## Distinguishing Primary vs Reactivation TB on Chest X-ray **Key Point:** The hallmark radiological difference between primary and reactivation TB lies in the pattern and distribution of findings, not the presence of individual features like cavitation. ### Primary Tuberculosis (Ghon Complex) - **Hilar and mediastinal lymphadenopathy** is the dominant finding - Minimal or no parenchymal consolidation - Lymph node enlargement often exceeds the size of the parenchymal lesion - Occurs within 3–8 weeks of infection - More common in children and immunocompromised individuals ### Reactivation Tuberculosis - **Apical and posterior segment consolidation** (upper lobes) is the hallmark - Cavitation is common (present in ~50% of cases) - Minimal lymphadenopathy - Occurs months to years after primary infection - More common in adults with waning immunity **High-Yield:** Lymphadenopathy **without** significant parenchymal disease = **Primary TB**. Cavitary apical consolidation **without** lymphadenopathy = **Reactivation TB**. ### Comparison Table | Feature | Primary TB | Reactivation TB | | --- | --- | --- | | **Lymphadenopathy** | Prominent (hilar/mediastinal) | Minimal or absent | | **Parenchymal consolidation** | Minimal | Extensive (apical/posterior) | | **Cavitation** | Rare | Common (50%) | | **Distribution** | Any lobe | Upper lobes (apical/posterior) | | **Age group** | Children, immunocompromised | Adults | | **Timeline** | 3–8 weeks post-infection | Months–years post-infection | **Clinical Pearl:** A child with TB and prominent hilar lymphadenopathy but minimal lung parenchymal disease is classic primary TB. An adult with cavitary apical consolidation and no lymphadenopathy is classic reactivation TB. **Warning:** Cavitation can occur in primary TB (especially in immunocompromised patients), so its presence alone does NOT distinguish the two forms. Lymphadenopathy pattern is the most reliable discriminator. 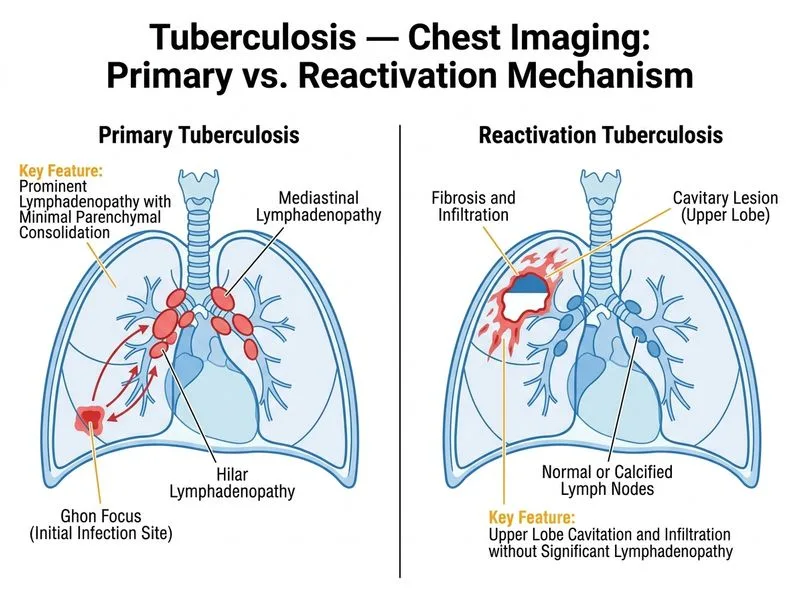
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.