## Clinical Diagnosis The clinical presentation—unilateral tonsillar enlargement with medial displacement, soft palate pushed downward and medially, and a palpable bulge in the lateral pharyngeal wall—is pathognomonic for **peritonsillar abscess (PTA)**. ## Management Principle **Key Point:** Peritonsillar abscess is a surgical emergency requiring immediate drainage. Antibiotics alone are insufficient and delay increases risk of airway compromise, mediastinitis, and sepsis. ## Why Needle Aspiration or I&D? 1. **Diagnostic confirmation**: Aspiration yields purulent material and allows culture/sensitivity. 2. **Therapeutic drainage**: Relieves pressure, reduces airway obstruction risk, and promotes healing. 3. **Timing**: Should be performed urgently under local anesthesia (or general if airway at risk). 4. **Success rate**: Needle aspiration has ~85% success; if unsuccessful, formal incision and drainage follows. ## Post-Drainage Management - High-dose IV antibiotics (e.g., ceftriaxone 1–2 g BD + metronidazole 500 mg TDS) covering Group A Streptococcus, anaerobes, and Staph aureus. - Airway monitoring and ICU admission if signs of airway compromise. - Elective tonsillectomy 4–6 weeks after resolution (to prevent recurrence). **High-Yield:** Observation or antibiotics alone in PTA risks **airway obstruction, mediastinitis, and Lemierre syndrome** (septic thrombophlebitis of internal jugular vein). **Clinical Pearl:** The "hot potato voice" (muffled, thick voice) and difficulty handling saliva are red flags for imminent airway compromise. 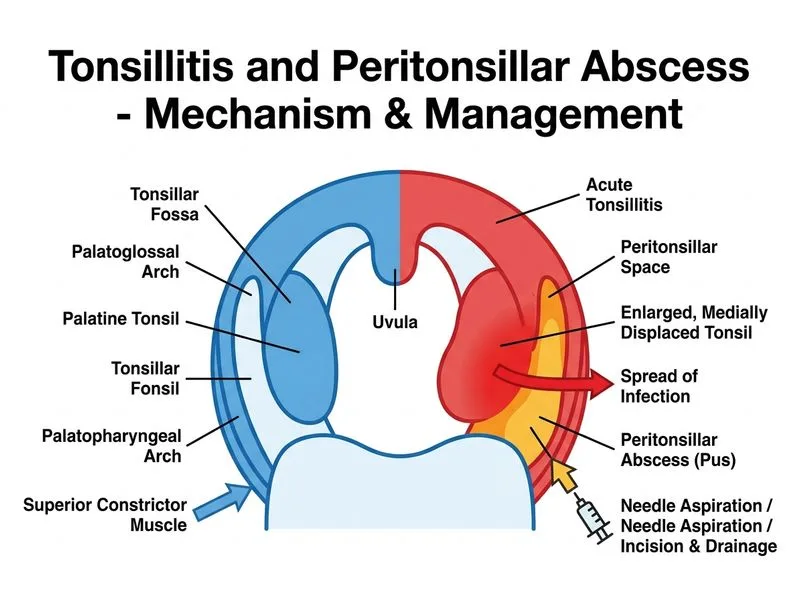
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.