## Clinical Presentation Analysis **Key Point:** Subcutaneous emphysema in the immediate postoperative period after tracheostomy is usually a **self-limited complication** caused by air dissecting into soft tissues during tube insertion or from minor tracheal trauma. ## Pathophysiology of Postoperative Subcutaneous Emphysema 1. **Mechanism:** Air escapes from the trachea into the loose areolar tissue of the neck and mediastinum during or immediately after tracheostomy. 2. **Timing:** Typically appears within 24–48 hours postoperatively. 3. **Clinical Features:** - Palpable crepitus over neck and chest - Mild dyspnea (from mass effect, not airway obstruction) - Mediastinal air on imaging 4. **Prognosis:** Usually resolves spontaneously as air is reabsorbed over 7–10 days. ## Why This Is NOT a Surgical Emergency **High-Yield:** The presence of a **patent tracheostomy tube with good bilateral air entry** rules out: - Significant tracheal stenosis (would cause stridor/obstruction) - Tube malposition (would cause unilateral air entry or subcutaneous air from cuff leak) - Tracheoesophageal fistula (would present with aspiration, not isolated emphysema) **Clinical Pearl:** Subcutaneous emphysema alone, in the absence of fever, mediastinitis signs, or airway obstruction, does NOT require intervention beyond observation. ## Management Algorithm ```mermaid flowchart TD A[Postoperative subcutaneous emphysema + patent tracheostomy]:::outcome --> B{Airway patent?}:::decision B -->|Yes, good air entry| C[Observe with serial CXR]:::action B -->|No, stridor/obstruction| D[Investigate stenosis/malposition]:::urgent C --> E{Fever or sepsis signs?}:::decision E -->|Yes| F[Broad-spectrum antibiotics + imaging]:::action E -->|No| G[Conservative management, resolves in 7-10 days]:::outcome D --> H[Bronchoscopy ± tube repositioning]:::action ``` ## Comparison: Postoperative Tracheostomy Complications | Complication | Timing | Presentation | Management | |---|---|---|---| | **Subcutaneous emphysema** | Immediate (24–48 h) | Crepitus, mild dyspnea, patent airway | Observation, serial CXR | | **Tube malposition** | Immediate | Unilateral air entry, stridor, hypoxia | Reposition or replace tube | | **Tracheal stenosis** | Weeks to months | Progressive stridor, fixed obstruction | Bronchoscopy, dilation, stent | | **Tracheoesophageal fistula** | Days to weeks | Aspiration, cough with feeding, sepsis | Urgent surgical repair | | **Mediastinitis** | Days | Fever, chest pain, hemodynamic instability | Antibiotics, drainage, imaging | **Mnemonic:** **SAFE OBSERVATION** = **S**ubcutaneous **A**ir **F**rom **E**ntry **O**bserve **B**ilateral **S**ounds **E**xclude **R**eal **V**ascular **A**nd **T**racheal **I**njury **O**n **N**ext imaging ## Why Other Options Are Incorrect - **Tracheal stenosis (Option A):** Stenosis develops over weeks to months, not 2 days postoperatively. The patient has good bilateral air entry, ruling out obstruction. - **Tube malposition with perforation (Option B):** Malposition would present with unilateral air entry, stridor, or hypoxia. The tube is patent with bilateral air entry. Needle aspiration of mediastinal air is not standard care. - **Tracheoesophageal fistula (Option D):** TEF presents with aspiration during feeding, cough, and signs of sepsis — not isolated subcutaneous emphysema. It develops days to weeks later, not immediately. 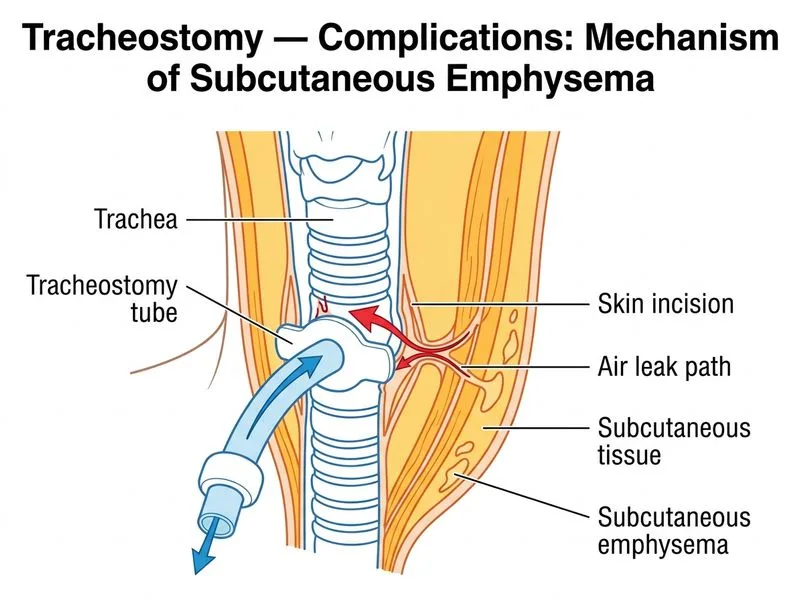
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.