## Management of Acute Tonsillitis: Viral vs. Bacterial ### Clinical Presentation Analysis **Key Point:** The absence of uvula deviation and soft palate bulge rules out peritonsillar abscess. The bilateral exudative tonsillitis with splenomegaly and lymphadenopathy suggests a **viral etiology** (likely infectious mononucleosis or EBV). ### Differential Diagnosis: Viral vs. Bacterial Tonsillitis | Feature | Viral Tonsillitis | Bacterial Tonsillitis (GAS) | |---------|-------------------|-----------------------------| | **Onset** | Gradual (2–3 days) | Acute (1–2 days) | | **Exudate** | Often present, may be thick | Yellow/white, confluent | | **Uvula deviation** | Absent | Absent (unless abscess forms) | | **Splenomegaly** | Common (EBV, CMV) | Rare | | **Cervical lymphadenopathy** | Marked, tender | Present but less prominent | | **Systemic symptoms** | Malaise, myalgia, headache | Fever, sore throat dominant | | **Culture** | Negative for GAS | Positive for Group A Streptococcus | | **Management** | Supportive care | Antibiotics (penicillin/amoxicillin) | ### Why Supportive Care Is Appropriate Here **High-Yield:** The **Centor criteria** help identify patients likely to have bacterial (GAS) tonsillitis and who benefit from antibiotics: 1. Fever ≥38°C ✓ 2. Exudate ✓ 3. Absence of cough ✓ (implied) 4. Tender anterior cervical lymphadenopathy ✓ 5. **Age 3–14 years** (this patient is 35 — scores lower) **Mnemonic:** **FETAL** (Fever, Exudate, Tender nodes, Age 3–14, Lack of cough) With a Centor score of 3–4 in an adult, the pre-test probability of GAS is **moderate**, but the **splenomegaly strongly suggests viral etiology** (EBV/infectious mononucleosis). ### Management Algorithm for Acute Tonsillitis ```mermaid flowchart TD A[Acute tonsillitis presentation]:::outcome --> B{Signs of abscess?}:::decision B -->|Yes: uvula deviation, soft palate bulge| C[Peritonsillar abscess]:::urgent C --> D[Immediate drainage + antibiotics]:::action B -->|No| E{Centor score or clinical features?}:::decision E -->|High score + no splenomegaly| F[Likely bacterial GAS]:::outcome F --> G[Empirical antibiotics]:::action E -->|Moderate/low score or splenomegaly| H[Likely viral]:::outcome H --> I[Supportive care, culture pending]:::action I --> J{Culture positive for GAS?}:::decision J -->|Yes| K[Start antibiotics]:::action J -->|No| L[Continue supportive care]:::action ``` ### Why Drainage Procedures Are NOT Indicated **Clinical Pearl:** Needle aspiration and incision-drainage are reserved for **peritonsillar abscess** (which this patient does NOT have). Draining uncomplicated tonsillitis risks: - Unnecessary trauma - Bleeding - Infection of the drainage site - No therapeutic benefit ### Appropriate Supportive Management 1. **Analgesics:** Paracetamol or ibuprofen for pain and fever 2. **Hydration:** Encourage fluids; consider IV fluids if unable to swallow 3. **Throat lozenges/gargles:** Salt water or topical anesthetics 4. **Throat culture:** Pending results guide antibiotic use 5. **Observation:** Monitor for signs of abscess formation (uvula deviation, dysphagia worsening) **High-Yield:** **Antibiotics should NOT be given empirically in suspected viral tonsillitis** — they increase resistance, cost, and adverse effects without benefit. Reserve antibiotics for confirmed or highly probable bacterial infection. ### When to Start Antibiotics - **Positive throat culture for GAS** → Start amoxicillin or penicillin V - **High Centor score (≥3) in child or young adult** → Consider empirical antibiotics - **Clinical deterioration or signs of abscess** → Antibiotics + drainage ### Why Tonsillectomy Is Not Immediate Tonsillectomy is considered **electively** after recurrent episodes (≥5–7 per year) or if there is **chronic tonsillar hypertrophy causing airway obstruction**. Acute tonsillitis is NOT an indication for emergency tonsillectomy. 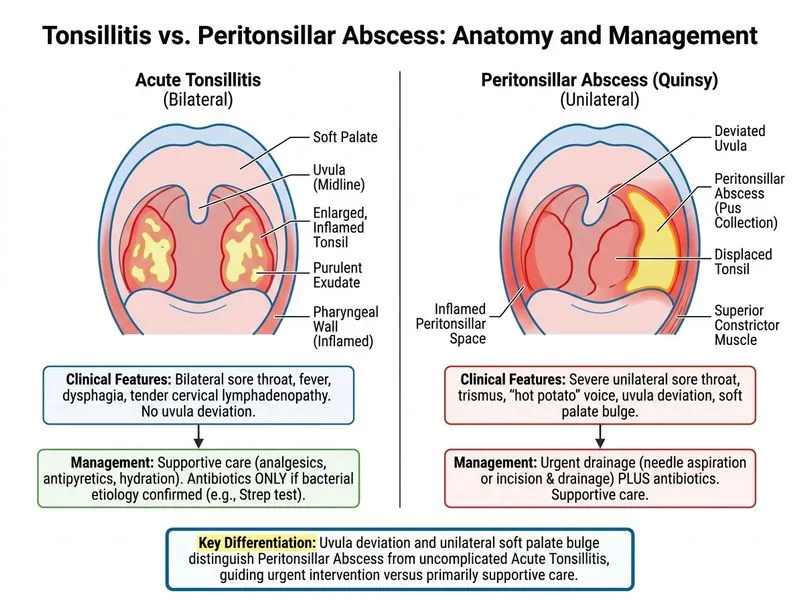
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.