## Distinguishing Early Stenosis from Tube Obstruction ### Clinical Context Both early tracheostomy stenosis (fibroblastic response at cuff site, 2–4 weeks post-procedure) and tube obstruction present with respiratory difficulty, but their **response to intervention** is the key discriminator. ### Key Differentiating Feature **Key Point:** Tube obstruction is a **mechanical problem** — cleaning, suctioning, or tube repositioning relieves symptoms acutely. Stenosis is a **structural/inflammatory problem** — symptoms persist despite tube patency because the lumen itself is narrowed. ### Comparison Table | Feature | Tube Obstruction | Early Stenosis | |---------|------------------|----------------| | **Onset** | Acute (hours to days) | Gradual (2–4 weeks) | | **Response to tube cleaning** | Complete resolution | No improvement | | **Response to tube removal** | Symptoms resolve | Symptoms persist or worsen | | **Endoscopic finding** | Patent tube, mucus/blood plugging | Narrowed subglottic/tracheal lumen | | **Pathology** | Secretion/clot obstruction | Fibroblastic proliferation, scarring | ### Clinical Pearl **Clinical Pearl:** The **gold standard test** for both is flexible laryngoscopy or bronchoscopy. In tube obstruction, the scope passes easily once the tube is removed; in stenosis, the narrowed lumen is visible and the scope meets resistance. ### High-Yield Mechanism **High-Yield:** Early stenosis results from: 1. Cuff pressure causing mucosal ischemia 2. Fibroblastic proliferation at the cuff site (weeks 2–4) 3. Progressive collagen deposition and scar contracture This is **irreversible** without intervention (dilation, laser, or surgical reconstruction). ### Why Option 1 is Correct Persistent stridor and dyspnea **despite tube cleaning and repositioning** indicates the tube itself is patent but the airway is structurally narrowed — the hallmark of stenosis, not obstruction. 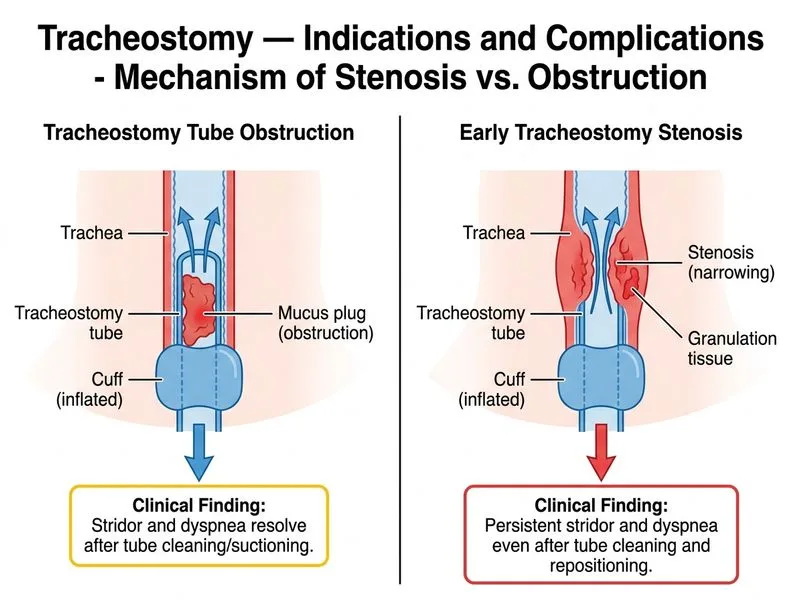
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.