## Diagnosis: Miliary Tuberculosis ### Clinical Presentation The patient presents with: - **6-month subacute course** (not acute) - **Negative sputum smear** (3 occasions) — indicates **non-cavitary disease** - **Constitutional symptoms** (fever, cough, dyspnea) - **Bilateral, symmetrical fine nodules** on imaging - **Hilar lymphadenopathy** This constellation is classic for **miliary TB**, a form of disseminated tuberculosis. ### Radiological Features of Miliary TB **Key Point:** Miliary TB is characterized by: 1. **Diffuse micronodules**: 1–3 mm diameter ("millet seed" appearance) 2. **Bilateral and symmetrical distribution** 3. **Upper and middle zone predominance** (though can be diffuse) 4. **Hilar lymphadenopathy** (often present) 5. **No cavitation** (unlike reactivation TB) ### Pathogenesis: Why Hematogenous Dissemination? ```mermaid flowchart TD A[Primary TB infection]:::outcome --> B[Caseous focus ruptures<br/>into pulmonary vessel]:::action B --> C[Hematogenous dissemination]:::action C --> D[Seeding of multiple organs]:::action D --> E[Lungs: diffuse micronodules]:::outcome D --> F[Liver, spleen, bone marrow]:::outcome D --> G[CNS: TB meningitis]:::urgent A --> H[Lymph node erosion<br/>into blood vessel]:::action H --> C ``` **Clinical Pearl:** Miliary TB can occur: - **Early dissemination**: weeks to months after primary infection (especially in children and immunocompromised) - **Late dissemination**: reactivation of old foci with erosion into vessels (as in this case — 6-month history suggests reactivation) ### Why Sputum Smear is Negative **High-Yield:** In miliary TB: - Disease is **non-cavitary** (no direct communication with airways) - Bacilli are distributed in small nodules throughout lung parenchyma - Sputum smear microscopy has low sensitivity (~10–20%) - **Diagnosis requires**: culture, GeneXpert MTB/RIF, or clinical-radiological correlation ### Comparison: Miliary vs. Cavitary TB | Feature | Miliary TB | Cavitary TB | |---------|-----------|-------------| | **Sputum smear** | Negative (usually) | Positive (highly infectious) | | **Nodule size** | 1–3 mm micronodules | Large opacity with lucency | | **Distribution** | Bilateral, diffuse, symmetrical | Unilateral, upper lobe | | **Cavitation** | Absent | Present | | **Infectivity** | Low (non-cavitary) | High (cavitary) | | **Pathogenesis** | Hematogenous dissemination | Reactivation with local spread | | **Prognosis** | Worse if untreated (high mortality) | Better with treatment | ### HRCT Findings in Miliary TB **Key Point:** HRCT is more sensitive than CXR for detecting miliary pattern: - **Centrilobular distribution** of nodules (as in this case) - Nodules may be difficult to see on plain CXR but obvious on HRCT - Random distribution throughout both lungs - No upper lobe predominance as marked as in reactivation TB **Mnemonic:** **MILIARY** features: - **M**icronodules (1–3 mm) - **I**nfectious (TB bacilli) - **L**ung involvement (bilateral) - **I**mmunocompromised risk (though can occur in immunocompetent) - **A**cute to subacute presentation - **R**apid progression if untreated - **Y**ield of sputum smear low ### Diagnostic Approach ```mermaid flowchart TD A[Bilateral micronodules<br/>+ hilar LAD<br/>+ constitutional symptoms]:::outcome --> B{Sputum smear?}:::decision B -->|Positive| C[Cavitary TB or<br/>endobronchial TB]:::outcome B -->|Negative| D{HRCT findings?}:::decision D -->|Centrilobular nodules<br/>1-3mm| E[Miliary TB]:::outcome D -->|Other pattern| F[Consider sarcoidosis,<br/>hypersensitivity pneumonitis]:::outcome E --> G[Confirm with:<br/>Culture, GeneXpert,<br/>TB-IGRA]:::action ``` [cite:Robbins 10e Ch 8; Harrison 21e Ch 205] 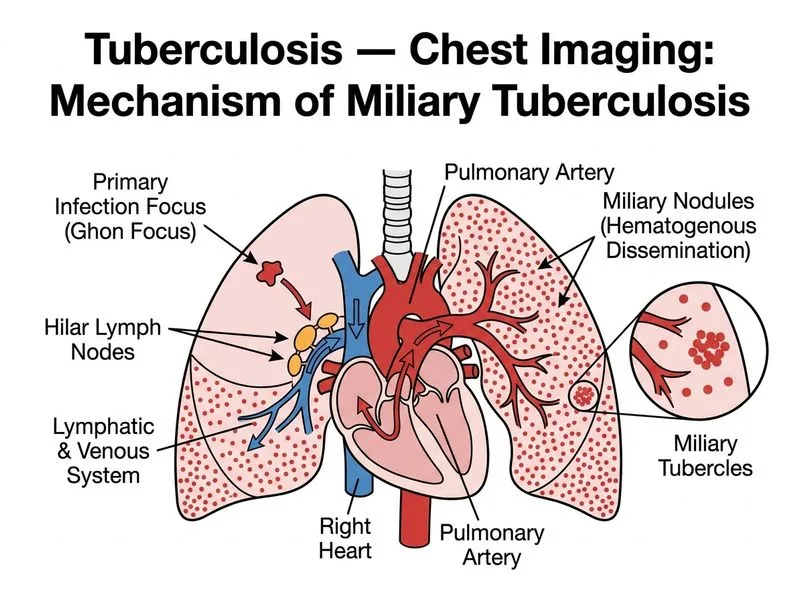
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.