## Clinical Presentation Analysis **Key Point:** The combination of purulent secretions, fever, subcutaneous emphysema, and pneumomediastinum indicates a **tracheal perforation with mediastinitis** — a late complication of tracheostomy. ## Pathophysiology of Tracheal Perforation **High-Yield:** Tracheal perforation after tracheostomy occurs due to: 1. **Tube pressure necrosis** — prolonged contact between the cuff and tracheal wall causes ischemic necrosis (typically at the cuff site) 2. **Tube migration** — if the tube erodes through the tracheal wall, it can perforate the anterior trachea 3. **Timing** — usually occurs 1–4 weeks post-tracheostomy (this patient is at 4 weeks, the peak risk window) 4. **Infection** — secondary bacterial colonization of the perforation leads to mediastinitis ## Clinical Features of Tracheal Perforation | Feature | Mechanism | |---|---| | **Purulent secretions** | Infection of the perforation site | | **Subcutaneous emphysema** | Air tracking from trachea into neck soft tissues | | **Pneumomediastinum** | Air dissecting into the mediastinum (CXR finding) | | **Fever** | Mediastinitis (infection of mediastinal tissues) | | **Foul odor** | Anaerobic bacterial overgrowth | **Clinical Pearl:** Mediastinitis is a surgical emergency with high mortality (20–40%) if not treated promptly. The presence of pneumomediastinum on CXR is a red flag. ## Management Algorithm ```mermaid flowchart TD A[Suspected tracheal perforation]:::outcome --> B[Confirm with CT neck/chest + contrast]:::action B --> C{Size & location of defect?}:::decision C -->|Small < 5mm, stable| D[Conservative: antibiotics, airway control]:::action C -->|Large or unstable| E[Surgical repair: primary closure ± flap]:::action E --> F[Reinforce with muscle/soft tissue]:::action A --> G[Blood cultures, broad-spectrum antibiotics]:::action A --> H[Imaging: CT chest for mediastinitis]:::action H --> I{Mediastinitis present?}:::decision I -->|Yes| J[Urgent surgical drainage + repair]:::urgent I -->|No| K[Medical management + close monitoring]:::action ``` **Diagnostic Confirmation:** - **CT neck/chest with IV contrast** — shows air in mediastinum, defines perforation site - **Bronchoscopy** — visualizes the defect in the tracheal wall - **Blood cultures** — identify causative organisms (often mixed aerobic/anaerobic) ## Why Other Options Are Incorrect **Tracheo-innominate artery fistula (Option 0):** - **Presentation:** Massive hemorrhage ("herald bleed" followed by catastrophic bleeding), not purulent secretions - **Timing:** Usually occurs 3–5 days post-tracheostomy (earlier than this patient's 4-week presentation) - **Imaging:** Would show active bleeding on CT angiography, not pneumomediastinum alone - **Mechanism:** Erosion of the tube tip into the innominate artery (low in the neck), not tracheal perforation **Tracheal stenosis with tube migration (Option 1):** - **Presentation:** Progressive dyspnea, stridor, difficulty decannulating — NOT acute fever, emphysema, or mediastinitis - **Timing:** Stenosis develops weeks to months after tracheostomy, not acutely - **Imaging:** CXR shows narrowing at the cuff site, not pneumomediastinum - **Pathology:** Fibrotic narrowing of the trachea, not perforation **Tube obstruction with aspiration pneumonia (Option 3):** - **Presentation:** Respiratory distress, cough, hypoxia — NOT subcutaneous emphysema or pneumomediastinum - **Imaging:** CXR shows infiltrate in lung fields (pneumonia), not air in mediastinum - **Mechanism:** Blocked tube prevents ventilation; does not cause air leak into tissues - **Secretions:** Purulent sputum is expected, but foul odor and emphysema point to a deeper process ## Management of This Patient 1. **Immediate:** Broad-spectrum IV antibiotics (cover anaerobes: e.g., piperacillin-tazobactam or clindamycin + fluoroquinolone) 2. **Imaging:** CT chest with IV contrast to confirm mediastinitis 3. **Surgical consultation:** Urgent ENT + Cardiothoracic surgery for tracheal repair and mediastinal drainage 4. **Airway:** Consider repositioning the tracheostomy tube above the perforation site or temporary intubation 5. **Definitive repair:** Primary closure of the tracheal defect with reinforcement (muscle flap, pericardium) **High-Yield:** Mediastinitis from tracheal perforation is a surgical emergency. Delay in diagnosis and treatment significantly increases mortality. [cite:Cummings Otolaryngology 6e Ch 97; Harrison 21e Ch 297] 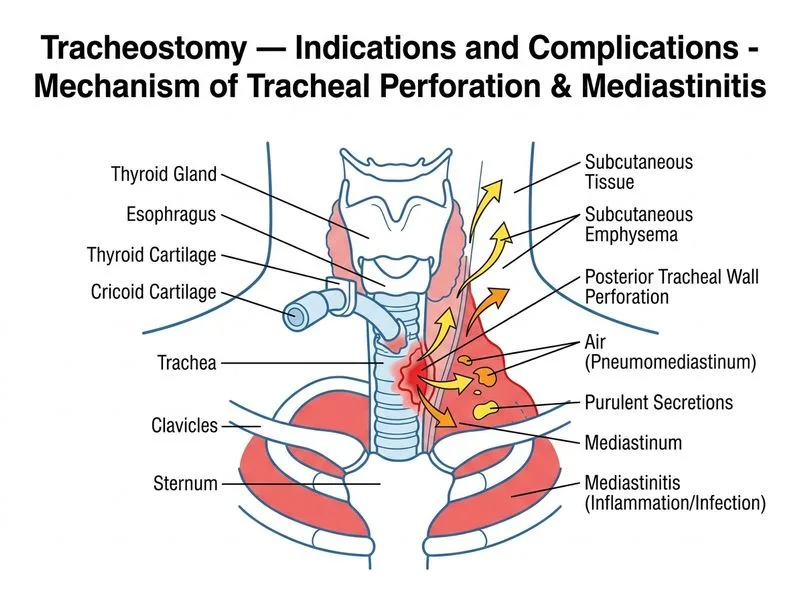
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.