## Management of Pott Disease with Neurological Involvement ### Clinical Context This patient has active tuberculosis of the spine (Pott disease) with: - Multi-level vertebral body destruction (T5–T6) - Anterior wedging and kyphotic deformity - Epidural extension with cord compression - Active systemic TB (apical infiltrates on CXR) ### Treatment Algorithm ```mermaid flowchart TD A[Pott Disease Diagnosed]:::outcome --> B{Neurological Deficit?}:::decision B -->|Yes, Active| C[Start Anti-TB Therapy Immediately]:::action B -->|No| D[Anti-TB Therapy + Monitoring]:::action C --> E{Neuro Deterioration on Therapy?}:::decision E -->|Yes| F[Surgical Intervention: Anterior Decompression ± Fusion]:::action E -->|No| G[Continue Medical Management]:::action D --> H[Reassess at 3-6 months]:::action ``` ### Key Point: Medical Management is First-Line **Anti-tuberculous therapy (4-drug regimen: HRZE for 2 months, then HR for 4 months minimum) is the cornerstone of treatment**, even with cord compression. Most patients improve with medical therapy alone due to: - Inflammatory edema resolution (major component of cord compression) - Gradual healing of vertebral bodies - Abscess resorption ### High-Yield: Indications for Surgery in Pott Disease | Indication | Timing | Rationale | |---|---|---| | **Neurological deterioration despite 6–8 weeks of ATT** | Urgent | Suggests mechanical compression or abscess | | **Severe kyphotic deformity (>60°)** | Elective, after ATT | Prevent late-onset paraplegia | | **Instability with severe destruction** | Elective | Reconstruction after disease quiescence | | **Active disease + cord compression (this case)** | Start ATT first | Edema usually resolves; reserve surgery for failure | ### Clinical Pearl: Why Not Immediate Surgery? - **Anterior corpectomy** is reserved for: - Failure to improve neurologically after 6–8 weeks of ATT - Severe kyphotic deformity requiring reconstruction - Late-onset paraplegia (years after healing) - Performing surgery during active disease increases infection risk and morbidity; healing is poor in the presence of active TB. ### High-Yield: Monitoring During Medical Therapy - **Neurological examination** every 2–4 weeks - **MRI at 3 months** to assess cord compression and vertebral healing - **Continue ATT for minimum 9–12 months** (longer for severe disease) - Surgical intervention only if neurological status worsens despite optimal ATT ### Mnemonic: POTT Management Sequence **P** — Prompt anti-TB therapy (first-line) **O** — Observe for neurological change (6–8 weeks) **T** — Treat surgically if deterioration occurs **T** — Thorough monitoring for kyphotic progression ### Warning: Common Exam Traps - ~~Immediate surgery for cord compression~~ — Medical therapy is first-line; surgery is reserved for failure or late complications. - ~~Biopsy before starting therapy~~ — If clinical + radiological suspicion is high and TB is confirmed systemically, start ATT immediately; biopsy delays critical treatment. - ~~Fusion during active disease~~ — Increases infection risk; wait for disease quiescence (usually 6–12 months). 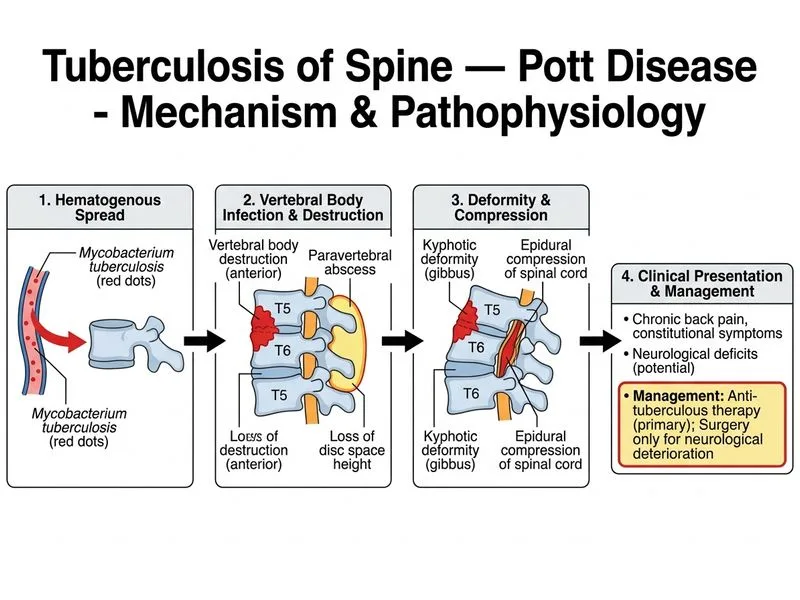
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.