## Lysinuric Protein Intolerance (LPI) — Acute Hyperammonemia Management ### Clinical Recognition The amino acid profile is pathognomonic for **lysinuric protein intolerance (LPI)**: - Elevated plasma lysine, arginine, ornithine (cannot be reabsorbed in proximal tubule) - Elevated urinary lysine, ornithine, cystine (triple aminoaciduria) - Low citrulline and argininosuccinate (secondary to arginine deficiency in urea cycle) **Key Point:** LPI is caused by a defect in the cationic amino acid transporter (y+LAT1), leading to: 1. Loss of lysine, arginine, ornithine in urine 2. Deficiency of arginine (a urea cycle substrate) → impaired ammonia detoxification 3. Secondary hyperammonemia despite a structurally intact urea cycle ### Why This Patient Needs Benzoate/Phenylbutyrate (NOT IV Arginine) Unlike OTC deficiency, where the urea cycle enzyme is blocked: - In LPI, the urea cycle is **structurally intact** but starved of arginine substrate - IV arginine will be rapidly lost in urine (due to the transporter defect) and does NOT solve the problem - **Benzoate and phenylbutyrate activate alternative nitrogen-scavenging pathways** that bypass the urea cycle: - Benzoate → hippurate (removes 1 N per glycine conjugate) - Phenylbutyrate → phenylacetylglutamine (removes 2 N per glutamine conjugate) - These are the **definitive therapy** for LPI hyperammonemia ### Management Algorithm ```mermaid flowchart TD A["Hyperammonemia + Elevated Lys/Arg/Orn + Low Cit/ASUC"]:::outcome --> B{"Urine shows triple aminoaciduria?"}:::decision B -->|Yes| C["Suspect LPI"]:::outcome C --> D["Start benzoate + phenylbutyrate"]:::action D --> E["Protein restriction"]:::action E --> F["Monitor ammonia & amino acids"]:::action B -->|No| G["Consider OTC/other urea cycle defect"]:::outcome G --> H["IV arginine + protein restriction"]:::action ``` ### Protein Restriction Rationale - Reduces nitrogen load and ammonia generation - Essential in both LPI and urea cycle defects - Protein intake adjusted based on ammonia levels and growth needs **High-Yield:** The key discriminator between LPI and OTC deficiency: | Feature | OTC Deficiency | LPI | |---------|---|---| | Urine orotic acid | Markedly elevated | Normal | | Urine amino acids | Normal | Triple aminoaciduria (Lys, Orn, Cys) | | Plasma arginine | Normal or high | Low | | Plasma citrulline | Low | Low | | First-line therapy | IV arginine | Benzoate + phenylbutyrate | **Clinical Pearl:** LPI is autosomal recessive and common in Finnish and Japanese populations. Patients often present with recurrent hyperammonemia triggered by infections or high protein intake. ### Why IV Arginine Fails in LPI - Arginine is a cationic amino acid — it cannot be reabsorbed by the defective transporter - Exogenous IV arginine is rapidly filtered and lost in urine - Does not restore intracellular arginine pools needed for urea cycle function - Benzoate/phenylbutyrate work because they activate ammonia scavenging independent of arginine availability [cite:Harrison 21e Ch 355; Robbins 10e Ch 7] 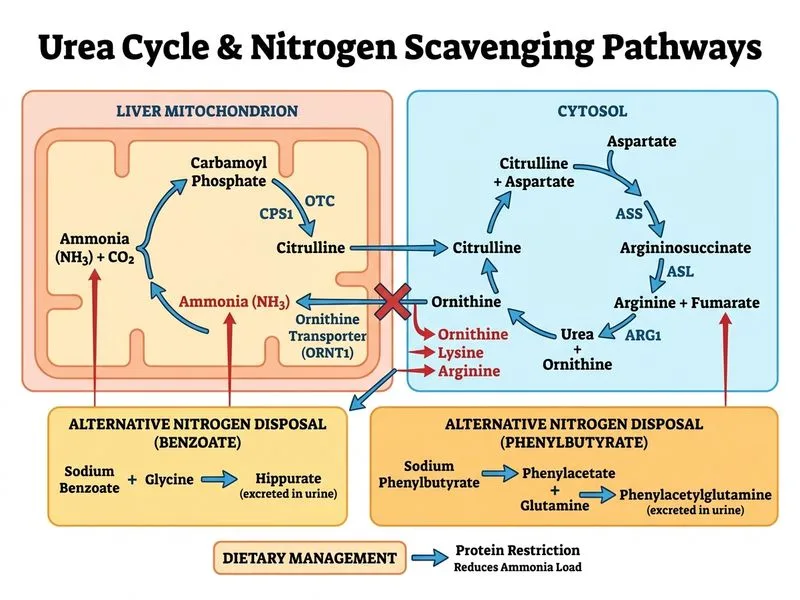
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.