## Distinguishing Tracheostomy Indications: Chronic Ventilation vs. Airway Obstruction ### Core Distinction **Key Point:** The fundamental difference lies in the **expected duration of airway support** and the underlying pathophysiology requiring intervention. ### Comparison Table | Feature | COPD with Ventilator Dependence | Bilateral Vocal Cord Paralysis | |---------|----------------------------------|-------------------------------| | **Primary indication** | Prolonged mechanical ventilation (weeks–months) | Permanent upper airway obstruction | | **Duration of tracheostomy** | May be temporary; weaning possible | Permanent; reversal unlikely | | **Underlying pathology** | Respiratory muscle fatigue, CO₂ retention | Fixed airway narrowing | | **Reversibility** | Potentially reversible with rehabilitation | Irreversible without surgery | | **Timing** | Elective, after failed weaning trials | Urgent, to relieve stridor | ### Why Duration Distinguishes Them **High-Yield:** In COPD patients requiring ventilatory support, tracheostomy is indicated when **weaning from mechanical ventilation fails after 7–10 days** or when prolonged support (>2–3 weeks) is anticipated. The procedure facilitates easier suctioning, reduces sedation needs, and improves comfort during what may be a temporary phase of dependence. In bilateral vocal cord paralysis, the tracheostomy is a **permanent solution** to bypass the fixed obstruction at the glottis. The vocal cords will not recover function without surgical intervention (e.g., arytenoidectomy, laser cordotomy), making the tracheostomy indefinite. ### Clinical Pearl **Clinical Pearl:** COPD patients may eventually be decannulated if respiratory status improves or if they adapt to non-invasive ventilation. Vocal cord paralysis patients rarely achieve decannulation without additional laryngeal surgery, making the distinction in *permanence* clinically crucial for counselling and long-term planning. ### Why Other Options Are Incorrect - **Presence of upper airway obstruction:** Both conditions can involve upper airway issues (COPD may have concurrent tracheomalacia; vocal cord paralysis is inherently obstructive), so this does not uniquely discriminate. - **Need for mechanical ventilation:** COPD requires it; vocal cord paralysis typically does not (unless there is concurrent respiratory failure), but this is not the *best* discriminator of the indication itself. - **Risk of aspiration:** Both conditions carry aspiration risk (COPD from reduced consciousness/sedation; vocal cord paralysis from incomplete glottic closure), and aspiration is not the primary indication for tracheostomy in either. 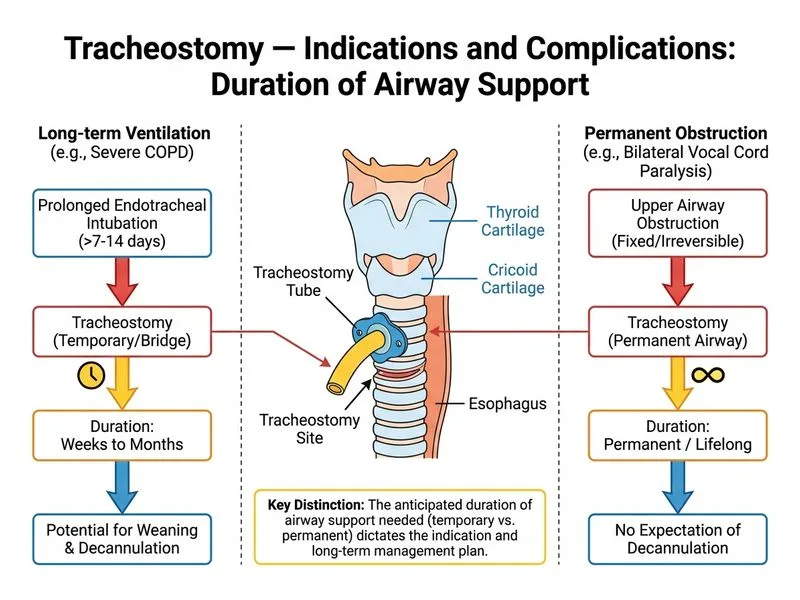
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.