## Long-Term Management of Argininosuccinate Lyase (ASL) Deficiency ### Clinical Context ASL deficiency (autosomal recessive) is the second most common urea cycle disorder. The biochemical signature is: - **Elevated citrulline** (substrate accumulates proximal to the block) - **Elevated argininosuccinate** in urine (diagnostic) - **Elevated glutamine and alanine** (secondary to hyperammonemia) - **Low arginine** (consumed by argininosuccinate synthetase; cannot be regenerated) Unlike OTC deficiency, ASL deficiency often presents later in childhood with episodic hyperammonemia triggered by protein intake, infections, or stress. ### Rationale for Correct Answer **Key Point:** Long-term management of urea cycle defects requires a three-pillar approach: protein restriction, arginine supplementation, and regular biochemical monitoring. #### 1. Protein Restriction (1.2–1.5 g/kg/day) - Reduces ammonia generation from amino acid catabolism - In children, must be balanced against growth requirements (higher than in adults) - Typically 1.2–1.5 g/kg/day for school-age children; adjust based on ammonia levels and growth - Avoid protein restriction <0.8 g/kg/day in growing children (risk of malnutrition and developmental delay) #### 2. Arginine Supplementation (100–200 mg/kg/day) - **Critical in ASL deficiency:** arginine is depleted because it is consumed by argininosuccinate synthetase and cannot be regenerated past the enzymatic block - Arginine is a semi-essential amino acid in urea cycle defects - Supplementation: - Activates carbamoyl phosphate synthetase I (CPSI) - Restores partial urea cycle flux - Prevents arginine deficiency (which impairs immune function, wound healing, and growth) #### 3. Regular Biochemical Monitoring - **Plasma ammonia:** every 3 months or when symptoms develop (target <100 µmol/L) - **Plasma amino acids:** every 3–6 months (assess glutamine, citrulline, arginine balance) - **Urine orotic acid or argininosuccinate:** annually (marker of urea cycle flux) - **Growth and neurodevelopment:** assess at each visit **High-Yield:** ASL deficiency often has a better prognosis than OTC deficiency if managed early and aggressively. Intellectual disability is less common if ammonia is kept <150 µmol/L. ### Biochemical Pathway in ASL Deficiency ```mermaid flowchart TD A[Ammonia + Carbamoyl phosphate]:::outcome --> B[CPSI]:::action B --> C[Citrulline]:::outcome C --> D[Argininosuccinate synthetase]:::action D --> E[Argininosuccinate]:::outcome F[ASL Block]:::urgent -.-> E E --> G[Argininosuccinate lyase]:::action G --> H[Arginine]:::outcome H --> I[Arginase]:::action I --> J[Urea + Ornithine]:::outcome K[Arginine supplementation]:::action -.-> H L[Protein restriction]:::action -.-> A M[Regular monitoring]:::action -.-> N[Ammonia, amino acids, growth]:::outcome ``` **Clinical Pearl:** In ASL deficiency, citrulline accumulates in urine and plasma (diagnostic finding). Unlike OTC deficiency, orotic acid is only mildly elevated because carbamoyl phosphate can still enter the urea cycle proximal to the block. [cite:Harrison 21e Ch 355] --- ## Why Each Distractor is Wrong | Option | Reason | | --- | --- | | **Protein <0.5 g/kg/day + avoid arginine** | Severe protein restriction (<0.8 g/kg/day) in a growing child causes malnutrition, poor growth, and developmental delay. More importantly, arginine MUST be supplemented in ASL deficiency because it is depleted (consumed by argininosuccinate synthetase and not regenerated). Avoiding arginine would worsen immune function, wound healing, and growth. This option confuses ASL deficiency with other urea cycle disorders. | | **Ursodeoxycholic acid + LFT monitoring** | Ursodeoxycholic acid is used in cholestatic liver disease, not urea cycle defects. While cirrhosis can develop in untreated urea cycle disorders (from chronic hyperammonemia), the primary management is ammonia control, not hepatoprotection. This option misses the biochemical basis of the disease. | | **Genetic counseling + discharge without dietary intervention** | Genetic counseling is appropriate for family planning but is NOT a substitute for long-term dietary and pharmacological management. Discharging without protein restriction and arginine supplementation would result in recurrent hyperammonemic crises, seizures, and progressive neurological damage. This option is dangerously inadequate. | --- ## Summary Table: Urea Cycle Defects — Long-Term Management | Defect | Enzyme | Key Finding | Protein Restriction | Arginine | Other | | --- | --- | --- | --- | --- | --- | | **OTC** | Ornithine transcarbamylase | ↑ Orotic acid, ↑ Carbamoyl phosphate | 1–1.5 g/kg/day | 100–600 mg/kg/day | Benzoate/phenylbutyrate | | **ASL** | Argininosuccinate lyase | ↑ Citrulline, ↑ Argininosuccinate | 1.2–1.5 g/kg/day | **100–200 mg/kg/day (essential)** | Monitor growth closely | | **CPS I** | Carbamoyl phosphate synthetase I | ↑ Glutamine, normal orotic acid | 1–1.5 g/kg/day | 100–600 mg/kg/day | Benzoate/phenylbutyrate | | **Arginase** | Arginase | ↑ Arginine, ↑ Lysine | 1.2–1.5 g/kg/day | Restrict arginine | Spasticity common | [cite:KD Tripathi 8e Ch 39] --- 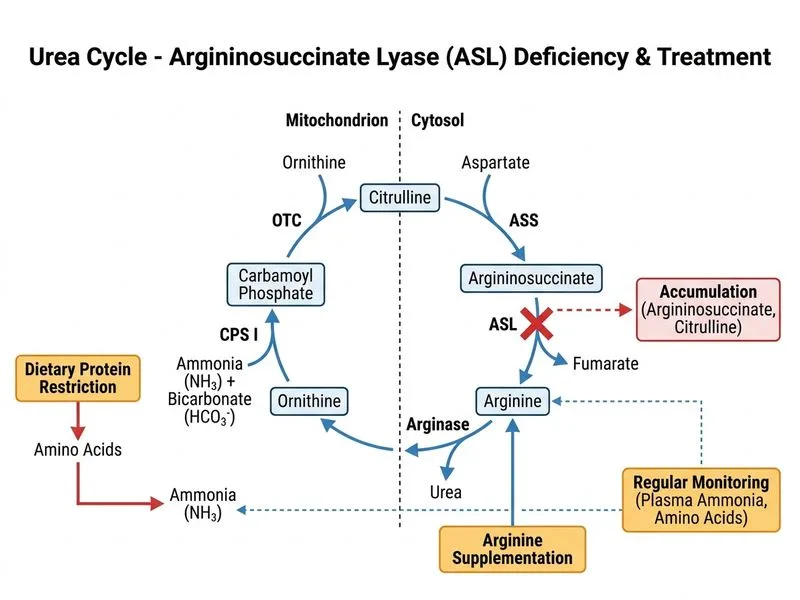
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.