## Management of Peritonsillar Abscess: Drainage ### Clinical Context This patient has developed a peritonsillar abscess (PTA) despite appropriate antibiotic therapy. The diagnosis is confirmed by: - Unilateral soft palate bulging - Medial displacement of tonsil - Muffled voice ("hot potato voice") - Worsening symptoms despite antibiotics - Progression from acute tonsillitis ### Management Algorithm ```mermaid flowchart TD A["Peritonsillar Abscess Diagnosed"]:::outcome --> B{"Airway patent?"}:::decision B -->|"Yes"| C["Needle aspiration or I&D"]:::action B -->|"No/Threatened"| D["Secure airway first"]:::urgent D --> E["Tracheostomy or intubation"]:::action C --> F["Send pus for culture"]:::action F --> G["Escalate antibiotics"]:::action G --> H["Elective tonsillectomy 4-6 weeks later"]:::action H --> I["Prevent recurrence"]:::outcome ``` **Key Point:** Drainage (needle aspiration or incision and drainage) is the definitive treatment for peritonsillar abscess. Antibiotics alone are insufficient once abscess has formed. ### Why Drainage is Essential 1. **Antibiotics cannot penetrate abscess wall** — loculated pus has poor antibiotic penetration 2. **Symptom relief** — immediate decompression of pressure 3. **Culture and sensitivity** — guides targeted antibiotic therapy 4. **Prevention of complications** — reduces risk of airway obstruction, Lemierre's syndrome, or mediastinitis ### Drainage Techniques | Technique | Indications | Advantages | Disadvantages | |-----------|-------------|-----------|----------------| | **Needle aspiration** | Cooperative patient, clear diagnosis | Minimal trauma, office procedure | May need repeat if inadequate drainage | | **Incision & drainage (I&D)** | Large abscess, immunocompromised, failed aspiration | Complete drainage, therapeutic and diagnostic | Requires local anesthesia, slight bleeding risk | | **Ultrasound-guided aspiration** | Unclear diagnosis, loculation | Precise localization | Requires ultrasound availability | **High-Yield:** In India, needle aspiration under topical anesthesia is the most commonly performed first-line drainage procedure in ENT outpatient settings. ### Antibiotic Escalation Post-Drainage - **Initial therapy:** Amoxicillin (as given) - **Post-drainage escalation:** Amoxicillin-clavulanate or clindamycin (covers anaerobes and beta-lactamase producers) - **Culture-directed therapy:** Adjust based on pus culture and sensitivity - **Duration:** 10–14 days total **Clinical Pearl:** Always send aspirated pus for Gram stain, culture, and sensitivity — polymicrobial infection (including anaerobes) is common in PTA. ### Follow-up: Elective Tonsillectomy - Performed 4–6 weeks after acute phase resolves - Reduces recurrence risk (up to 30% without tonsillectomy) - Timing allows inflammation to subside and reduces operative bleeding risk **Warning:** Do NOT perform emergency tonsillectomy during acute abscess phase — high risk of hemorrhage and spread of infection. [cite:Harrison 21e Ch 309; Robbins & Cotran 10e Ch 16] 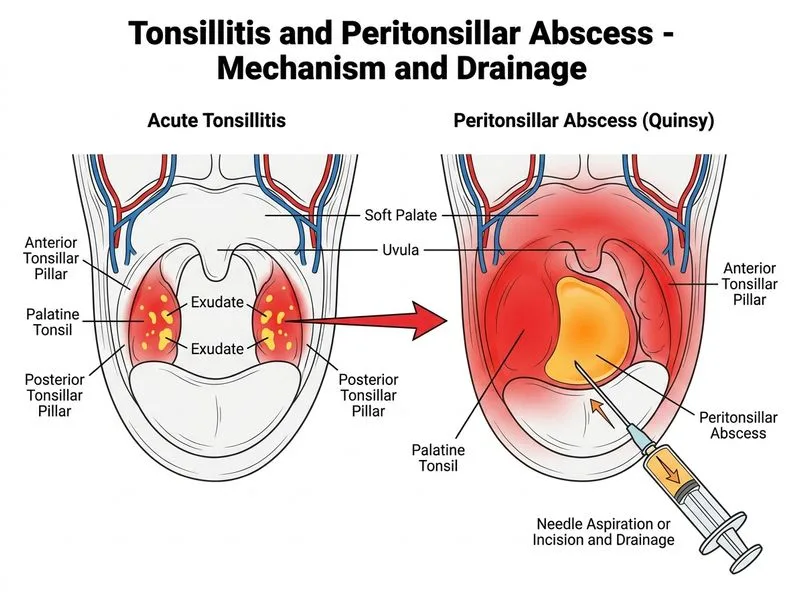
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.