## Distinguishing Early Hemorrhage from Chronic Infection in Tracheostomy ### Core Distinction **Key Point:** The **anatomical source of bleeding/drainage** is the critical discriminator. Early hemorrhage (especially life-threatening) typically involves the **innominate artery**, while chronic infection involves **local granulation tissue and secondary bacterial colonization**. ### Comparison Table | Feature | Early Hemorrhage (POD 5) | Chronic Infection/Granulation | |---------|--------------------------|------------------------------| | **Timing** | Days 3–7 (early); days 7–21 (late) | Weeks to months after placement | | **Primary source** | Innominate artery erosion (life-threatening) or tube-related mucosal bleeding | Local granulation tissue, chronic inflammation | | **Character of bleeding** | Brisk, pulsatile (if innominate); can be massive | Oozing, purulent drainage; slow bleeding | | **Associated findings** | Hemodynamic instability (if innominate); no fever initially | Purulent drainage, granulation tissue, local erythema; low-grade fever possible | | **Pathophysiology** | Tube erosion into vessel; pressure necrosis | Chronic irritation, biofilm formation, secondary infection | | **Management** | Emergent: tube repositioning, hyperinflation cuff, surgical exploration ± ligation | Conservative: local care, topical agents, antibiotics; rarely surgical | ### Why Vessel Involvement Distinguishes Them **High-Yield:** **Early hemorrhage** (especially on POD 5) is classically due to **innominate artery erosion**—a surgical emergency. The tube tip erodes through the anterior tracheal wall into the artery, causing potentially exsanguinating bleeding. This is a **vascular complication** requiring immediate intervention (cuff hyperinflation, tube repositioning, or surgical ligation). **Chronic infection/granulation** arises from **persistent irritation and biofilm colonization** of the stoma and surrounding tissue. Granulation tissue is a normal inflammatory response to the chronic foreign body; secondary bacterial infection (often *Pseudomonas*, *Staphylococcus*) causes purulent drainage. This is a **tissue-level complication** managed with local care, topical antibiotics, and tube hygiene. ### Clinical Pearl **Clinical Pearl:** Innominate artery erosion classically presents with **herald bleeding** (small amounts of blood in secretions) followed by massive hemorrhage. The **Innominate Artery Syndrome** is a surgical emergency; immediate measures include hyperinflating the cuff to tamponade the vessel and advancing the tube into the distal trachea. Chronic granulation, by contrast, is benign and self-limiting with proper stoma care. ### Why Other Options Are Incorrect - **Timing of onset:** While timing *does* differ (early vs. late), it is not the *best* discriminator because both can occur at variable intervals. The *type* of complication (vascular vs. tissue) is more specific. - **Presence of fever and systemic toxicity:** Early hemorrhage from innominate artery erosion does NOT typically cause fever; the patient presents with shock and hemodynamic instability. Chronic infection may cause low-grade fever, but absence of fever does not rule out either complication. - **Response to topical antibiotics and local care:** Chronic granulation responds well to conservative management, but early hemorrhage does not—it requires emergency intervention. This is a *management* feature, not a *discriminating finding*. ### Mnemonic **Mnemonic:** **VESSEL vs. TISSUE** - **V**ascular (early, POD 3–7): **E**rosion of **S**ignificant **S**tructure (innominate artery) → **E**mergency - **T**issue (chronic, weeks–months): **I**nflammation, **S**econdary infection, **S**low ooze, **U**sually benign, **E**asy management 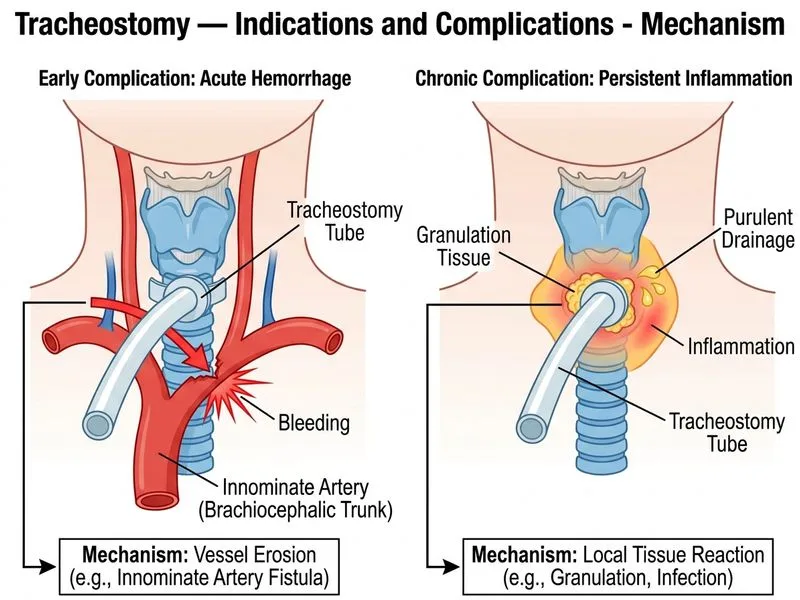
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.