## Clinical Presentation Analysis The patient presents with classic signs of **tracheal perforation** occurring in the immediate post-operative period (48 hours post-laryngectomy): ### Key Clinical Features **High-Yield:** The triad of acute respiratory distress, subcutaneous emphysema, and sudden gush of air from the surgical site is pathognomonic for tracheal perforation. **Key Point:** Tracheal perforation is a catastrophic complication that can occur during: - Intubation trauma (especially with high-pressure cuffs) - Surgical manipulation during laryngectomy or tracheostomy - Thermal injury from electrocautery - Ischemic necrosis from excessive dissection ### Mechanism in This Case During total laryngectomy with subglottic tumor extension, the surgeon must carefully dissect around the proximal trachea. Excessive traction, thermal injury from monopolar cautery, or inadvertent full-thickness laceration can breach the tracheal wall. The immediate post-operative period (first 48–72 hours) is when such injuries become clinically apparent as: 1. Air leakage into the mediastinum and subcutaneous tissues → subcutaneous emphysema 2. Loss of airway seal → acute respiratory compromise 3. Visible air egress from the surgical site ### Diagnostic Confirmation **Clinical Pearl:** Loss of the normal tracheal air column on CT imaging indicates disruption of the tracheal wall integrity. ### Management Immediate steps: - Secure the airway (intubation distal to the perforation or emergency tracheostomy) - Broad-spectrum antibiotics (mediastinitis risk) - Urgent surgical exploration and primary repair with muscle flap coverage (sternohyoid or sternocleidomastoid) - Drain placement for mediastinal/subcutaneous collections **Warning:** Delayed recognition can lead to mediastinitis, sepsis, and death. This is a surgical emergency. [cite:Cummings Otolaryngology 6e Ch 106] 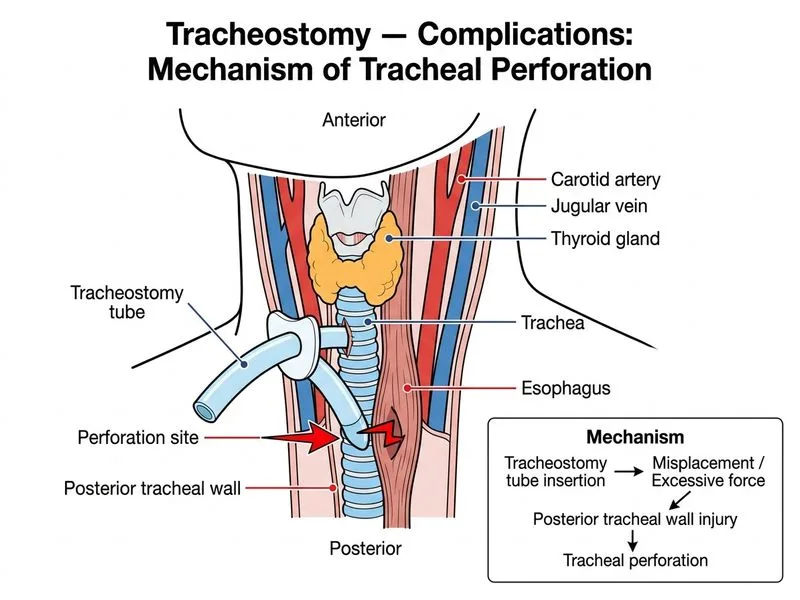
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.