## Diagnosis: Tinea Cruris **Key Point:** Tinea cruris is a dermatophyte infection of the groin and upper inner thighs, classically sparing the scrotum — a cardinal distinguishing feature from candidiasis. ### Clinical Features of Tinea Cruris - **Location:** Groin, inner thighs, inguinal folds, lower abdomen - **Sparing of scrotum:** Pathognomonic for tinea cruris; candidiasis typically involves the scrotum - **Morphology:** Well-demarcated erythematous plaques with raised, scaly, advancing border and central clearing - **Symptoms:** Intense pruritus and burning; worse with sweating and friction - **Risk factors:** Warm, moist environment; occlusion; male predominance (3:1); tropical/subtropical climates ### Causative Organisms | Organism | Prevalence | Geography | Notes | |----------|-----------|-----------|-------| | *Trichophyton rubrum* | Most common (60–70%) | Worldwide | Anthropophilic | | *Trichophyton mentagrophytes* | Common (15–20%) | Worldwide | Zoophilic | | *Epidermophyton floccosum* | Less common | Tropical regions | Anthropophilic | **High-Yield:** *T. rubrum* is the most common cause of tinea cruris globally and in India. ### Microscopy & Culture - **KOH mount:** Branching, septate hyphae (as in this case) - **Culture:** Grows on Sabouraud dextrose agar; colonies are white to cream-colored, slow-growing - **Wood's lamp:** No fluorescence (unlike erythrasma, which shows coral-red) ### Differential Diagnosis | Condition | Scrotum Involvement | KOH Mount | Wood's Lamp | Key Feature | |-----------|-------------------|----------|------------|-------------| | Tinea cruris | Spared | Septate hyphae | Negative | Raised border, central clearing | | Candidiasis | Involved | Budding yeast + pseudohyphae | Negative | Satellite pustules, maceration | | Erythrasma | May involve | Negative | Coral-red fluorescence | Fine scale, non-inflammatory | | Tinea corporis | Variable | Septate hyphae | Negative | Annular lesions, can be anywhere | **Clinical Pearl:** The **sparing of the scrotum** is the single most useful clinical discriminator between tinea cruris and candidiasis in a male patient with groin involvement. ### Management - **Topical:** Azoles (miconazole, clotrimazole) or terbinafine cream for 2–4 weeks - **Systemic:** Terbinafine 250 mg daily × 2–4 weeks or itraconazole 200 mg daily × 2 weeks for extensive/refractory disease - **Adjuncts:** Keep area dry, avoid occlusion, antifungal powder **Mnemonic:** **SCROTUM SPARED** = Tinea cruris (not candidiasis). 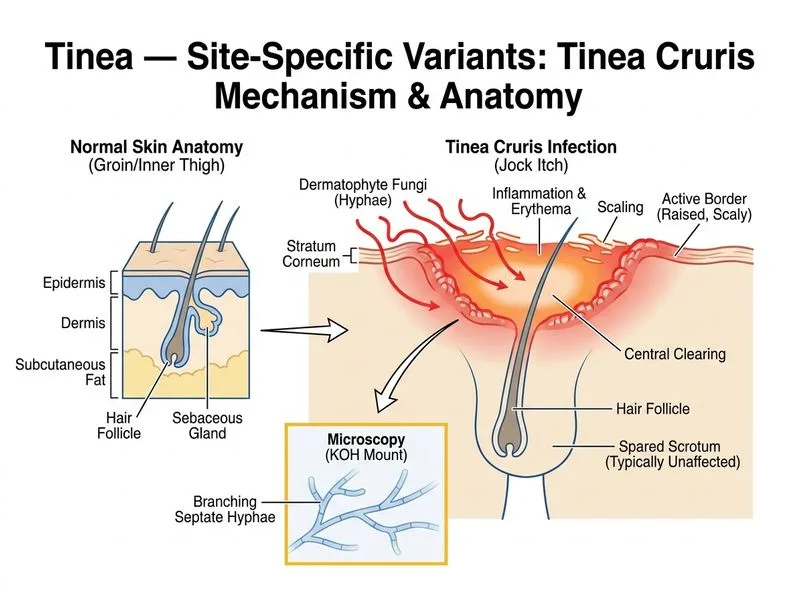
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.