## Clinical Context A 72-year-old woman on postoperative day 3 after tracheostomy presents with blood-stained secretions and mild bleeding from the stoma. She is hemodynamically stable and afebrile. The timing (POD 3) and clinical stability are crucial clues. ## Differential Diagnosis of Tracheostomy Bleeding | Complication | Timing | Presentation | Hemodynamic Status | Management | |---|---|---|---|---| | **Tube-related trauma / granulation** | POD 1–7 | Mild–moderate bleeding, blood-stained secretions | Stable | Increase tube size, topical hemostasis, monitor | | **Tracheal stenosis** | Weeks–months | Stridor, dyspnea, NOT acute bleeding | Stable | Serial dilation, corticosteroids | | **Tracheoinnominate fistula** | POD 3–7 (classically) | **Massive hemorrhage**, hemodynamic collapse, sentinel bleeding → exsanguination | **Unstable** | Emergency clamping, hyperinflation, surgical exploration | ## Why Granulation Tissue Bleeding is Correct **Key Point:** Early postoperative bleeding (POD 1–7) from a tracheostomy is most commonly due to tube-related trauma, granulation tissue formation, or minor mucosal bleeding. The patient is hemodynamically stable with only mild bleeding, making a minor source most likely. **High-Yield:** Tracheoinnominate artery fistula is a **rare but catastrophic** complication (incidence ~0.5%) that typically presents with: - Massive hemorrhage ("herald bleed" followed by exsanguination) - Hemodynamic instability - Usually POD 3–7 but can occur weeks later - Often associated with tube placement too low or cuff over-inflation **Clinical Pearl:** The presence of hemodynamic stability and mild bleeding argues against tracheoinnominate fistula. Granulation tissue and minor trauma are far more common causes of early postoperative oozing. ## Management Algorithm ```mermaid flowchart TD A[Tracheostomy bleeding POD 3]:::outcome --> B{Hemodynamic status?}:::decision B -->|Unstable + massive bleed| C[Tracheoinnominate fistula]:::urgent C --> D[Clamp tube, hyperinflate cuff, emergency surgery]:::action B -->|Stable + mild bleeding| E[Granulation tissue / tube trauma]:::outcome E --> F[Increase tube size]:::action F --> G[Apply topical hemostatic agents]:::action G --> H[Monitor closely, suction gently]:::action H --> I{Bleeding persists?}:::decision I -->|Yes| J[Consider rigid bronchoscopy, cautery]:::action I -->|No| K[Continue routine care]:::action ``` **Rationale:** Increasing the tube size reduces movement and friction at the stoma. Topical hemostatic agents (epinephrine-soaked gauze, thrombin, or topical hemostats) promote clotting. Gentle suctioning and close monitoring allow time for hemostasis. If bleeding persists despite these measures, rigid bronchoscopy with cautery or laser ablation may be needed. [cite:Cummings Otolaryngology 6e Ch 82; Schwartz Principles of Surgery 11e Ch 13] 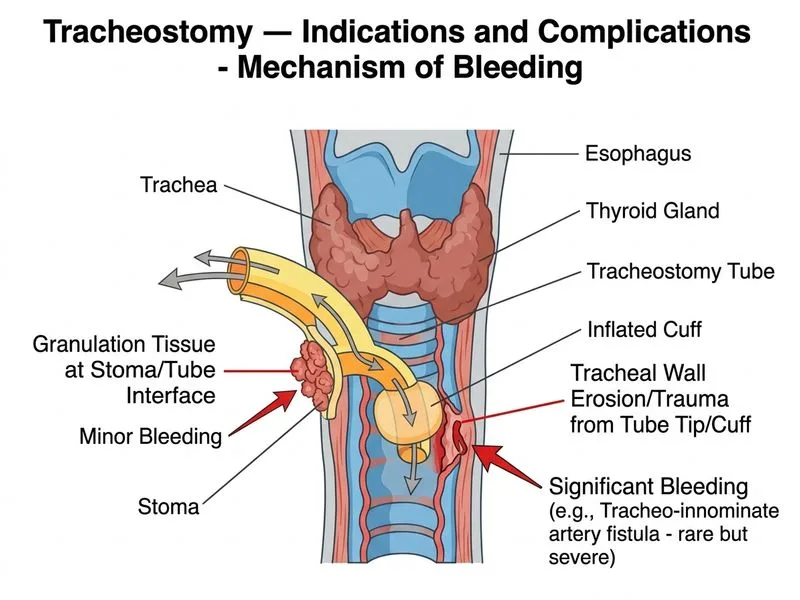
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.