## Radiological Features of Active Pulmonary Tuberculosis ### Cavitary Disease as a Hallmark of Active TB **Key Point:** Cavitation is the most characteristic radiological finding of active (infectious) pulmonary tuberculosis and indicates tissue necrosis with viable bacilli within the cavity. **High-Yield:** Cavities in TB are typically: - Located in the **apical and posterior segments of the upper lobes** (due to high oxygen tension) - Have **irregular, shaggy margins** (not smooth like in fungal or malignant cavities) - Associated with **surrounding consolidation** and satellite nodules - Often accompanied by **bronchial spread** to lower lobes ### Why Cavitation Indicates Active Disease Cavitation occurs due to: 1. Caseous necrosis of infected lung parenchyma 2. Rupture of necrotic material into the bronchial tree 3. Drainage of liquefied caseous material, leaving an air-filled cavity 4. High bacterial load within the cavity (bacilli thrive in the aerobic environment) **Clinical Pearl:** A patient with cavitary TB is highly infectious because the cavity communicates with the bronchial tree, allowing aerosolization of bacilli during coughing. ### Radiological Differential of Cavitary Lesions | Feature | TB Cavity | Fungal Cavity | Malignant Cavity | Lung Abscess | |---------|-----------|---------------|------------------|---------------| | Margin | Irregular, shaggy | Smooth, thick-walled | Irregular, thick | Irregular, air-fluid level | | Location | Upper lobe apical/posterior | Upper lobe | Any lobe | Dependent areas | | Associated findings | Satellite nodules, bronchial spread | Fungal ball | Pleural involvement | Fever, putrid sputum | | Wall thickness | Thin to moderate | Thick | Thick | Variable | **Mnemonic: CAVITY** — **C**aseous necrosis, **A**pical location, **V**iable bacilli, **I**rregular margins, **T**issue destruction, **Y**ield high bacterial load ### Why Other Findings Are Secondary - **Nodular opacities** alone suggest early/minimal disease or hematogenous spread but do not confirm active disease - **Hilar lymphadenopathy** is more typical of primary TB (children, immunocompromised) or endobronchial disease - **Pleural effusion** indicates TB pleuritis but is not the hallmark of active pulmonary TB [cite:Robbins 10e Ch 8] 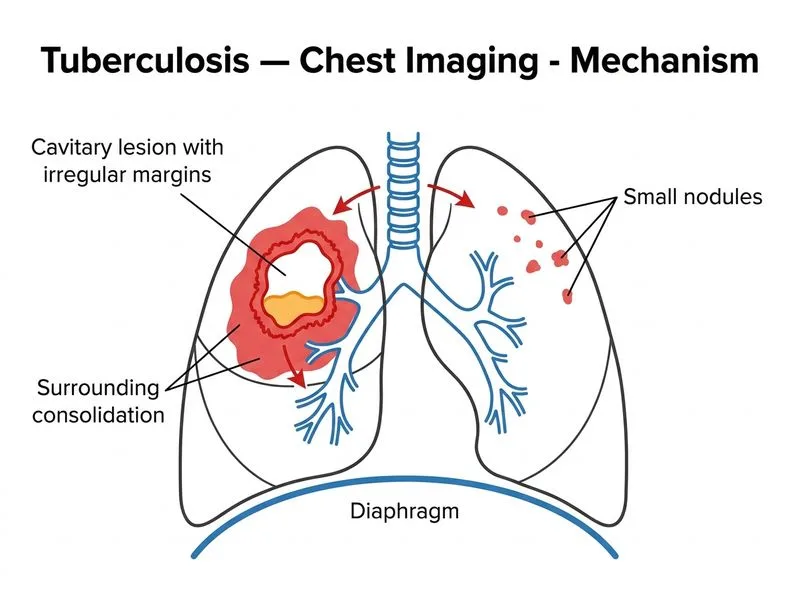
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.