## Diagnosis: Acute Bacterial Tonsillitis (Group A Streptococcal) **Key Point:** The positive RADT for Group A Streptococcus (GAS) in a patient with classic acute tonsillitis (fever, exudate, cervical lymphadenopathy, no airway compromise) confirms bacterial infection and mandates antibiotic therapy. Absence of trismus and uvular deviation rules out peritonsillar abscess. ## Outpatient vs. Inpatient Management | Feature | Outpatient (Oral Abx) | Inpatient (IV Abx) | |---------|----------------------|-------------------| | **Airway compromise** | None | Present or imminent | | **Systemic toxicity** | Mild–moderate | Severe (sepsis, dehydration) | | **Ability to swallow** | Adequate for oral meds | Severely impaired | | **Complications** | No signs of abscess/Lemierre | Suspected abscess or deep neck space infection | | **Social factors** | Reliable follow-up | Unreliable, homeless, or immunocompromised | This patient has **no airway compromise, no trismus, no uvular deviation**—all signs are absent. She is a suitable candidate for **outpatient oral antibiotic therapy**. ## First-Line Antibiotic Regimen **Mnemonic:** **PEN-V-TEN** = **Penicillin V** for **10 days** (standard GAS tonsillitis). | Drug | Dose | Duration | Notes | |------|------|----------|-------| | **Penicillin V** | 500 mg QID (or 250 mg QID for children) | 10 days | First-line, excellent GAS coverage, low cost | | **Amoxicillin** | 500 mg TDS | 10 days | Alternative, better taste, same efficacy | | **Cephalexin** | 500 mg QID | 10 days | If penicillin allergy (non-anaphylaxis) | | **Erythromycin** | 500 mg QID | 10 days | If true penicillin allergy (anaphylaxis) | **High-Yield:** RADT-positive patients should receive antibiotics immediately without waiting for culture confirmation. Culture is useful only if RADT is negative (to rule out false negatives in high-risk populations). ## Supportive Care - Throat lozenges, warm salt-water gargles - Paracetamol or ibuprofen for fever and pain - Adequate hydration (oral fluids, IV if unable to swallow) - Rest ## When to Escalate to Admission ```mermaid flowchart TD A[GAS-positive Acute Tonsillitis]:::outcome --> B{Airway compromise or severe toxicity?}:::decision B -->|Yes| C[Admit for IV antibiotics & monitoring]:::urgent B -->|No| D{Signs of abscess or deep neck space infection?}:::decision D -->|Yes| E[Admit, imaging, drainage]:::urgent D -->|No| F[Outpatient oral antibiotics]:::action F --> G[Follow-up in 48–72 hours]:::action G --> H{Improving?}:::decision H -->|Yes| I[Continue oral antibiotics to day 10]:::action H -->|No| J[Reassess for complications, consider admission]:::action ``` **Clinical Pearl:** The 10-day course is critical to eradicate GAS and prevent post-streptococcal sequelae (acute rheumatic fever, post-streptococcal glomerulonephritis), not just to resolve symptoms. [cite:Harrison 21e Ch 309], [cite:Robbins & Cotran 10e Ch 16] 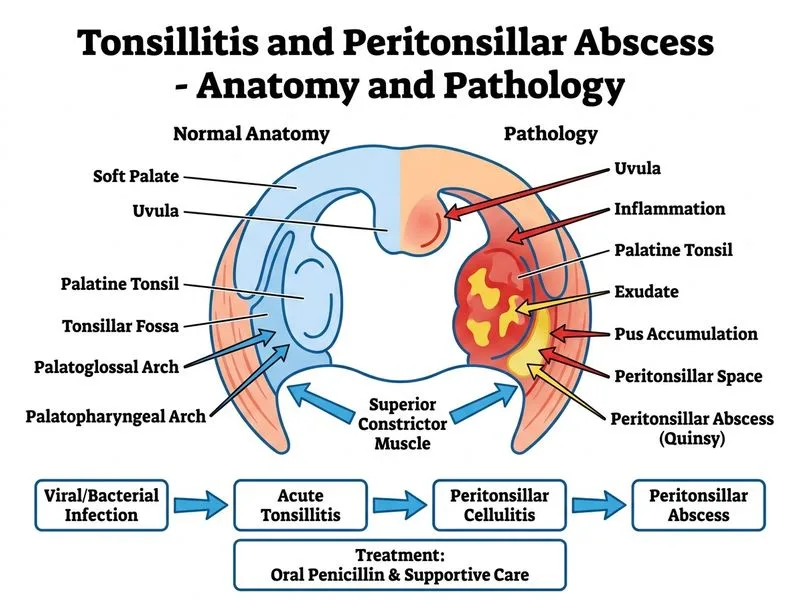
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.