## Distinguishing Trigeminal Neuralgia from Post-Herpetic Neuralgia ### Key Clinical Differences **Key Point:** The character and trigger of pain are the most reliable discriminators between TN and PHN in the trigeminal region. | Feature | Trigeminal Neuralgia | Post-Herpetic Neuralgia | |---------|---------------------|------------------------| | **Pain character** | Sudden, lancinating, electric-shock-like | Continuous, burning, aching | | **Trigger** | Light touch, chewing, cold wind (trigger zones) | Spontaneous; worsened by light touch (allodynia) | | **Duration of episodes** | Seconds to 2 minutes | Hours to continuous | | **Preceding rash** | None | Vesicular rash in acute herpes zoster | | **Age of onset** | Typically >50 years | Any age, but more common in elderly | | **Pathophysiology** | Vascular compression of trigeminal root | Nerve damage from varicella-zoster virus | ### Why This Distinction Matters **Clinical Pearl:** TN is characterized by **sudden, triggered, brief paroxysmal pain**, whereas PHN is **continuous or frequent spontaneous pain with allodynia**. This difference drives management: TN responds to carbamazepine; PHN requires gabapentin, pregabalin, or topical agents. **High-Yield:** The presence of a **trigger** (eating, talking, touching the face, cold wind) that provokes sudden, severe pain lasting seconds is pathognomonic for TN. PHN lacks such discrete triggers and instead presents with constant background pain punctuated by spontaneous exacerbations. ### Mechanism **Trigeminal Neuralgia:** Typically caused by neurovascular compression (often superior cerebellar artery) leading to demyelination and ectopic firing at the root entry zone. **Post-Herpetic Neuralgia:** Results from direct viral destruction of nerve fibers and dorsal root ganglia, causing permanent neuropathic changes and central sensitization. 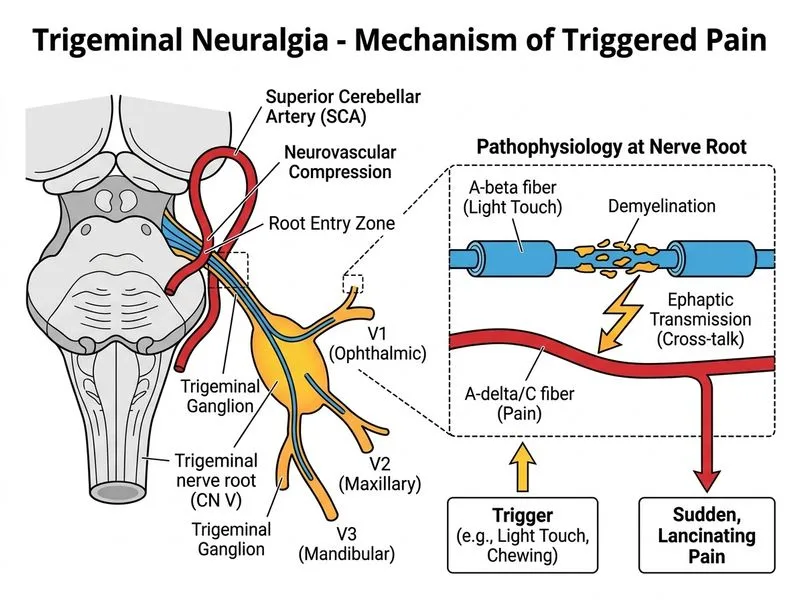
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.