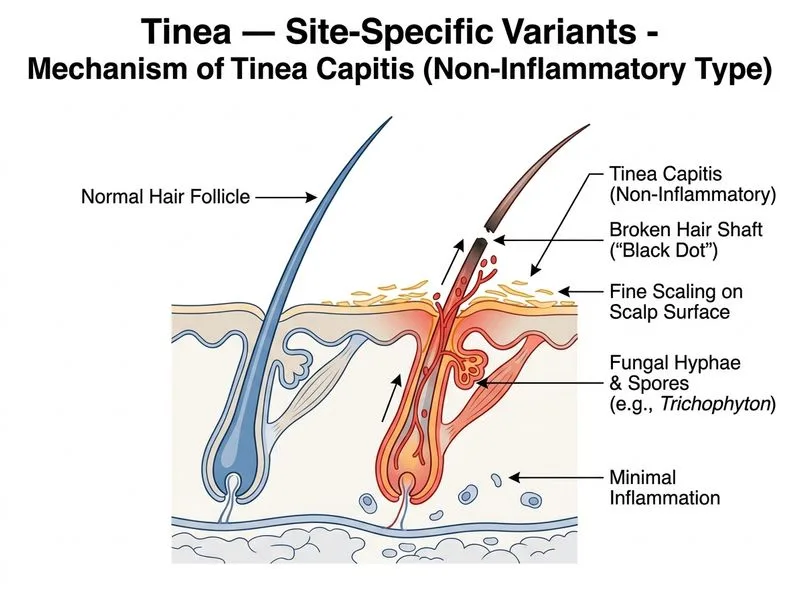
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.