## Secondary vs. Idiopathic Trigeminal Neuralgia ### Clinical Distinction | Feature | Idiopathic TN | Secondary TN (Symptomatic) | |---------|---------------|---------------------------| | **Sensory/motor findings** | Neurologically normal | Sensory loss, motor weakness, or other neurological deficits | | **Age of onset** | Typically > 50 years | Can occur at any age; often younger | | **Imaging findings** | Normal or vascular loop only | Tumor, MS lesion, vascular malformation, or other structural lesion | | **Bilateral involvement** | Rare (< 5%) | More common; suggests MS or bilateral pathology | | **Associated symptoms** | Pain only | Headache, hearing loss, gait disturbance, etc. | | **Response to medication** | Usually good (CBZ, PHT) | Variable; may require surgical intervention | ### High-Yield Discriminator **Key Point:** The **presence of objective neurological signs** (sensory loss, motor weakness, diminished corneal reflex, or other CN deficits) is the single best clinical discriminator between idiopathic and secondary trigeminal neuralgia. In idiopathic TN, the neurological examination is **entirely normal** except for pain. **Warning:** Do not confuse the *quality* of pain (sharp, lancinating) or the *trigger* (touch, chewing) with the presence of structural disease. Both idiopathic and secondary TN present with identical pain characteristics; the key is **objective neurological deficit**. **Clinical Pearl:** When a patient with trigeminal neuralgia presents with sensory loss, diminished corneal reflex, or weakness of the muscles of mastication, always suspect a **secondary cause** (tumor, MS, vascular malformation, Charcot-Marie-Tooth disease). Imaging (MRI with CISS sequences) is mandatory in such cases. **Mnemonic — Red flags for secondary TN:** **ABCD** - **A**bnormal neuro exam (sensory loss, weakness) - **B**ilateral pain (suggests MS or systemic disease) - **C**hildhood or young adult onset - **D**eficits beyond pain (hearing loss, ataxia) ### Pathophysiology Idiopathic TN is thought to result from demyelination of the trigeminal root caused by vascular compression, but this does **not** cause structural damage severe enough to produce sensory loss. Secondary TN, by contrast, involves actual compression, infiltration, or destruction of nerve tissue, leading to objective deficits. 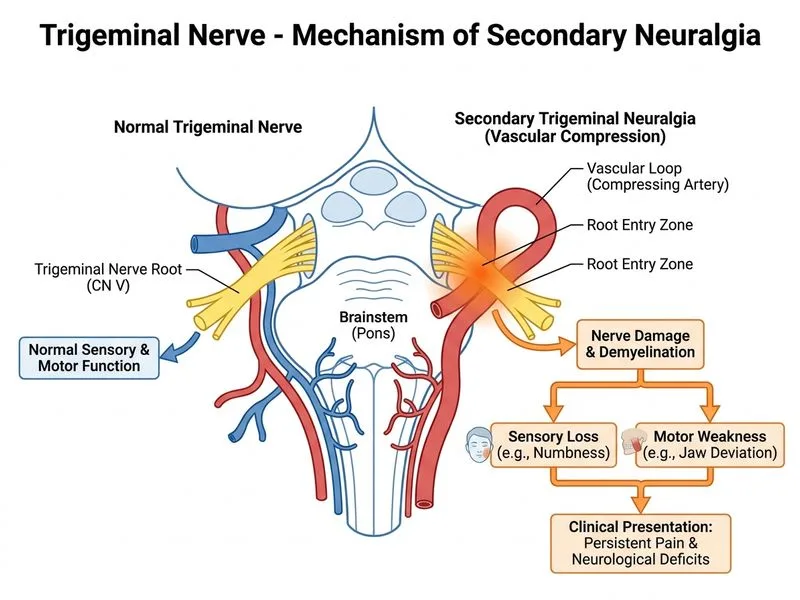
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.