## Diagnosis: Tinea Cruris ### Clinical Presentation **Key Point:** Tinea cruris is a dermatophyte infection of the groin, scrotum, perineum, and inner thighs—classically presenting with intense pruritus, erythema, and well-demarcated borders with central clearing. ### Diagnostic Features | Feature | Tinea Cruris | Candidiasis | Erythrasma | |---------|-------------|------------|----------| | **Border** | Sharp, advancing, raised | Ill-defined, maceration | Diffuse, non-raised | | **Satellite lesions** | Pustules (typical) | Vesicles/pustules | Absent | | **KOH mount** | Branching septate hyphae | Budding yeast + pseudohyphae | Negative | | **Wood's lamp** | Negative | Negative | Coral-red fluorescence | | **Predisposing factors** | Warm, moist, occlusive environment | Diabetes, immunosuppression | Erythrasma (Corynebacterium minutissimum) | ### Key Clinical Pearls **High-Yield:** Tinea cruris is the second most common dermatophyte infection (after tinea pedis) and is more common in males. The condition is exacerbated by: - Warm, humid climates (common in India) - Occlusive clothing - Profuse sweating - Poor hygiene **Clinical Pearl:** The presence of **satellite pustules** at the periphery of the lesion is pathognomonic for tinea cruris and helps distinguish it from candidiasis (which typically shows vesicles and maceration). **Warning:** Topical corticosteroids (as used by this patient) can worsen tinea cruris by suppressing local immunity and promoting fungal growth—a common clinical trap. ### Organism - *Trichophyton rubrum* (most common, ~70% of cases) - *Trichophyton mentagrophytes* - *Epidermophyton floccosum* ### Management 1. **Topical azoles** (miconazole, clotrimazole) for 2–4 weeks 2. **Oral terbinafine** (250 mg daily × 2–4 weeks) if extensive or refractory 3. **Hygiene measures:** Keep area dry, loose clothing, antifungal powder 4. **Avoid corticosteroids** (worsen infection) [cite:Park 26e Ch 12] 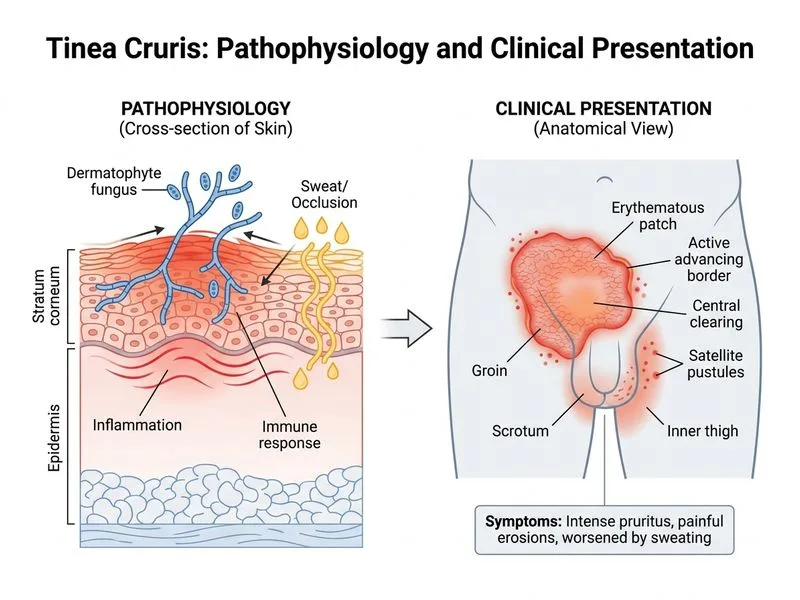
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.