## Late-Onset Pott Paraplegia: Pathophysiology and Management ### Clinical Scenario Analysis This patient has completed adequate anti-tuberculous therapy (9 months) but shows **no improvement in paraplegia**. The key imaging findings are: - Severe kyphotic deformity (70°) - Anterior subluxation - Cord atrophy - Destruction of multiple vertebral bodies These features indicate **late-onset Pott paraplegia**, a distinct entity from early-onset paraplegia. ### Classification of Pott Paraplegia | Feature | Early-Onset | Late-Onset | |---------|-------------|------------| | **Timing** | During active disease (0–2 yrs) | Years after cure (5–20+ yrs) | | **Mechanism** | Inflammatory edema, abscess, granulation tissue | Mechanical: kyphosis, subluxation, cord atrophy, fibrosis | | **ATT Response** | 80–90% respond to ATT alone | Resistant to ATT; requires surgery | | **Imaging** | Abscess, edema, inflammation | Severe kyphosis, cord atrophy, fibrosis | | **Treatment** | ATT + monitoring | Surgical decompression & fusion | ### Mechanism of Late-Onset Paraplegia **Key Point:** Late-onset Pott paraplegia is **mechanical**, not inflammatory. The cord deficit results from: 1. **Severe kyphotic deformity** (>60°) causing chronic stretch and ischemia 2. **Anterior subluxation** with direct compression from bony ridges 3. **Cord atrophy and gliosis** from chronic compression and vascular insufficiency 4. **Tethering** of the cord by fibrosis 5. **Vascular compromise** from stretching of spinal arteries **High-Yield:** The cord becomes **irreversibly damaged** (atrophic) by the time late-onset paraplegia develops. This is why ATT alone is ineffective—the damage is structural, not inflammatory. ### Why This Patient Requires Surgery **Clinical Pearl:** Late-onset Pott paraplegia is the **primary indication for surgical intervention** in Pott disease. Surgical goals: - Correct kyphosis (reduce mechanical stretch) - Decompress cord (remove bony ridges, subluxation) - Stabilize spine (prevent further deformity progression) - Fusion to prevent recurrent deformity Surgical outcomes in late-onset paraplegia are modest (30–50% neurological improvement) because cord atrophy is irreversible, but surgery prevents further deterioration. ### Why Other Options Are Incorrect - **Inflammatory edema and abscess** (Option A) would respond to ATT. This patient has already completed 9 months of therapy with no improvement, ruling out active inflammation as the primary mechanism. - **Reactivation of TB** (Option C) is unlikely after 9 months of adequate therapy; moreover, reactivation would present with new systemic symptoms and imaging would show new abscess formation, not cord atrophy. - **Spinal cord infarction from vasculitis** (Option D) is a rare complication of TB; it does not explain the chronic kyphotic deformity or cord atrophy seen here. ```mermaid flowchart TD A["Pott Disease Paraplegia"]:::outcome --> B{"Timing & Mechanism?"}:::decision B -->|"Early-onset: Inflammatory<br/>0-2 years, edema/abscess"| C["ATT + Monitoring"]:::action B -->|"Late-onset: Mechanical<br/>5-20+ years, kyphosis/atrophy"| D["Surgical Decompression<br/>& Fusion"]:::action C --> E{"Improvement?"}:::decision E -->|"Yes"| F["Continue ATT"]:::outcome E -->|"No"| G["Reassess for late-onset<br/>features; consider surgery"]:::urgent D --> H["Correct kyphosis,<br/>decompress cord"]:::action H --> I["Prevent further<br/>deterioration"]:::outcome ``` [cite:Campbell's Operative Orthopaedics 13e Ch 63; Robbins & Cotran Pathologic Basis of Disease 10e Ch 8] 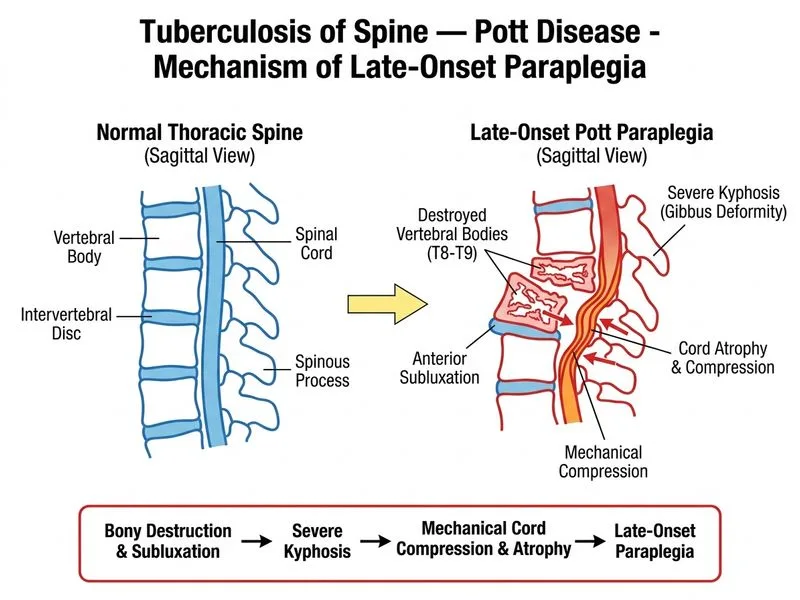
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.